Hello there! In this comprehensive guide, you’ll find everything you need to know about managing diabetes. From creating a balanced meal plan to the importance of regular exercise, we’ll cover all the essential tips and strategies to help you live a healthy and fulfilling life with diabetes. Get ready to take charge of your health and empower yourself with the knowledge and tools to effectively manage your diabetes. Let’s dive in!
Managing Diabetes: A Complete Guide
Have you or a loved one recently been diagnosed with diabetes? Managing diabetes can seem overwhelming at first, but with the right tools and knowledge, you can take control of your health and lead a fulfilling life. This complete guide will provide you with the information and resources you need to navigate the complexities of diabetes management.
Understanding Diabetes
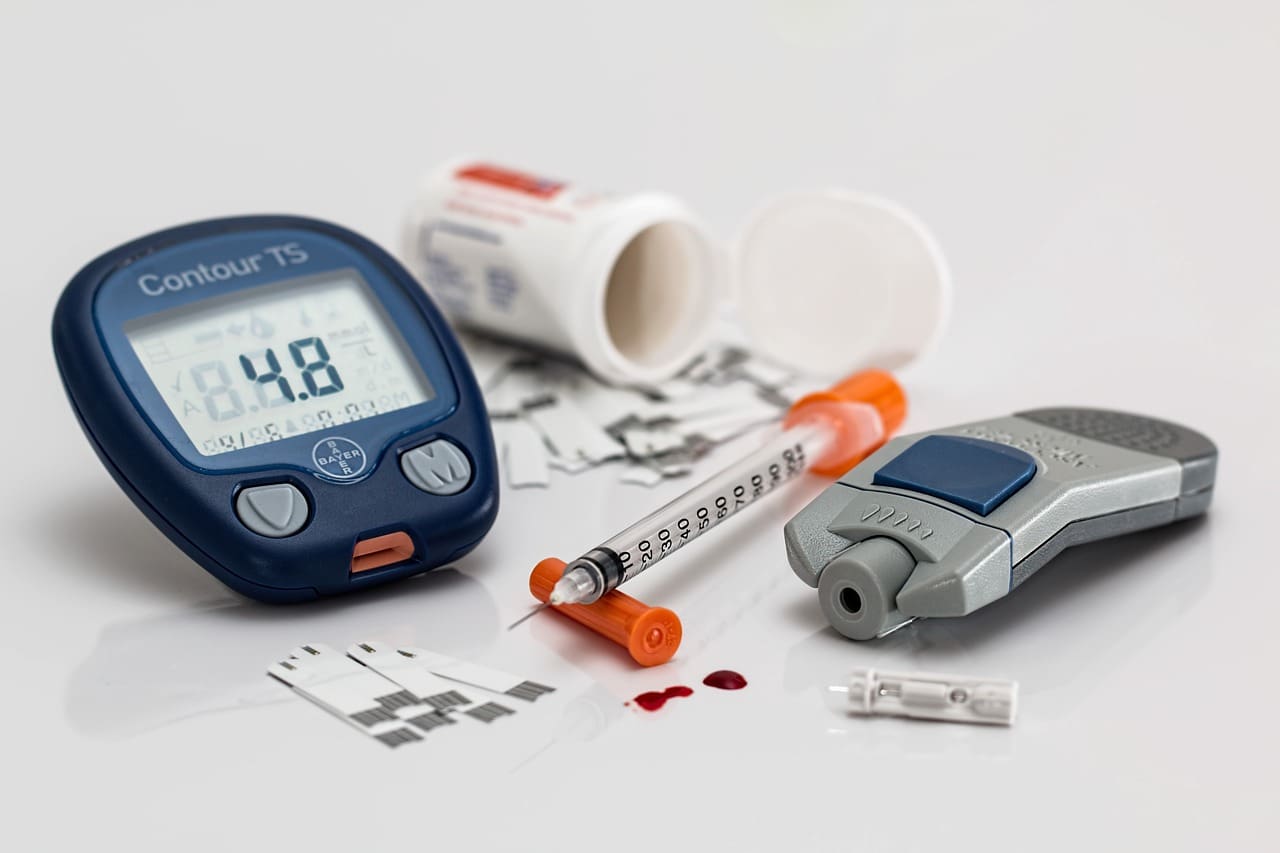
Diabetes is a chronic condition that affects how your body processes glucose, or blood sugar. It occurs when the pancreas either does not produce enough insulin or the body cannot effectively use the insulin it produces. There are two main types of diabetes: type 1 and type 2.
Type 1 diabetes is an autoimmune disease where the immune system mistakenly attacks and destroys the insulin-producing cells in the pancreas. People with type 1 diabetes must take insulin injections or use an insulin pump to manage their blood sugar levels.
Type 2 diabetes is the most common form of diabetes and is often linked to lifestyle factors such as diet and exercise. In type 2 diabetes, the body becomes resistant to insulin or does not produce enough insulin to maintain normal blood sugar levels.
How Does Diabetes Affect the Body?
Unchecked diabetes can lead to a wide range of health complications, including cardiovascular disease, kidney disease, nerve damage, and vision problems. High blood sugar levels can damage blood vessels and nerves throughout the body, leading to long-term health issues if left untreated.
Diabetes Management
Managing diabetes involves a combination of medication, lifestyle changes, and regular monitoring of blood sugar levels. By taking a holistic approach to diabetes management, you can minimize the risk of complications and improve your overall quality of life.
Medications for Diabetes
There are several types of medications used to treat diabetes, including:
- Insulin: Used to lower blood sugar levels in people with type 1 diabetes and some people with type 2 diabetes.
- Oral Medications: Including metformin, sulfonylureas, and thiazolidinediones, which help lower blood sugar levels in people with type 2 diabetes.
- Injectable Medications: Such as GLP-1 receptor agonists and SGLT2 inhibitors, which help lower blood sugar levels and promote weight loss in people with type 2 diabetes.
Your healthcare provider will work with you to determine the most appropriate medication regimen based on your individual needs and health status.
Blood Sugar Monitoring
Monitoring your blood sugar levels is a crucial aspect of diabetes management. Regular blood sugar testing can help you track how your body responds to medication, exercise, and dietary changes. Common methods of blood sugar monitoring include:
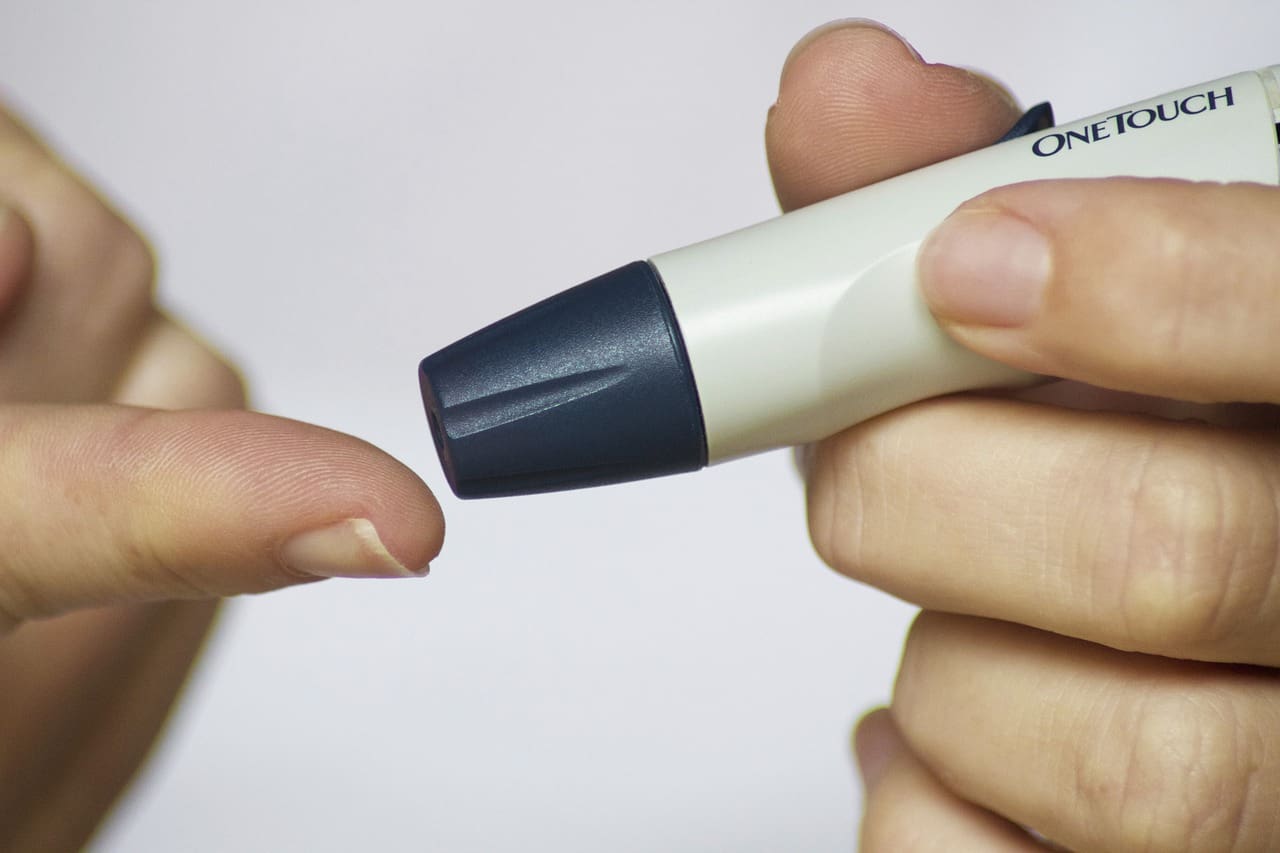
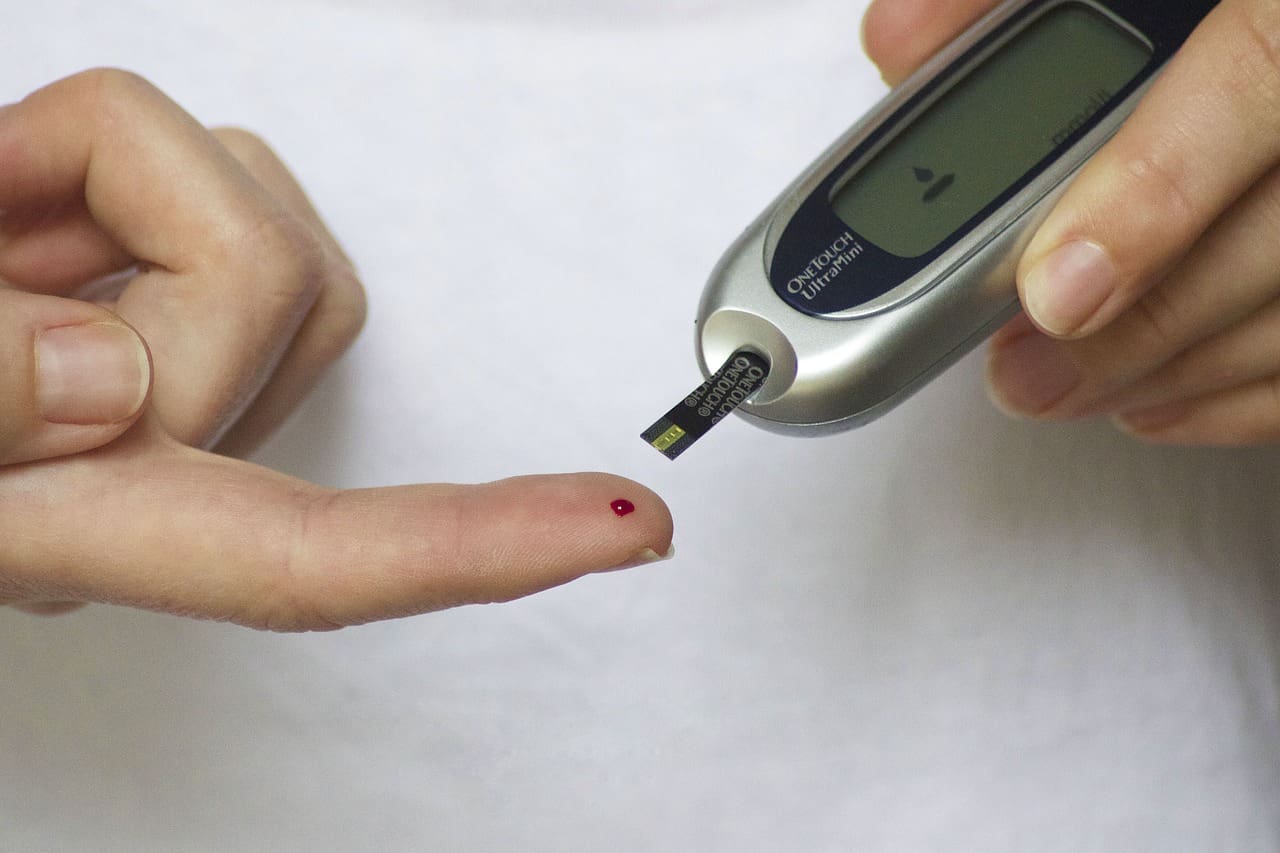
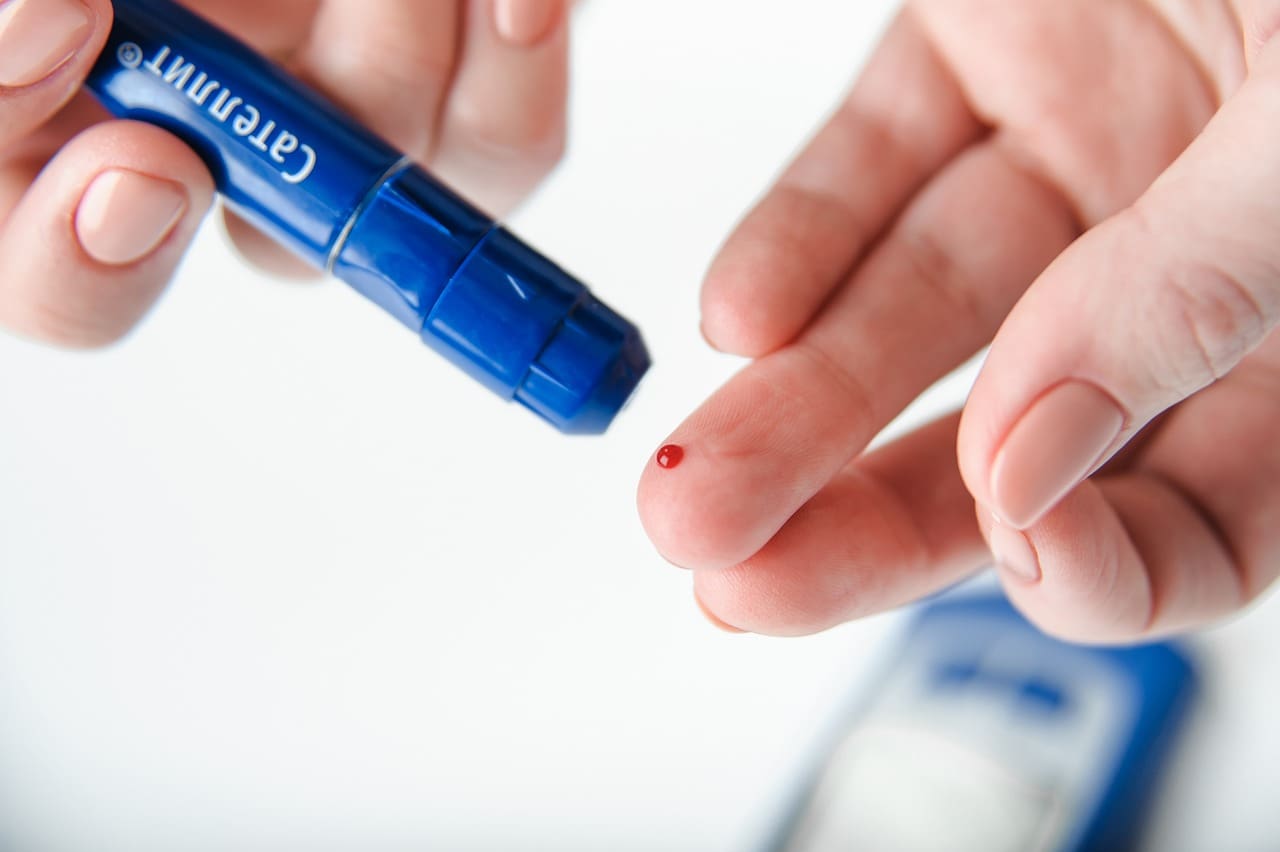
- Fingerstick Testing: Using a handheld glucose meter to check blood sugar levels several times a day.
- Continuous Glucose Monitoring (CGM): A device that tracks blood sugar levels throughout the day and sends real-time data to your smartphone or receiver.
By keeping track of your blood sugar levels regularly, you can make informed decisions about your diabetes management plan.
Nutrition and Meal Planning
Maintaining a healthy diet is essential for managing diabetes and controlling blood sugar levels. A well-balanced meal plan can help you regulate your blood sugar, maintain a healthy weight, and prevent complications associated with diabetes. Some key nutrition tips for managing diabetes include:
- Limiting Carbohydrates: Starchy foods and sugary drinks can cause blood sugar spikes. Focus on consuming whole grains, fruits, vegetables, and lean proteins.
- Monitoring Portion Sizes: Pay attention to portion sizes to avoid overeating and manage blood sugar levels.
- Eating at Regular Intervals: Consistency in meal timing can help regulate blood sugar levels and prevent fluctuations throughout the day.
Working with a registered dietitian can help you develop a personalized meal plan that meets your dietary needs and fits your lifestyle.
Physical Activity and Exercise
Regular physical activity is an essential component of diabetes management. Exercise helps your body use insulin more effectively, lower blood sugar levels, and improve overall cardiovascular health. Some benefits of exercise for people with diabetes include:
- Lowering Blood Sugar Levels: Physical activity can help lower blood sugar levels by increasing insulin sensitivity.
- Weight Management: Exercise can help you maintain a healthy weight or lose excess weight, which is crucial for managing type 2 diabetes.
- Improving Cardiovascular Health: Regular exercise can lower blood pressure, improve cholesterol levels, and reduce the risk of heart disease.
Consult with your healthcare provider before starting an exercise regimen to ensure it is safe and appropriate for your individual health needs.
Tips for Living Well with Diabetes
Living with diabetes requires ongoing diligence and commitment to managing your health. Here are some tips to help you navigate the challenges of living with diabetes:
Stay Informed
Knowledge is power when it comes to managing diabetes. Stay informed about the latest research, treatment options, and lifestyle strategies for diabetes management. Education can empower you to take control of your health and make informed decisions about your care.
Build a Support Network
Living with diabetes can be challenging, but you don’t have to do it alone. Building a strong support network of family, friends, healthcare providers, and support groups can provide you with the encouragement and resources you need to navigate the ups and downs of managing diabetes.
Prioritize Self-Care
Taking care of yourself is essential when living with diabetes. Make time for activities that bring you joy and relaxation, such as reading, walking, or spending time with loved ones. Prioritizing self-care can help you manage stress, improve your overall well-being, and better cope with the demands of living with a chronic condition.
Set Realistic Goals
Setting realistic goals for your diabetes management can help you stay motivated and focused on your health. Break larger goals into smaller, manageable steps, and celebrate your accomplishments along the way. By setting achievable objectives, you can make steady progress towards better health and well-being.
Stay Positive
Maintaining a positive attitude can make a significant difference in how you manage diabetes. Focus on your strengths, resilience, and ability to overcome challenges. Remember that living with diabetes is a journey, and it’s okay to seek help and support when you need it.
Monitoring and Managing Blood Sugar Levels
Blood Sugar Targets
It is essential to set and monitor blood sugar targets to ensure that your diabetes is well-managed. Your healthcare provider can help you determine the ideal blood sugar targets based on factors such as age, overall health, and the presence of any diabetes-related complications.
| Blood Sugar Target | Ideal Range |
|---|---|
| Fasting Blood Sugar | 70-130 mg/dL (3.9-7.2 mmol/L) |
| Postprandial (After Meal) | Less than 180 mg/dL (10 mmol/L) |
Discuss your blood sugar targets with your healthcare provider and make a plan to track and adjust your blood sugar levels accordingly.
Understanding A1C Levels
A1C is a blood test that measures your average blood sugar levels over the past two to three months. This test provides a comprehensive view of how well your diabetes is controlled and can help guide treatment decisions. The American Diabetes Association recommends an A1C goal of less than 7% for most adults with diabetes.
Lifestyle Factors That Affect Blood Sugar Levels
Several lifestyle factors can impact blood sugar levels, including:
- Stress: Stress can cause blood sugar levels to rise. Learning to manage stress through relaxation techniques, mindfulness, and stress-reducing activities can help keep your blood sugar in check.
- Sleep: Lack of sleep can affect blood sugar levels and insulin sensitivity. Aim for quality sleep each night to support overall health and diabetes management.
- Alcohol: Alcohol can interfere with blood sugar control. Limit alcohol intake and monitor your blood sugar levels if you choose to consume alcoholic beverages.
By recognizing how lifestyle factors can influence your blood sugar levels, you can make informed choices to support optimal diabetes management.
Complications and Risk Factors
Diabetes Complications
Untreated or poorly managed diabetes can lead to a range of complications, including:
- Cardiovascular Disease: Diabetes increases the risk of heart disease, stroke, and other cardiovascular conditions.
- Nerve Damage (Neuropathy): High blood sugar levels can damage nerves throughout the body, leading to pain, numbness, and other symptoms.
- Kidney Disease (Nephropathy): Diabetes is a leading cause of kidney failure, which can require dialysis or a kidney transplant.
- Eye Damage (Retinopathy): Diabetes can cause damage to the blood vessels in the retina, leading to vision problems and potential blindness.
Regular monitoring of blood sugar levels, blood pressure, cholesterol levels, and kidney function can help reduce the risk of complications associated with diabetes.
Risk Factors for Type 2 Diabetes
Several factors can increase the risk of developing type 2 diabetes, including:
- Family History: If you have a family member with diabetes, you may be at a higher risk for developing the condition.
- Obesity: Being overweight or obese increases the risk of developing insulin resistance and type 2 diabetes.
- Physical Inactivity: Lack of exercise can contribute to weight gain and insulin resistance, increasing the risk of type 2 diabetes.
- Unhealthy Diet: Consuming a diet high in refined sugars, processed foods, and unhealthy fats can contribute to the development of type 2 diabetes.
Modifying lifestyle factors such as diet, exercise, and weight management can help reduce the risk of developing type 2 diabetes and support overall health and well-being.
Diabetes Management Tools and Resources
Healthcare Providers
Working with a multidisciplinary team of healthcare providers is essential for effective diabetes management. Your diabetes care team may include:
- Endocrinologist: A doctor who specializes in hormone-related disorders, including diabetes.
- Registered Dietitian: A nutrition expert who can help you develop a personalized meal plan.
- Certified Diabetes Educator (CDE): A healthcare professional who specializes in diabetes education and management.
- Pharmacist: A medication expert who can provide information about the use and side effects of diabetes medications.
Collaborating with a team of healthcare professionals can provide you with the support and resources you need to successfully manage your diabetes.
Diabetes Education Programs
Diabetes education programs offer valuable resources and information for individuals living with diabetes. These programs cover a range of topics, including blood sugar monitoring, healthy eating, medication management, and coping strategies for living with diabetes. Participating in a diabetes education program can help you gain the knowledge and skills needed to effectively manage your condition.
Mobile Apps and Technology
There are various mobile apps and digital tools available to help you monitor and manage your diabetes. These apps can track blood sugar levels, provide nutritional information, offer medication reminders, and connect you with healthcare providers. Using technology to track your diabetes management can simplify the process and improve your overall health outcomes.
Support Groups and Online Communities
Joining a support group or online community for individuals with diabetes can provide you with a platform to share experiences, ask questions, and connect with others who understand the challenges of living with diabetes. These groups offer emotional support, practical advice, and a sense of community that can help you navigate the complexities of managing diabetes.
Conclusion
Managing diabetes is a lifelong journey that requires dedication, education, and support. By taking a proactive approach to diabetes management and prioritizing your health and well-being, you can reduce the risk of complications and lead a fulfilling life with diabetes. Remember that you are not alone in this journey, and there are resources and tools available to help you navigate the challenges of living with diabetes. Take control of your health today and empower yourself to live well with diabetes.
