In this article, you will gain valuable insight into the world of autoimmune diseases. From the common types that often go unnoticed to the treatment options available, this information will empower you with the knowledge needed to better understand and manage these conditions. So, grab a cup of tea, sit back, and let’s embark on a journey to unravel the complexities of autoimmune diseases together.
What are autoimmune diseases?
Definition
Autoimmune diseases are conditions in which the immune system mistakenly attacks and damages healthy cells and tissues in the body. Normally, the immune system is responsible for defending the body against foreign invaders like bacteria and viruses. However, in people with autoimmune diseases, the immune system cannot distinguish between these foreign substances and the body’s own cells. As a result, the immune system launches an immune response, causing inflammation and damage to various organs and tissues.
Causes
The exact causes of autoimmune diseases are still largely unknown. However, researchers believe that a combination of genetic, environmental, and hormonal factors play a role in their development. Genetic predisposition is believed to make certain individuals more susceptible to autoimmune diseases, as certain genes may affect how the immune system functions. Environmental factors, such as infections, exposure to certain toxins, and diet, may also trigger or exacerbate autoimmune diseases. Hormonal changes, such as those that occur during pregnancy or menopause, can also influence the development of autoimmune diseases.
Prevalence
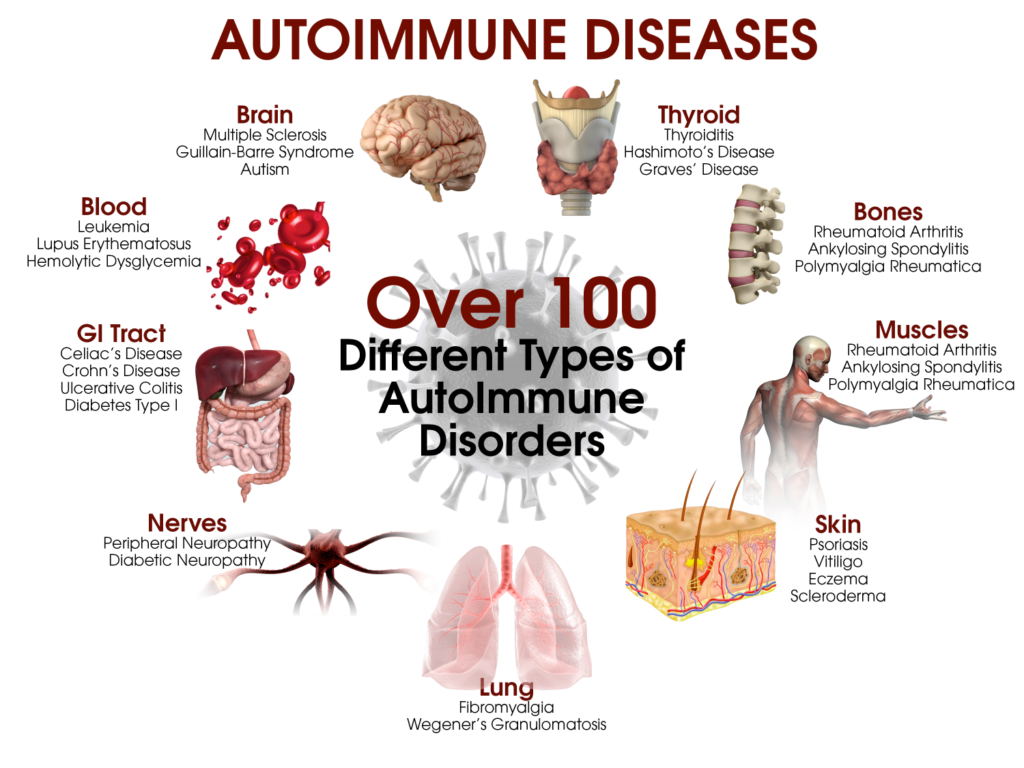
Autoimmune diseases are relatively common, affecting millions of people worldwide. According to the American Autoimmune Related Diseases Association (AARDA), there are over 100 known autoimmune diseases, and they collectively affect approximately 50 million Americans. Women are more likely to develop autoimmune diseases than men, and the onset of symptoms often occurs during childbearing years. Autoimmune diseases can affect individuals of any age, race, or ethnicity.
Common types of autoimmune diseases
Rheumatoid arthritis
Rheumatoid arthritis is a chronic inflammatory disease that primarily affects the joints. It is characterized by the immune system mistakenly attacking the synovium, which is the lining around the joints. This leads to joint inflammation, pain, and swelling. Over time, rheumatoid arthritis can cause joint deformities and damage to other organs, such as the heart and lungs.
Systemic lupus erythematosus
Systemic lupus erythematosus, commonly referred to as lupus, is an autoimmune disease that can affect multiple organs and tissues in the body. It is characterized by periods of flare-ups and remission. Lupus can cause a wide range of symptoms, including joint pain, skin rashes, fatigue, and kidney problems. It primarily affects women of childbearing age.
Multiple sclerosis
Multiple sclerosis (MS) is a chronic autoimmune disease that affects the central nervous system. It occurs when the immune system mistakenly attacks the protective covering of nerve fibers, disrupting the communication between the brain and the rest of the body. This can lead to a wide range of symptoms, including fatigue, coordination and balance problems, muscle weakness, and cognitive impairments.
Type 1 diabetes
Type 1 diabetes is an autoimmune disease in which the immune system destroys the insulin-producing cells in the pancreas. Without insulin, the body cannot regulate blood sugar levels, leading to high blood sugar levels. People with type 1 diabetes require lifelong insulin therapy.
Inflammatory bowel disease
Inflammatory bowel disease (IBD) is an umbrella term for chronic inflammatory conditions of the digestive tract, including Crohn’s disease and ulcerative colitis. In IBD, the immune system mistakenly attacks the lining of the intestines, leading to inflammation, abdominal pain, diarrhea, and other digestive symptoms.
Hashimoto’s thyroiditis
Hashimoto’s thyroiditis is an autoimmune disease in which the immune system attacks the thyroid gland, leading to inflammation and decreased thyroid function. This can result in symptoms such as fatigue, weight gain, and sensitivity to cold. Hashimoto’s thyroiditis is the most common cause of hypothyroidism, an underactive thyroid.
Psoriasis
Psoriasis is a chronic autoimmune skin condition characterized by the rapid buildup of skin cells, leading to thick, scaly patches on the skin. These patches can be itchy and painful. Psoriasis can also affect the nails and joints, causing psoriatic arthritis.
Graves’ disease
Graves’ disease is an autoimmune disease that affects the thyroid gland. In this condition, the immune system produces antibodies that stimulate the thyroid gland to produce excessive amounts of thyroid hormone. This leads to symptoms such as weight loss, rapid heartbeat, and anxiety.
Sjögren’s syndrome
Sjögren’s syndrome is an autoimmune disease that primarily affects the salivary and lacrimal glands, leading to decreased production of tears and saliva. This can result in symptoms such as dry eyes, dry mouth, and difficulty swallowing.
Autoimmune hepatitis
Autoimmune hepatitis is a chronic liver disease in which the immune system attacks the liver cells, leading to inflammation and liver damage. It can cause symptoms such as fatigue, jaundice, and abdominal pain.

Symptoms and diagnosis
General symptoms
While the specific symptoms of autoimmune diseases can vary depending on the type of disease and the organs affected, there are some general symptoms that may indicate an autoimmune condition. These may include fatigue, joint pain, muscle weakness, fever, and general malaise. It is important to note that these symptoms can also be caused by other conditions, so a thorough medical evaluation is necessary for an accurate diagnosis.
Specific symptoms
Each autoimmune disease has its own distinct set of symptoms. For example, rheumatoid arthritis primarily affects the joints and can cause joint pain, swelling, and deformities. Lupus, on the other hand, can cause a wide range of symptoms, including skin rashes, joint pain, and kidney problems. Multiple sclerosis often presents with symptoms such as fatigue, numbness or tingling, and problems with coordination.
Diagnosis process
Diagnosing autoimmune diseases can be challenging, as the symptoms can be vague and similar to those of other conditions. The diagnosis process usually starts with a thorough medical history and physical examination. Your healthcare provider may also order specific laboratory tests and imaging studies to help confirm a diagnosis.
Laboratory tests
Laboratory tests are often used to measure certain antibodies or other markers that may be present in autoimmune diseases. These tests can include blood tests to detect specific autoantibodies or markers of inflammation. Examples of commonly used tests include antinuclear antibody (ANA) test, rheumatoid factor (RF) test, and erythrocyte sedimentation rate (ESR) test.
Imaging studies
Imaging studies, such as X-rays, ultrasounds, or magnetic resonance imaging (MRI), may be performed to visualize the affected organs or tissues. These tests can help detect any abnormalities or changes that may be indicative of an autoimmune disease.
Biopsy
In some cases, a biopsy may be necessary to obtain a small tissue sample for further examination under a microscope. Biopsies can provide valuable information about the presence of inflammation, the extent of tissue damage, and the specific type of autoimmune disease.
Risk factors and triggers
Genetic predisposition
Genetics plays a role in the development of autoimmune diseases. Certain genes may make individuals more susceptible to developing autoimmune conditions. Having a family history of autoimmune diseases increases the risk of developing these conditions. However, having a genetic predisposition does not guarantee that an individual will develop an autoimmune disease, as other triggers are also involved.
Environmental factors
Environmental factors can trigger or exacerbate autoimmune diseases. These factors may include exposure to certain infections, toxins, or pollutants. For example, exposure to certain viruses or bacteria has been associated with the development of autoimmune diseases. Additionally, certain medications, such as antibiotics, may also trigger autoimmune responses in susceptible individuals.
Infections
Infections, particularly viral infections, have been linked to the development of autoimmune diseases. It is believed that certain infections can trigger an abnormal immune response, leading to the development of autoantibodies and the subsequent attack on healthy cells and tissues.
Hormonal changes
Hormonal changes, such as those that occur during puberty, pregnancy, or menopause, can influence the development and severity of autoimmune diseases. For example, many autoimmune diseases, including lupus and rheumatoid arthritis, are more common in women of childbearing age. This suggests that hormonal fluctuations may play a role in triggering or exacerbating autoimmune responses.
Stress
Chronic stress has been identified as a potential trigger for autoimmune diseases. Stress can affect the immune system, leading to dysregulation and abnormalities in immune function. This can increase the risk of developing autoimmune diseases or worsen existing symptoms.

Treatment options
Immunosuppressive medications
Immunosuppressive medications are commonly used to treat autoimmune diseases. These medications work by suppressing the immune system, reducing the immune response and inflammation. Examples of immunosuppressive medications include methotrexate, azathioprine, and mycophenolate mofetil. These medications can help control symptoms and prevent further damage to organs and tissues.
Corticosteroids
Corticosteroids, such as prednisone, are potent anti-inflammatory medications that are often used to reduce inflammation and suppress the immune system in autoimmune diseases. They can provide rapid relief of symptoms but are typically used for short periods of time due to their potential side effects.
Biologic therapies
Biologic therapies are a newer class of medications that specifically target certain components of the immune system, such as specific cytokines or immune cells. These medications are often used when other treatments have not been effective. Examples of biologic therapies include tumor necrosis factor (TNF) inhibitors, interleukin-6 (IL-6) inhibitors, and B-cell targeted therapies.
Nonsteroidal anti-inflammatory drugs (NSAIDs)
Nonsteroidal anti-inflammatory drugs (NSAIDs) are commonly used to relieve pain and reduce inflammation in autoimmune diseases. They work by blocking certain enzymes that play a role in inflammation. NSAIDs can be purchased over the counter or prescribed in higher doses by a healthcare provider.
Disease-modifying antirheumatic drugs (DMARDs)
DMARDs are a class of medications used to treat rheumatoid arthritis and other autoimmune diseases. These medications work by modifying the underlying disease process, rather than just treating the symptoms. Examples of DMARDs include methotrexate, sulfasalazine, and hydroxychloroquine.
Pain management techniques
In addition to medication, various pain management techniques can be helpful in managing the symptoms of autoimmune diseases. These may include heat or cold therapy, physical therapy exercises, relaxation techniques, and alternative therapies such as acupuncture or massage.
Physical therapy
Physical therapy can be beneficial in managing the symptoms and improving the function of individuals with autoimmune diseases, particularly those affecting the joints and muscles. Physical therapists can develop customized exercise programs to improve strength, flexibility, and mobility, while also minimizing pain and preventing further joint damage.
Diet and lifestyle modifications
Certain dietary and lifestyle modifications may help manage autoimmune diseases. These can include following an anti-inflammatory diet, which emphasizes whole foods and minimizes processed foods and added sugars. Regular exercise, stress management techniques, and adequate sleep are also important for overall health and well-being.
Alternative and complementary therapies
Some individuals may find relief from autoimmune symptoms through alternative and complementary therapies. These may include acupuncture, herbal supplements, chiropractic care, or mind-body techniques such as meditation or yoga. It is important to discuss these therapies with a healthcare provider to ensure they are safe and effective in each specific case.
Clinical trials and experimental treatments
Participation in clinical trials can provide access to cutting-edge treatments and therapies for autoimmune diseases. Clinical trials are research studies that test the safety and efficacy of new medications, treatments, or approaches. Individuals may consider enrolling in clinical trials if they have exhausted other treatment options or if they are interested in contributing to the advancement of autoimmune disease research.
Managing autoimmune diseases
Patient education and support
Patient education is an essential component of managing autoimmune diseases. Understanding the nature of the disease, its triggers, and treatment options can empower individuals to actively participate in their own care. Support groups and online communities can also provide valuable emotional support, information sharing, and coping strategies for individuals living with autoimmune diseases.
Regular medical check-ups
Regular medical check-ups are important for individuals with autoimmune diseases to monitor disease progression, assess treatment efficacy, and detect any potential complications. These check-ups may involve physical examinations, blood tests, imaging studies, and discussions about symptom management and lifestyle modifications.
Adherence to treatment plan
Adherence to the prescribed treatment plan is crucial for managing autoimmune diseases effectively. This includes taking medications as directed, attending medical appointments, and following lifestyle and dietary recommendations. It is important to communicate with healthcare providers about any concerns or difficulties with treatment adherence.
Monitoring and managing symptoms
Individuals with autoimmune diseases should be vigilant in monitoring and managing their symptoms. Keeping a symptom journal and recording any changes or flare-ups can help identify triggers and patterns. It is important to communicate any changes or worsening of symptoms to healthcare providers for appropriate management.
Stress management techniques
Stress management techniques can help individuals with autoimmune diseases minimize the impact of stress on their symptoms and overall well-being. These techniques can include relaxation exercises, mindfulness meditation, deep breathing exercises, and engaging in activities that bring joy and relaxation.
Supportive therapies
In addition to medical treatments, supportive therapies can play a valuable role in managing autoimmune diseases. These may include physical or occupational therapy, counseling or psychotherapy to address emotional challenges, and assistive devices or adaptive equipment to improve daily functioning.
Potential complications
Organ damage
If left untreated or poorly controlled, autoimmune diseases can lead to organ damage. The immune system’s attack on healthy cells and tissues can cause long-term damage and dysfunction in affected organs. For example, rheumatoid arthritis can cause progressive joint destruction and deformities, while lupus can lead to kidney damage and other organ complications.
Secondary infections
Autoimmune diseases often require immune-suppressing medications to reduce inflammation and prevent damage. However, these medications can also weaken the immune system, increasing the risk of secondary infections. It is important for individuals with autoimmune diseases to take appropriate precautions and seek medical attention promptly if they develop signs of an infection.
Increased risk of certain cancers
Some autoimmune diseases, such as systemic lupus erythematosus or Sjögren’s syndrome, have been associated with an increased risk of certain types of cancer. Regular medical check-ups and monitoring can help detect any signs of cancer early, improving the chances of successful treatment.
Reduced quality of life
Autoimmune diseases can significantly impact the quality of life of individuals affected by these conditions. Chronic pain, physical limitations, and the unpredictability of symptoms can affect daily activities, employment, relationships, and overall well-being. It is important to address the physical, emotional, and social aspects of living with an autoimmune disease to enhance quality of life.
Advancements in autoimmune disease research
Identification of new autoimmune diseases
Advancements in autoimmune disease research have led to the identification of new autoimmune diseases. Researchers continue to uncover novel autoimmune conditions and expand our understanding of the underlying mechanisms that contribute to these diseases. This knowledge can lead to improved diagnosis and targeted treatments.
Improved understanding of disease mechanisms
Researchers have made significant progress in understanding the underlying mechanisms of autoimmune diseases. These mechanisms include dysregulation of the immune system, genetic factors, environmental triggers, and abnormalities in specific immune cells or molecules. The increased understanding of disease mechanisms can help guide the development of more effective treatments.
Development of targeted therapies
Targeted therapies have emerged as a promising approach for treating autoimmune diseases. These therapies aim to specifically target key components of the immune system involved in the disease process. For example, monoclonal antibodies that block specific cytokines or immune cells have shown success in treating conditions such as rheumatoid arthritis and psoriasis.
Personalized medicine approaches
Advances in technology and research have paved the way for personalized medicine approaches in autoimmune diseases. Personalized medicine takes into account an individual’s unique genetic and molecular profile, allowing for more precise diagnosis and treatment decisions. This approach can help optimize treatment response and reduce the risk of side effects.
Gene editing and gene therapies
Gene editing technologies, such as CRISPR-Cas9, hold promise for the future treatment of autoimmune diseases. These technologies allow for precise modifications of specific genes or genetic sequences involved in autoimmune diseases. Gene therapies are also being explored to modulate the immune system and restore normal immune function in affected individuals.

Prevention and risk reduction
Maintaining a healthy lifestyle
Maintaining a healthy lifestyle is important for overall health and may help reduce the risk of developing autoimmune diseases. This includes eating a balanced diet rich in fruits, vegetables, whole grains, and lean proteins, engaging in regular physical activity, avoiding tobacco use, and limiting alcohol consumption.
Avoiding known triggers
For individuals already diagnosed with an autoimmune disease, avoiding known triggers can help prevent exacerbations and manage symptoms. These triggers can include specific foods, environmental allergens, stressors, or infections. Identifying and avoiding these triggers, as well as adopting stress management techniques, can help minimize symptoms and disease flare-ups.
Early detection and intervention
Early detection and intervention are key in managing autoimmune diseases effectively. Recognizing early signs and symptoms, seeking medical attention promptly, and adhering to treatment plans can help prevent disease progression and minimize complications. Regular check-ups and monitoring can facilitate early detection and proactive management of autoimmune diseases.
Conclusion
Autoimmune diseases are complex conditions characterized by the immune system’s attack on healthy cells and tissues in the body. They can affect various organs and tissues, leading to a wide range of symptoms and potential complications. While the exact causes of autoimmune diseases are still not fully understood, genetic, environmental, and hormonal factors are believed to play a role.
Treatment options for autoimmune diseases aim to suppress the immune system, reduce inflammation, and manage symptoms. Advancements in research have led to the development of targeted therapies and personalized medicine approaches, offering hope for more effective treatments in the future.
Managing autoimmune diseases involves a multidisciplinary approach, including medication, lifestyle modifications, supportive therapies, and regular medical check-ups. Patient education, emotional support, and adherence to treatment plans are crucial for optimal management and maintaining quality of life.
By staying informed, seeking early intervention, and actively participating in their own care, individuals with autoimmune diseases can effectively manage their condition and lead fulfilling lives. Ongoing research and advancements hold promise for improved understanding, prevention, and treatment of autoimmune diseases in the future.

