In today’s fast-paced and ever-evolving healthcare landscape, the issue of rising healthcare costs has become a pressing concern for individuals and governments alike. With the increasing demand for quality healthcare services, it is imperative to explore the role of healthcare policy in addressing healthcare cost containment. By implementing effective policies that focus on cost-effective strategies, innovative payment models, and enhanced healthcare delivery systems, we can strive towards a more sustainable healthcare system that provides accessible and affordable care for all.

Introduction
In today’s healthcare landscape, cost containment has become a critical issue that policymakers and stakeholders are grappling with. The rising cost of healthcare has put a strain on individuals, families, and the economy as a whole. Healthcare policy plays a crucial role in addressing these escalating costs and finding sustainable solutions. By defining cost containment, understanding its importance, and exploring the role of healthcare policy, we can gain insights into the factors influencing healthcare costs, different approaches to cost containment, successful examples, challenges, and recommendations for the future.
1. Definition of Healthcare Cost Containment
Healthcare cost containment refers to the efforts made to control and reduce the rapidly increasing costs associated with providing medical services and care to individuals and communities. It involves implementing measures to slow down the rate of growth in healthcare spending while maintaining or improving the quality of care. Cost containment strategies aim to achieve a balance between affordability, access to care, and high-quality outcomes.
2. Importance of Healthcare Cost Containment
The importance of healthcare cost containment cannot be overstated. As healthcare costs continue to rise, they put a significant burden on individuals, families, employers, and governments. High healthcare costs can lead to financial hardship for individuals, increased premiums for employers, and strain on government budgets. In addition, escalating healthcare costs can limit access to care, leading to disparities in health outcomes and an inefficient healthcare system. Effective cost containment measures are crucial to ensuring a sustainable healthcare system that provides affordable, accessible, and high-quality care for all.
3. Role of Healthcare Policy
Healthcare policy plays a pivotal role in addressing healthcare cost containment. It provides a framework for setting goals, implementing strategies, and regulating the healthcare market. By implementing evidence-based policies, healthcare systems can achieve cost containment while improving health outcomes. The role of healthcare policy includes:
3.1 Setting Cost Control Goals
Healthcare policy sets the objectives for cost containment by defining specific goals and targets. These goals may focus on reducing healthcare spending growth, improving cost-efficiency, or enhancing the value of healthcare services. By setting clear goals, policymakers can guide the development and implementation of effective cost containment strategies.
3.2 Implementing Cost Reduction Strategies
Healthcare policy facilitates the implementation of various cost reduction strategies. These strategies can include promoting preventive care, reducing administrative costs, implementing payment reforms, and encouraging the use of technology to improve efficiency. By strategically implementing these strategies, healthcare systems can achieve cost containment without compromising the quality of care.
3.3 Regulating Pricing and Reimbursement
Healthcare policy plays a crucial role in regulating pricing and reimbursement. By establishing pricing rules, policies can ensure fair and transparent pricing for healthcare services. Additionally, policies can regulate reimbursement rates to align them with the goals of cost containment and quality improvement. These regulations create a level playing field and prevent excessive costs from being passed on to patients and payers.
3.4 Encouraging Preventive Care
Healthcare policy can incentivize and promote preventive care as a cost containment measure. By focusing on preventive strategies, such as vaccinations, screenings, and health education, policymakers can reduce the prevalence and severity of chronic diseases. Preventive care not only improves health outcomes but also reduces the need for costly interventions and hospitalizations, resulting in long-term cost savings.
3.5 Promoting Competition in the Healthcare Market
Healthcare policy can foster competition in the healthcare market as a means of achieving cost containment. By encouraging competition among healthcare providers, insurers, and pharmaceutical companies, policymakers can drive down prices while maintaining quality. Increased competition leads to greater efficiency, innovation, and cost reduction, ultimately benefiting consumers and the healthcare system as a whole.
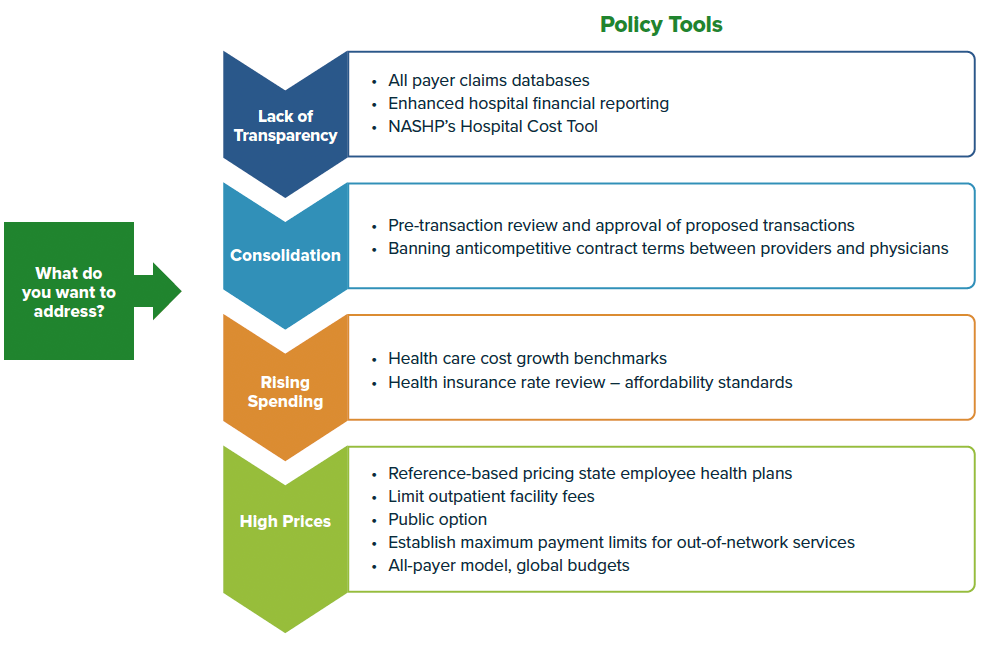
4. Factors Influencing Healthcare Costs
To effectively address healthcare cost containment, it is essential to understand the factors that contribute to rising healthcare costs. Several key factors influence healthcare costs:
4.1 Technology and Innovation
Technological advancements and medical innovations have significantly contributed to rising healthcare costs. While medical breakthroughs have led to improved outcomes and treatments, they often come at a high price. The costs associated with research, development, and implementation of new technologies impact overall healthcare spending and must be carefully managed.
4.2 Aging Population
An aging population is another significant factor driving healthcare costs. As the population ages, there is an increased demand for healthcare services, especially for chronic diseases and long-term care. The costs of providing care for older adults, including hospitalizations, medications, and specialized services, place a significant financial burden on the healthcare system.
4.3 Chronic Diseases
The prevalence of chronic diseases, such as diabetes, heart disease, and obesity, has been on the rise in recent years. Chronic diseases require long-term management and often lead to costly complications. The management and treatment of chronic diseases contribute significantly to healthcare expenditures and require effective cost containment strategies.
4.4 Administrative Costs
Administrative costs, including billing, coding, and insurance-related activities, account for a significant proportion of healthcare spending. Streamlining administrative processes and reducing unnecessary bureaucracy can help contain healthcare costs.
4.5 Pharmaceuticals
The high cost of pharmaceuticals is a notorious factor driving healthcare costs. The development of new drugs, price inflation, and the high cost of specialty medications contribute to increased spending on pharmaceuticals. Negotiating drug prices and promoting the use of generic medications are potential cost containment strategies.
4.6 Provider Reimbursement
Provider reimbursement rates also impact healthcare costs. The fee-for-service model, which reimburses healthcare providers for each service rendered, can incentivize unnecessary procedures and tests, driving up costs. Shifting towards value-based reimbursement models that focus on quality outcomes and cost-efficiency can help contain costs while promoting high-quality care.
5. Healthcare Policy Approaches to Cost Containment
Healthcare policies employ various approaches to achieve cost containment. These approaches aim to improve healthcare quality, increase efficiency, and reduce unnecessary spending. Key healthcare policy approaches to cost containment include:
5.1 Payment Reforms
Payment reforms focus on changing the way healthcare providers are reimbursed for their services. This includes transitioning from fee-for-service to alternative payment models that promote value-based care. Bundled payments, accountable care organizations, and pay-for-performance models are examples of payment reforms aimed at aligning reimbursement with quality outcomes and cost-efficiency.
5.2 Value-Based Care Models
Value-based care models prioritize the delivery of high-quality care at an affordable cost. These models focus on outcomes, patient experience, and cost-effectiveness. By incentivizing providers to meet specific quality and cost targets, value-based care models encourage improved care coordination and efficiency.
5.3 Health Information Technology
Health information technology plays a crucial role in cost containment efforts. Electronic health records, telemedicine, and other digital tools can streamline workflows, improve communication among healthcare providers, and reduce administrative costs. Additionally, health information technology enables better data analysis and population health management, facilitating evidence-based decision-making and cost-effective care delivery.
5.4 Care Coordination and Integration
Efforts to improve care coordination and integration can help reduce healthcare costs and improve patient outcomes. By ensuring that all healthcare providers involved in a patient’s care work together and share information, unnecessary duplications and inefficiencies can be minimized. Coordinated and integrated care models, such as patient-centered medical homes and care teams, promote continuity of care, reduce hospital readmissions, and ultimately lower costs.
5.5 Evidence-Based Medicine
Evidence-based medicine involves the use of scientific evidence to guide clinical decision-making and improve patient outcomes. By promoting the use of evidence-based guidelines and treatment protocols, healthcare systems can achieve higher quality care and reduce unnecessary spending on ineffective or low-value interventions.
5.6 Telemedicine and Remote Monitoring
Telemedicine and remote monitoring technologies enable the provision of healthcare services and monitoring of patients’ health remotely. These technologies can reduce the need for in-person visits, which can be costly and time-consuming. Telemedicine and remote monitoring can improve access to care, particularly for underserved populations, while reducing healthcare costs.

6. Successful Examples of Healthcare Cost Containment Policies
Several countries and healthcare systems have implemented successful cost containment policies. These examples offer valuable insights into effective strategies for achieving cost containment while maintaining quality care. Some notable examples include:
6.1 International Comparison: The Case of Germany
Germany’s healthcare system has achieved successful cost containment by employing a combination of strategies. These include strict regulation of healthcare prices, mandatory health insurance coverage, payment reforms, and emphasis on preventive care and primary care. Germany’s approach highlights the importance of a comprehensive and coordinated healthcare system in achieving cost containment.
6.2 Affordable Care Act in the United States
The Affordable Care Act (ACA) in the United States aimed to increase access to healthcare while also containing costs. Through various provisions, such as the establishment of health insurance marketplaces, expansion of Medicaid, and implementation of payment reforms, the ACA has had a positive impact on reducing the uninsured rate and slowing down healthcare spending growth.
6.3 Accountable Care Organizations
Accountable Care Organizations (ACOs) are groups of healthcare providers that collaborate to deliver coordinated and high-quality care to a defined population. ACOs have shown promising results in terms of cost savings and improved care outcomes. By promoting care coordination, prevention, and value-based reimbursement, ACOs have the potential to achieve sustainable cost containment.
6.4 Bundled Payments
Bundled payment models involve the reimbursement of healthcare providers for a defined episode of care, rather than individual services. This approach encourages greater collaboration among providers, reduces unnecessary procedures, and promotes efficiency. Bundled payments have been successful in reducing costs and improving care coordination in various settings, including joint replacements and maternity care.
6.5 Medicaid Expansion
Medicaid expansion, as implemented under the ACA, has provided coverage for millions of low-income individuals and families. By expanding Medicaid eligibility, states have improved access to care and reduced the financial burden on individuals, leading to better health outcomes and cost containment.
7. Challenges and Limitations of Healthcare Cost Containment Policies
While healthcare cost containment policies offer significant benefits, they also face several challenges and limitations. These challenges must be considered to ensure the effectiveness and sustainability of cost containment efforts. Some key challenges include:
7.1 Political and Stakeholder Resistance
Implementing cost containment policies often encounters resistance from political stakeholders, interest groups, and healthcare providers. Resistance can arise due to concerns about reduced revenue, changes in reimbursement models, or perceived threats to autonomy and quality of care. Overcoming resistance requires effective communication, stakeholder engagement, and collaboration among all entities involved.
7.2 Access to Care and Quality Concerns
Cost containment efforts must carefully balance the need to reduce healthcare costs with the provision of timely and high-quality care. There is a risk that stringent cost containment measures may limit access to care or compromise the quality of services. Policymakers must carefully evaluate the potential impacts of cost containment measures to ensure that they do not inadvertently harm patients or lead to disparities in care.
7.3 Rising Healthcare Costs in Other Areas
While cost containment policies may succeed in one area, they can inadvertently contribute to rising healthcare costs in other areas. For example, reducing reimbursement rates for certain services may result in providers compensating by increasing prices in other areas. Policymakers must take a holistic approach to cost containment to minimize unintended consequences.
7.4 Balancing Cost Containment with Innovation
Achieving cost containment while promoting innovation in healthcare is a delicate balance. Strict cost containment measures may discourage investment in research and development, leading to a slowdown in medical innovation. Finding the right balance between cost containment and fostering innovation is essential to ensure long-term sustainability and progress in healthcare.
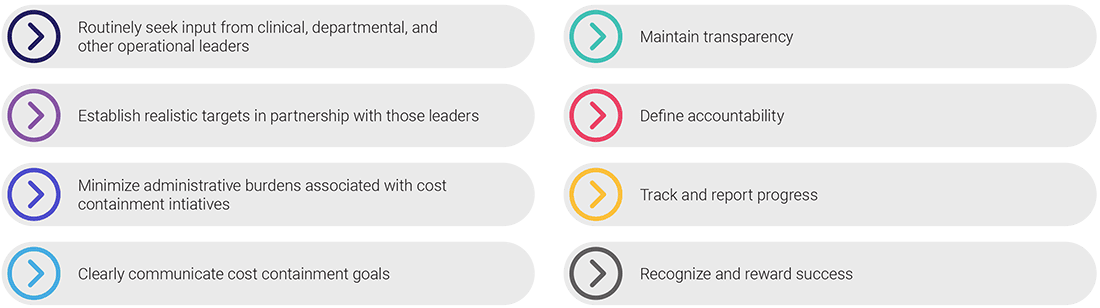
8. Future Directions and Recommendations
To address the ongoing challenge of healthcare cost containment effectively, it is crucial to consider future directions and recommendations. By focusing on these areas, policymakers can navigate the evolving healthcare landscape and promote sustainable cost containment. Some future directions and recommendations include:
8.1 Investing in Health IT Infrastructure
Health information technology infrastructure must be improved to support cost containment efforts. This includes promoting interoperability among electronic health records, increasing access to telemedicine, and investing in data analytics for population health management. By leveraging technology effectively, healthcare systems can achieve improved efficiency, reduced administrative burdens, and better coordination of care.
8.2 Strengthening Primary Care and Preventive Services
Investing in primary care and preventive services is crucial for achieving cost containment. A robust primary care system can help prevent unnecessary hospitalizations and emergency room visits, reducing overall healthcare costs. Prioritizing preventive care, health education, and early intervention can lead to better health outcomes and lower long-term healthcare expenditures.
8.3 Promoting Value-Based Reimbursement Across Payers
Expanding value-based reimbursement models to all payers, including private insurers and Medicare, can help drive cost containment efforts. By aligning financial incentives with quality outcomes and cost-efficiency, providers are encouraged to deliver high-value care. Continued collaboration among payers, providers, and policymakers is necessary to accelerate the adoption of value-based reimbursement models.
8.4 Addressing Social Determinants of Health
Recognizing and addressing the social determinants of health is imperative for achieving effective cost containment. Factors such as income, education, housing, and access to healthy food significantly impact health outcomes and healthcare costs. By investing in social programs, improving socioeconomic conditions, and implementing policies that address health disparities, healthcare systems can achieve long-term cost savings.
8.5 Encouraging Transparent Pricing and Patient Empowerment
Promoting transparent pricing and empowering patients to make informed healthcare decisions is vital for cost containment. Transparent pricing allows patients to compare costs and make value-based choices. Providing patients with access to their health information, educational resources, and decision-making tools can help foster a culture of patient empowerment and engagement, leading to wiser healthcare utilization and more cost-conscious decisions.
Conclusion
Healthcare cost containment is a multifaceted challenge that requires continuous efforts and strategic policy implementation. By defining cost containment, recognizing its importance, understanding the role of healthcare policy, and exploring factors influencing healthcare costs, approaches to cost containment, successful examples, challenges, and future recommendations, we can pave the way for a sustainable and affordable healthcare system. Through evidence-based policies, collaboration among stakeholders, and a focus on value-based care, healthcare systems can achieve the delicate balance of containing costs while ensuring access to high-quality care for all.

