In this article, you will explore the dynamic relationship between healthcare policy and telemedicine and digital health. With the rapid advancements in technology and the growing popularity of virtual healthcare services, understanding how healthcare policy influences these fields is crucial. From regulations and reimbursement policies to privacy and security concerns, the impact of healthcare policy on telemedicine and digital health is far-reaching. Join us as we navigate this fascinating intersection and uncover the implications for the future of healthcare delivery.
Overview of Healthcare Policy
Definition and significance of healthcare policy
Healthcare policy refers to a set of rules, regulations, and guidelines that govern the delivery, funding, and accessibility of healthcare services. It encompasses various aspects, such as healthcare financing, insurance coverage, provider reimbursement, and quality assurance. Healthcare policy plays a crucial role in shaping the healthcare landscape, as it has a direct impact on the availability and affordability of healthcare services for individuals and communities.
Current state of healthcare policy
Currently, healthcare policy is undergoing significant changes and transformations due to various socio-economic factors and advancements in technology. Governments and organizations around the world are striving to develop policies that address the evolving healthcare needs of their populations while ensuring the efficient utilization of resources. Additionally, there is a growing recognition of the importance of telemedicine and digital health in modern healthcare systems, which is leading to policy changes to facilitate their implementation and integration.
Telemedicine and Digital Health
Explanation and importance of telemedicine
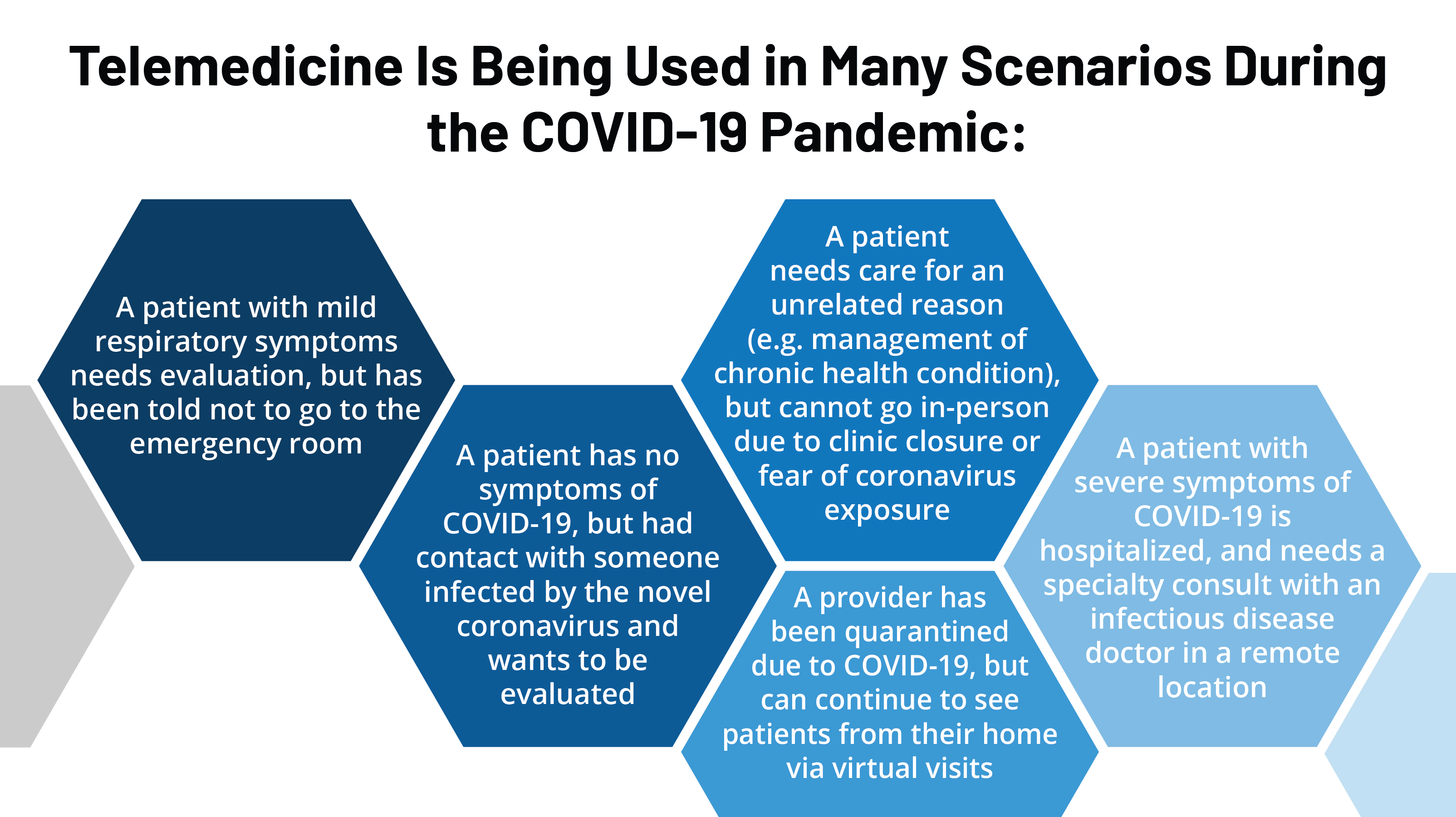
Telemedicine refers to the use of telecommunications technology to provide healthcare services remotely. It allows patients to consult with healthcare professionals, receive diagnoses, and receive treatment without the need for in-person visits. Telemedicine has emerged as a powerful tool in expanding access to healthcare, especially for individuals in remote areas or those with limited mobility. It has the potential to revolutionize the way healthcare is delivered by bridging geographical barriers and improving efficiency.
Overview of digital health technologies
Digital health technologies encompass a wide range of tools and applications that leverage digital platforms to improve healthcare delivery, patient engagement, and clinical outcomes. These technologies include mobile health apps, wearable devices, remote monitoring systems, electronic health records, and artificial intelligence (AI)-powered diagnostic tools. They contribute to the transformation of healthcare by enabling real-time data collection, seamless communication between patients and healthcare providers, and personalized care.
Impact of Healthcare Policy on Telemedicine
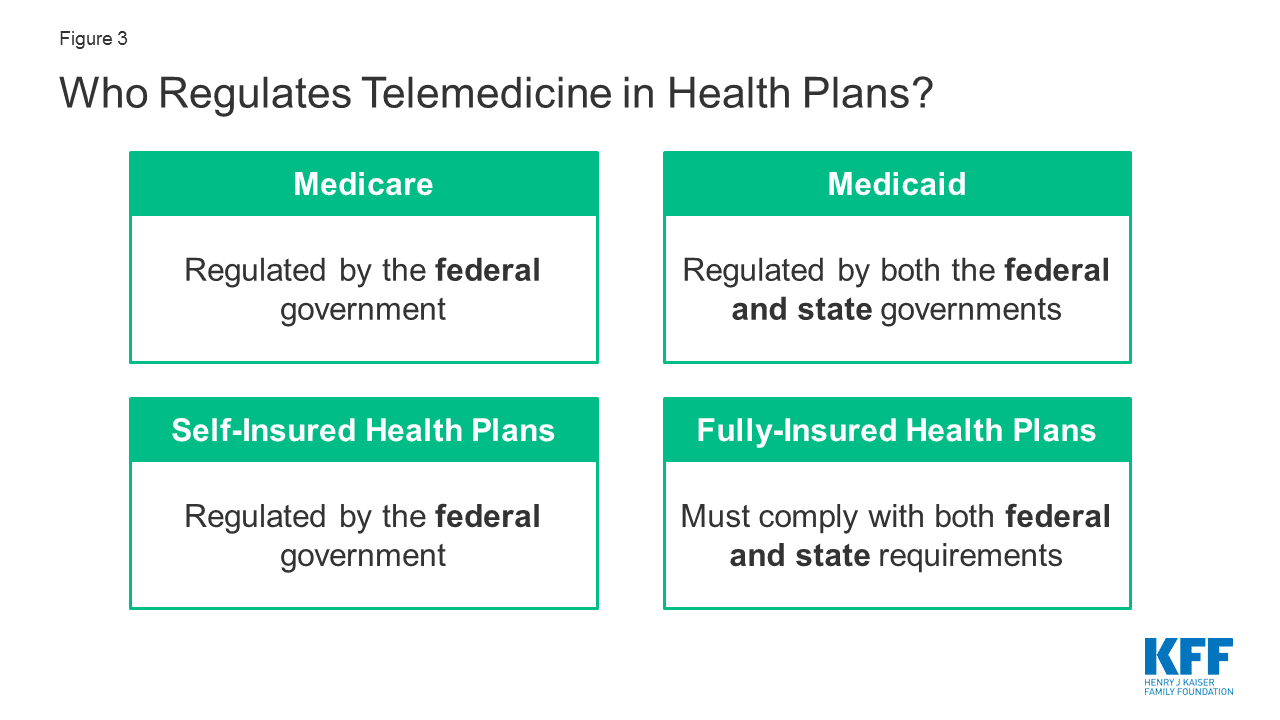
Regulations and guidelines for telemedicine
The regulations and guidelines governing telemedicine vary across countries and regions. These policies aim to ensure patient safety, maintain privacy and security, and establish standards for telemedicine practices. They often include requirements for licensure and credentialing of healthcare professionals providing telemedicine services, reimbursement policies, and guidelines for the appropriate use of telemedicine technologies. Healthcare policy plays a crucial role in shaping these regulations, which can either facilitate or hinder the adoption and implementation of telemedicine.
Access and affordability of telemedicine services
Healthcare policy has a significant impact on the access and affordability of telemedicine services. Policies that recognize telemedicine as a viable and reimbursable mode of healthcare delivery can lead to increased access for underserved populations. Additionally, policies that promote equitable reimbursement for telemedicine services, including coverage by public and private insurance providers, can make telemedicine more affordable for patients. However, barriers such as restrictive licensure requirements and limitations in telemedicine reimbursement can hinder the widespread adoption of telemedicine.
Integration of telemedicine into healthcare systems
The integration of telemedicine into healthcare systems is influenced by healthcare policy. Policy initiatives that promote the seamless integration of telemedicine technologies with existing healthcare infrastructure can lead to more efficient and coordinated care. This integration requires collaboration among policymakers, healthcare providers, and technology companies to establish interoperability standards, ensure data privacy and security, and address administrative and legal challenges. Healthcare policy can also influence the implementation of telemedicine at different levels of care, such as primary care, specialty care, and emergency services.
Benefits of Telemedicine and Digital Health
Improved access to healthcare services
Telemedicine has the potential to significantly improve access to healthcare services, particularly for individuals residing in remote areas or facing transportation barriers. Through telemedicine, patients can access medical consultations, receive diagnoses, and obtain prescriptions from the comfort of their homes. This increased accessibility reduces the need for in-person visits and allows healthcare services to reach underserved populations, ultimately improving health outcomes.
Enhanced patient convenience and satisfaction
Telemedicine offers convenience and flexibility to patients by eliminating the need for travel and reducing waiting times. Patients can schedule virtual appointments at their convenience and avoid long waits in crowded waiting rooms. Additionally, telemedicine allows patients to receive care from the comfort of their home, reducing the stress and inconvenience associated with traditional visits. This convenience leads to higher patient satisfaction rates and improved overall healthcare experiences.
Reduction in healthcare costs
Telemedicine has the potential to significantly reduce healthcare costs. By leveraging digital technologies, telemedicine eliminates the need for costly in-person consultations, travel expenses, and infrastructure investments. It streamlines care delivery processes, reduces administrative burdens, and optimizes resource utilization. Additionally, telemedicine enables early detection and intervention, which can prevent costly complications and hospital admissions. As a result, healthcare organizations and individuals can achieve significant cost savings through the implementation of telemedicine.
Opportunities for remote monitoring and chronic disease management
Telemedicine offers opportunities for remote monitoring of patients, especially those with chronic conditions. With the help of wearable devices and remote monitoring systems, healthcare providers can collect real-time data on patients’ vital signs, medication adherence, and disease progression. This allows for proactive interventions, timely adjustments in treatment plans, and early detection of potential complications. Telemedicine also enables patients to actively participate in their own care, promoting self-management and empowering individuals to take control of their health.

Challenges and Limitations
Lack of standardized policies and legal frameworks
One of the primary challenges in the implementation of telemedicine is the lack of standardized policies and legal frameworks across jurisdictions. Varying regulations and licensing requirements for telemedicine hinder the seamless delivery of care across state lines or international borders. Policymakers need to collaboratively establish clear guidelines and frameworks that ensure patient safety, protect privacy and security, and facilitate the licensure and credentialing of telemedicine providers.
Technological barriers and infrastructure requirements
Despite the rapid advancements in digital health technologies, there are still technological barriers that hinder the widespread adoption of telemedicine. Inadequate internet connectivity, particularly in rural or underserved areas, limits the accessibility and reliability of telemedicine services. Lack of interoperability between different telemedicine platforms and electronic health record systems also poses challenges in seamless data exchange and care coordination. Healthcare policy must address these technological barriers and invest in infrastructure development to ensure the availability of robust and reliable telemedicine services.
Privacy and security concerns
Telemedicine introduces unique privacy and security challenges due to the remote nature of care provision and the electronic transmission of sensitive patient information. Healthcare policy needs to establish comprehensive data protection regulations and standards for telemedicine platforms, ensuring the encryption and secure storage of patient data. Additionally, clear consent procedures and guidelines for patient information sharing within telemedicine networks should be in place to safeguard patient privacy and maintain trust in telemedicine services.
Resistance to change among healthcare providers
The adoption of telemedicine may face resistance from healthcare providers who are accustomed to traditional in-person care delivery. Some providers may express concerns about the quality of care, loss of personal interaction with patients, and implications for their professional autonomy. Healthcare policy can play a role in addressing these concerns by providing support, training, and incentives for healthcare providers to embrace telemedicine. Policies that prioritize the integration of telemedicine into medical education and professional development programs can enhance provider acceptance and uptake.
Case Studies and Success Stories
Examples of successful telemedicine implementation
Numerous case studies demonstrate the successful implementation of telemedicine across different healthcare settings. For example, in rural areas of Australia, the Royal Flying Doctor Service utilizes telemedicine to provide specialist consultations, emergency support, and virtual healthcare outreach. This has significantly improved access to specialized care for remote populations. Similarly, the Veterans Health Administration (VHA) in the United States has successfully integrated telemedicine into its healthcare system, offering telehealth services for primary care, mental health, and rehabilitation, resulting in improved patient outcomes and cost savings.
Positive outcomes and impact on patient care
Telemedicine has shown promising results in improving patient care outcomes across various clinical areas. Studies have shown that telemedicine interventions in chronic disease management lead to better patient adherence to treatment plans, reduced hospitalization rates, and improved overall health outcomes. In mental health, telepsychiatry has been effective in extending care to individuals with limited access to mental health services and has demonstrated comparable clinical outcomes to traditional in-person care. These success stories highlight the potential of telemedicine to enhance patient care and transform healthcare delivery.
Potential Future Developments
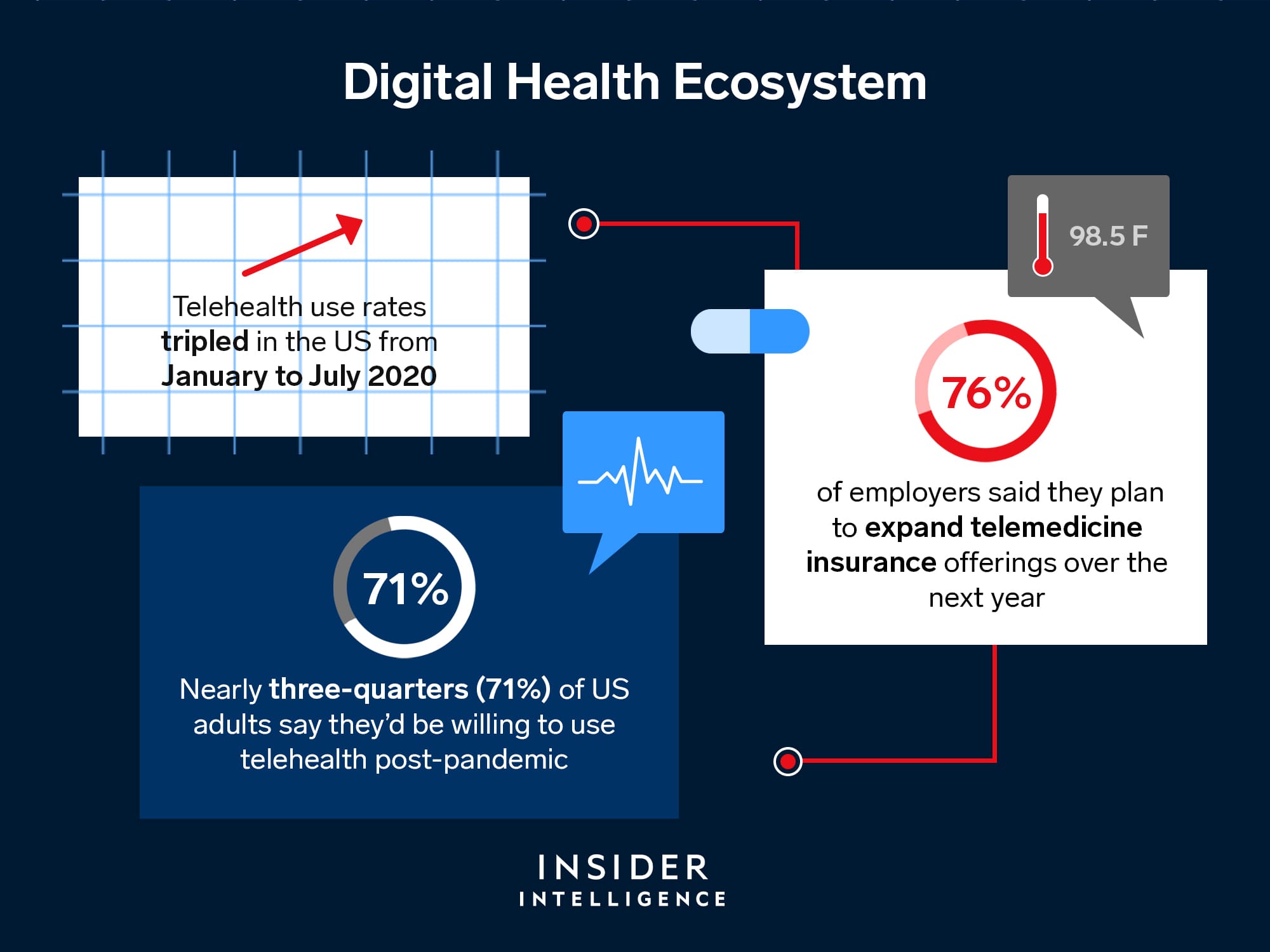
Advancements in digital health technologies
The field of digital health is rapidly evolving, driven by technological advancements and innovative applications. New digital health technologies, such as AI-powered diagnostic tools, remote patient monitoring systems, and virtual reality-based therapies, hold great promise for improving healthcare outcomes and patient experiences. As these technologies continue to advance, healthcare policy needs to adapt to enable their integration into healthcare systems and ensure their safe and effective use.
Evolution of healthcare policies for telemedicine
Healthcare policies are expected to evolve to keep pace with the increasing adoption of telemedicine. Governments and regulatory bodies are recognizing the importance of telemedicine in improving access to care and achieving healthcare system efficiencies. Policies may expand reimbursement models, ease licensing requirements, and establish guidelines for telemedicine service standards. The continued evolution of healthcare policies for telemedicine will be crucial in creating an enabling environment for its widespread implementation.
Integration of artificial intelligence and machine learning in telemedicine
Artificial intelligence (AI) and machine learning have the potential to revolutionize telemedicine by enabling more accurate diagnoses, personalized treatment plans, and predictive analytics for disease management. AI-powered algorithms can analyze vast amounts of healthcare data and generate insights to support clinical decision-making. However, the integration of AI into telemedicine raises ethical and policy considerations regarding transparency, accountability, and potential biases. Healthcare policy must ensure the ethical and responsible use of AI technologies in telemedicine, striking a balance between innovation and patient safety.
Policy Considerations for Effective Implementation
Collaboration among policymakers, healthcare providers, and technology companies
Effective implementation of telemedicine requires collaboration among policymakers, healthcare providers, and technology companies. Policymakers need to engage with healthcare professionals to understand their needs and concerns and develop policies that address these issues. Collaboration with technology companies can help ensure that telemedicine technologies are user-friendly, secure, and aligned with healthcare needs. By creating a collaborative ecosystem, policymakers can foster an environment conducive to the successful implementation of telemedicine initiatives.
Addressing privacy and security concerns
Privacy and security concerns are paramount in telemedicine. Healthcare policy needs to establish clear regulations and standards for data protection, encryption, and secure transmission of patient information. Policies should also address consent procedures, patient rights, and data breach reporting requirements. By ensuring robust privacy and security measures, healthcare policy can help build trust and confidence in telemedicine, encouraging its adoption and use.
Investment in telemedicine infrastructure and training
Infrastructure development is essential for the successful implementation of telemedicine. Policies should prioritize investments in broadband connectivity, telecommunication networks, and technological infrastructure to support the reliable and seamless delivery of telemedicine services. Additionally, healthcare policy should allocate resources for training healthcare professionals in telemedicine practices, ensuring their competence and confidence in providing virtual care. Adequate funding and supportive policies can accelerate the development of telemedicine infrastructure and education, facilitating its widespread adoption.
Promoting equitable access to telemedicine services
Healthcare policy should prioritize equitable access to telemedicine services, particularly for underserved populations. Policies should address disparities in access to technology, internet connectivity, and healthcare resources that hinder access to telemedicine. Initiatives such as subsidized telecommunication services, mobile health units, and telemedicine outreach programs can help bridge these gaps and ensure that all individuals have equal opportunities to benefit from telemedicine. By promoting equitable access, healthcare policy can contribute to reducing healthcare disparities and improving population health outcomes.
Conclusion
Healthcare policy plays a central role in shaping the implementation and impact of telemedicine and digital health technologies. By establishing regulations, guidelines, and support structures, healthcare policy can facilitate the widespread adoption and integration of telemedicine into healthcare systems. Telemedicine offers numerous benefits, including improved access to care, enhanced patient convenience, cost savings, and opportunities for remote monitoring and chronic disease management. However, challenges such as standardized policies, technological barriers, privacy concerns, and provider resistance need to be addressed for telemedicine to reach its full potential. Through collaboration, investment in infrastructure, and equitable access, healthcare policy can contribute to the continued development and success of telemedicine initiatives. Continued support and development of telemedicine policies are essential to unlock the full potential of telemedicine in transforming healthcare delivery and improving patient outcomes.