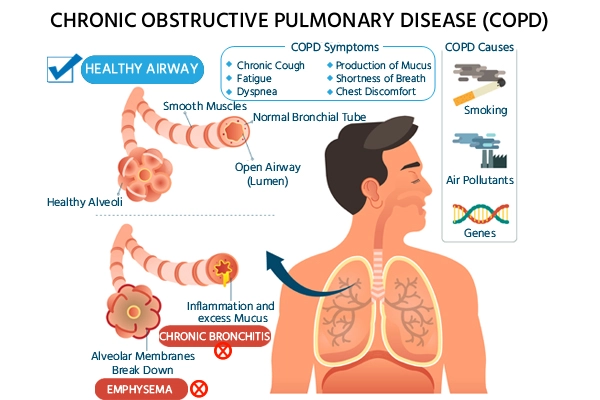
Living with chronic obstructive pulmonary disease (COPD) can be challenging, but thankfully, there are numerous treatment options available to help manage the condition. This article explores the most popular treatments for COPD, ranging from medications to pulmonary rehabilitation programs. Whether you’re newly diagnosed or seeking additional information, understanding these treatment options can empower you to take control of your health and improve your quality of life. Chronic obstructive pulmonary disease (COPD) is a chronic respiratory condition that affects millions of people around the world. Managing COPD requires a comprehensive treatment plan that may include a combination of medications, therapies, lifestyle changes, and more. In this article, we will explore the most popular treatments for COPD and provide insights into each treatment option. Whether you have been recently diagnosed with COPD or are already undergoing treatment, this guide will help you understand the various treatment options available to you.
Medication
Bronchodilators
Bronchodilators are medications that help relax and widen the airways, making it easier to breathe. These medications are commonly prescribed to individuals with COPD to alleviate symptoms such as breathlessness and wheezing. There are two main types of bronchodilators: short-acting and long-acting bronchodilators.
Short-acting bronchodilators are typically used on an as-needed basis to provide immediate relief during sudden flare-ups or exacerbations of COPD symptoms. These medications work quickly to open up the airways and provide temporary relief.
On the other hand, long-acting bronchodilators are taken regularly to prevent symptoms and maintain improved lung function over time. They are usually prescribed as a long-term treatment strategy to keep the airways open and reduce the frequency and severity of COPD symptoms.
Corticosteroids
Corticosteroids, also known as steroids, are anti-inflammatory medications commonly used in the treatment of COPD. These medications help reduce inflammation in the airways, easing breathing difficulties and decreasing the risk of exacerbations. Corticosteroids can be taken orally, inhaled, or administered through injections, depending on the severity of the symptoms.
Inhaled corticosteroids are often used in combination with bronchodilators to achieve better control of COPD symptoms. They are typically prescribed for individuals with moderate to severe COPD who have frequent exacerbations. The use of oral corticosteroids is generally reserved for more severe cases or during exacerbations that do not respond well to other treatment options.
Phosphodiesterase-4 Inhibitors
Phosphodiesterase-4 (PDE4) inhibitors are a newer class of medications used in the treatment of COPD. These medications work by reducing inflammation and relaxing the airway muscles, helping to improve lung function and reduce symptoms. PDE4 inhibitors are typically taken orally and can be beneficial for individuals with severe COPD and a history of exacerbations.
It is essential to discuss with your healthcare provider about the different medication options, their potential side effects, and how they may best fit into your personalized treatment plan. Your healthcare provider will consider factors such as the severity of your COPD, your overall health, and any other medications you may be taking to determine the most suitable medication for you.
Oxygen Therapy
Short-Burst Oxygen
Short-burst oxygen therapy involves the use of oxygen during specific activities or periods of exertion. It can provide a quick oxygen boost to help relieve breathlessness and improve physical activity tolerance. Short-burst oxygen is often recommended for individuals with COPD who experience desaturation or a drop in oxygen levels during certain tasks, such as walking or climbing stairs.
Your healthcare provider will assess your oxygen needs and guide you on when and how to use short-burst oxygen therapy effectively. They may recommend using a portable oxygen cylinder or concentrator that allows you to access oxygen on-the-go as needed.
Ambulatory Oxygen
Ambulatory oxygen therapy involves the use of oxygen during daily activities and exercise. It aims to improve oxygen saturation levels and enhance overall quality of life for individuals with COPD. Ambulatory oxygen can help reduce breathlessness, increase exercise capacity, and enhance energy levels, allowing individuals to stay more active and engaged in daily activities.
To receive ambulatory oxygen, your healthcare provider will assess your oxygen needs and determine the appropriate flow rate and duration of oxygen therapy based on your exercise capacity and oxygen saturation levels. Portable oxygen concentrators or lightweight oxygen cylinders are commonly used to deliver oxygen during ambulatory activities.
Nocturnal Oxygen
Nocturnal oxygen therapy is prescribed to individuals with COPD who experience low oxygen levels during sleep. It involves the use of oxygen during nighttime sleep to help maintain adequate oxygen saturation levels and prevent complications associated with low blood oxygen levels.
Your healthcare provider may recommend a nocturnal oxygen assessment, such as an overnight oximetry test or a polysomnogram, to evaluate your oxygen needs during sleep. Based on the test results, they will determine the appropriate oxygen flow rate and duration for nocturnal oxygen therapy. Oxygen concentrators or liquid oxygen systems are commonly used to deliver oxygen during sleep.
Pulmonary Rehabilitation
Pulmonary rehabilitation is a comprehensive program that combines various therapies, education, and support to help individuals with COPD improve their overall well-being, alleviate symptoms, and enhance their ability to perform daily activities. The components of pulmonary rehabilitation typically include exercise training, nutritional counseling, and breathing techniques.
Exercise Training
Exercise training is a fundamental component of pulmonary rehabilitation for individuals with COPD. It involves a combination of aerobic activities, such as walking or cycling, and muscle-strengthening exercises to improve cardiovascular fitness, muscle strength, and endurance. Regular exercise can help individuals with COPD develop better breathing patterns, reduce breathlessness, and enhance their overall physical performance.
A pulmonary rehabilitation program typically includes supervised exercise sessions conducted in a specialized facility or hospital. Exercise training is tailored to each individual’s needs and abilities, and progress is monitored closely by healthcare professionals to ensure safe and effective outcomes.
Nutritional Counseling
Nutritional counseling plays an essential role in the management of COPD. Individuals with COPD may experience involuntary weight loss, muscle wasting, and nutritional deficiencies due to increased energy demands and decreased appetite associated with the condition. Proper nutrition can help maintain overall health, support respiratory muscle function, and improve immune system function.
During pulmonary rehabilitation, a healthcare professional, such as a dietitian or nutritionist, will assess your nutritional status, dietary intake, and specific needs. They will provide guidance on balanced meals, portion sizes, and strategies to maintain a healthy weight. They may also recommend specific dietary modifications, such as increasing calorie and protein intake, to support optimal respiratory function.
Breathing Techniques
Breathing techniques are an integral part of pulmonary rehabilitation for individuals with COPD. These techniques aim to improve breathing efficiency, reduce breathlessness, and enhance overall respiratory function. Various breathing exercises, such as diaphragmatic breathing, pursed-lip breathing, and controlled breathing, may be taught during pulmonary rehabilitation.
Pursed-lip breathing is a breathing technique commonly used by individuals with COPD to control breathlessness and promote better airway control. It involves inhaling slowly through the nose and exhaling gently through the mouth with pursed lips. This technique helps create back pressure in the airways, preventing early airway collapse and improving oxygen exchange.
By incorporating pulmonary rehabilitation into your COPD management plan, you can experience significant improvements in your overall physical fitness, respiratory function, and quality of life. It is crucial to work closely with your healthcare team to develop an individualized pulmonary rehabilitation program that meets your specific needs and goals.
Lung Volume Reduction Surgery
Lung volume reduction surgery (LVRS) is a surgical procedure performed on individuals with severe emphysema, a type of COPD. The goal of LVRS is to remove damaged or diseased parts of the lungs to improve lung function, relieve symptoms, and enhance overall quality of life.
Bullectomy
Bullectomy is a specific type of lung volume reduction surgery that involves the removal of large air spaces called bullae. Bullae are abnormal air pockets that develop in areas of damaged lung tissue and can compress adjacent healthy lung tissue, impairing lung function. By removing these bullae, the remaining healthy lung tissue can function more effectively, leading to improved breathing capacity.
Bullectomy is typically considered for individuals with severe emphysema who have large bullae occupying a significant portion of their lungs. The procedure can be performed either through open surgery or minimally invasive techniques, depending on individual circumstances and surgeon expertise.
Lung Transplantation
Lung transplantation is a treatment option for individuals with end-stage COPD, who have severe respiratory impairment and have not responded well to other treatment modalities. During a lung transplantation, a diseased lung is replaced with a healthy lung from a donor, allowing the individual to breathe better and improve their overall quality of life.
Lung transplantation is a complex surgical procedure that requires a careful evaluation process, including medical, psychological, and social assessments. Moreover, availability of suitable donor organs and post-transplant care are crucial factors in determining the success of lung transplantation. It is considered a last-resort option for individuals with severe COPD who meet specific criteria and have exhausted other treatment possibilities.

Supplemental Nutrition
Vitamin D
Vitamin D plays a crucial role in overall health, including lung health. Some studies suggest that individuals with COPD may have lower levels of vitamin D compared to healthy individuals, and maintaining adequate vitamin D levels may help reduce the risk of complications and improve respiratory function.
Your healthcare provider may recommend monitoring your vitamin D levels through blood tests and prescribing vitamin D supplements if deficiencies are detected. Additionally, incorporating vitamin D-rich foods, such as fatty fish, fortified dairy products, and egg yolks, into your diet can help support optimal respiratory health.
Omega-3 Fatty Acids
Omega-3 fatty acids are a type of healthy fat found in certain foods, such as fatty fish, nuts, and flaxseed. These fatty acids have anti-inflammatory properties and may help reduce inflammation in the airways, improving lung function and decreasing symptoms in individuals with COPD.
Incorporating omega-3 fatty acids into your diet can be beneficial for overall health and respiratory function. Consult with your healthcare provider or a registered dietitian to determine the appropriate amount of omega-3 fatty acids for your specific needs and to discuss dietary modifications or the use of omega-3 supplements if necessary.
Smoking Cessation
Behavioral Support
Smoking cessation is the most important step individuals with COPD can take to slow the progression of the disease and improve their overall health. Quitting smoking can significantly reduce symptoms, enhance lung function, and decrease the frequency of exacerbations.
Behavioral support, such as counseling, therapy, or support groups, plays a pivotal role in smoking cessation. These interventions are designed to help individuals overcome nicotine addiction, develop healthy coping strategies, and adopt positive lifestyle changes. Behavioral support can be provided by healthcare professionals, addiction specialists, or smoking cessation programs.
Nicotine Replacement Therapy
Nicotine replacement therapy (NRT) is a widely used approach to help individuals quit smoking. NRT involves delivering nicotine to the body through alternative sources, such as nicotine patches, gum, lozenges, nasal sprays, or inhalers. By providing a controlled dose of nicotine, NRT helps alleviate nicotine withdrawal symptoms and cravings, facilitating the smoking cessation process.
Nicotine replacement therapy is available over-the-counter or through prescription, depending on the specific nicotine replacement product. It is essential to consult with your healthcare provider to discuss the most suitable NRT option based on your smoking habits, medical history, and individual needs.
Medications
In addition to behavioral support and nicotine replacement therapy, certain medications can be prescribed to aid smoking cessation in individuals with COPD. Medications, such as bupropion and varenicline, work to reduce nicotine cravings and withdrawal symptoms, making it easier to quit smoking.
These medications should be used under the guidance of a healthcare professional who can assess your individual circumstances and determine the most appropriate medication and dosage for you. It is important to discuss any potential side effects or contraindications with your healthcare provider before starting any smoking cessation medications.
Vaccinations
Influenza Vaccine
Annual influenza vaccination is crucial for individuals with COPD to prevent complications associated with influenza infection. Influenza, also known as the flu, can cause severe respiratory illness and exacerbate COPD symptoms, leading to hospitalization or other serious health consequences.
Receiving the influenza vaccine each year can help protect against the flu and reduce the risk of complications. The vaccine is typically administered as an injection and is recommended for all individuals with COPD, regardless of age or severity of the condition. It is generally recommended to get the vaccination before the start of the flu season, which varies by region.
Pneumococcal Vaccine
Pneumococcal vaccination is recommended for individuals with COPD to protect against pneumococcal infections, including pneumonia. People with COPD are at a higher risk of developing pneumonia, which can lead to severe respiratory complications and exacerbations of COPD symptoms.
The pneumococcal vaccine helps reduce the risk of pneumococcal infections and their associated complications. There are currently two types of pneumococcal vaccines available: pneumococcal conjugate vaccine (PCV13) and pneumococcal polysaccharide vaccine (PPSV23). Your healthcare provider will determine which vaccine is appropriate for you based on your age, vaccination history, and specific risk factors.
Pursed-lip Breathing
Techniques and Benefits
Pursed-lip breathing is a breathing technique commonly used by individuals with COPD to manage breathlessness and promote better control of airflow. It involves inhaling slowly through the nose and exhaling gently through pursed lips, as if blowing out a candle. This technique helps create resistance in the airways, prolonging exhalation and enhancing oxygen exchange.
Pursed-lip breathing can help relieve shortness of breath, reduce the effort required to breathe, and improve lung function. By promoting the release of trapped air and preventing early airway collapse, this technique can enhance overall respiratory comfort and allow individuals with COPD to engage in daily activities with greater ease.
Practicing pursed-lip breathing regularly can help individuals with COPD develop better breathing habits and reduce the frequency of breathlessness episodes. It is best to learn this technique under the guidance of a respiratory therapist or healthcare provider, who can provide proper instruction and ensure correct technique implementation.

Lifestyle Changes
Exercise and Physical Activity
Incorporating regular exercise and physical activity into your daily routine is essential for managing COPD. Exercise can improve cardiovascular fitness, increase muscle strength and endurance, and enhance overall respiratory function. Engaging in activities such as walking, cycling, swimming, or yoga can help improve lung capacity and reduce breathlessness.
It is important to start with low-impact exercises and gradually increase the intensity as tolerated. Working with a pulmonary rehabilitation program, a physical therapist, or an exercise specialist can help design an exercise plan that is specific to your needs and abilities. Always consult with your healthcare provider before starting any new exercise regimen to ensure it is safe and appropriate for you.
Dietary Changes
Maintaining a healthy diet is essential for individuals with COPD to support overall health, maintain proper weight, and optimize respiratory function. Eating a well-balanced diet that includes fruits, vegetables, whole grains, lean proteins, and healthy fats can provide essential nutrients and support optimal lung health.
Your healthcare provider, along with a registered dietitian, can help assess your dietary needs, identify any deficiencies, and create an appropriate meal plan. They may recommend consuming smaller, more frequent meals to reduce breathlessness during eating, as well as suggestions to avoid foods that may trigger symptoms or excess bloating.
Avoiding Respiratory Irritants
Avoiding respiratory irritants and environmental triggers is crucial for managing COPD and preventing exacerbations. Exposure to substances such as tobacco smoke, air pollution, dust, chemicals, and strong odors can worsen COPD symptoms and contribute to respiratory flare-ups.
If you smoke, quitting is essential to protect your lungs and slow the progression of COPD. It is also important to avoid secondhand smoke and maintain a smoke-free environment.
Reducing exposure to air pollution and environmental toxins can be achieved by staying indoors during high pollution days, using air purifiers in your home, and taking precautions when in heavily polluted areas.
When working or spending time in dusty or chemical-filled environments, wearing a mask or respirator can help filter the air and protect your lungs. Additionally, avoiding strong odors or fumes can help minimize respiratory irritation.
Acupuncture
Effectiveness and Considerations
Acupuncture is a complementary therapy that involves the insertion of thin needles into specific points on the body to promote healing and symptom relief. Some individuals with COPD may consider acupuncture as an adjunct to traditional medical treatments to alleviate symptoms and enhance overall well-being.
Research on the effectiveness of acupuncture in treating COPD is limited and often mixed. While some studies suggest that acupuncture may help improve lung function, reduce dyspnea (shortness of breath), and enhance quality of life in individuals with COPD, others have found little to no significant benefit.
If you are considering acupuncture for COPD, it is crucial to consult with your healthcare provider and a licensed acupuncturist. They can guide you on the potential benefits, risks, and appropriate integration of acupuncture into your comprehensive treatment plan.
In conclusion, managing COPD requires a multifaceted approach that addresses various aspects of the condition. Treatment options range from medication to improve lung function and reduce inflammation, oxygen therapy to support oxygen levels, pulmonary rehabilitation to enhance physical fitness and respiratory function, and lifestyle changes to promote overall health and well-being. By working closely with your healthcare team and following a personalized treatment plan, you can effectively manage COPD and improve your quality of life. Remember, everyone’s journey with COPD is unique, and it may take time to find the optimal combination of treatments that work best for you.