In this article, we will explore the essential aspects of managing Inflammatory Bowel Disease (IBD) through diet and medication. With an aim to provide a comprehensive understanding of IBD, we will delve into the importance of maintaining a healthy diet and the role of medication in managing the symptoms. Whether you or a loved one has been diagnosed with IBD, this article will serve as a helpful guide to navigate through the complexities of managing this chronic condition. Let’s embark on this journey towards a better understanding of IBD and empowering yourself with the knowledge needed for effective management.
Overview of Inflammatory Bowel Disease (IBD)
Definition of IBD
Inflammatory Bowel Disease (IBD) refers to a group of chronic, inflammatory conditions that affect the digestive tract. It involves the inflammation of the lining of the intestines, which can cause various symptoms and complications. The two main types of IBD are Crohn’s disease and ulcerative colitis.
Types of IBD
-
Crohn’s disease: This type of IBD can affect any part of the gastrointestinal tract from the mouth to the anus. It can cause inflammation in patches, leading to symptoms such as diarrhea, abdominal pain, weight loss, and fatigue.
-
Ulcerative colitis: Unlike Crohn’s disease, ulcerative colitis mainly affects the colon and rectum. It causes continuous inflammation and ulcers in the inner lining of the colon, resulting in symptoms like abdominal pain, rectal bleeding, and frequent bowel movements.
Causes and risk factors
The exact cause of IBD is still unknown, but it is believed to involve a combination of genetic, environmental, and immune system factors. Some potential risk factors for developing IBD include a family history of the condition, certain genetic mutations, a malfunctioning immune system, and a history of smoking.
Symptoms of IBD
The symptoms of IBD can vary from person to person and depend on the type and severity of the condition. Common symptoms include diarrhea, abdominal pain and cramping, rectal bleeding, weight loss, fatigue, loss of appetite, and fever. It is essential to consult with a healthcare provider for a proper diagnosis if any of these symptoms are present.
Dietary Management for IBD
Importance of diet in IBD
Diet plays a vital role in the management of IBD. While there is no specific diet that works for everyone, making certain dietary modifications can help improve symptoms and reduce inflammation. A well-balanced diet can provide essential nutrients, support gut healing, and maintain overall health.
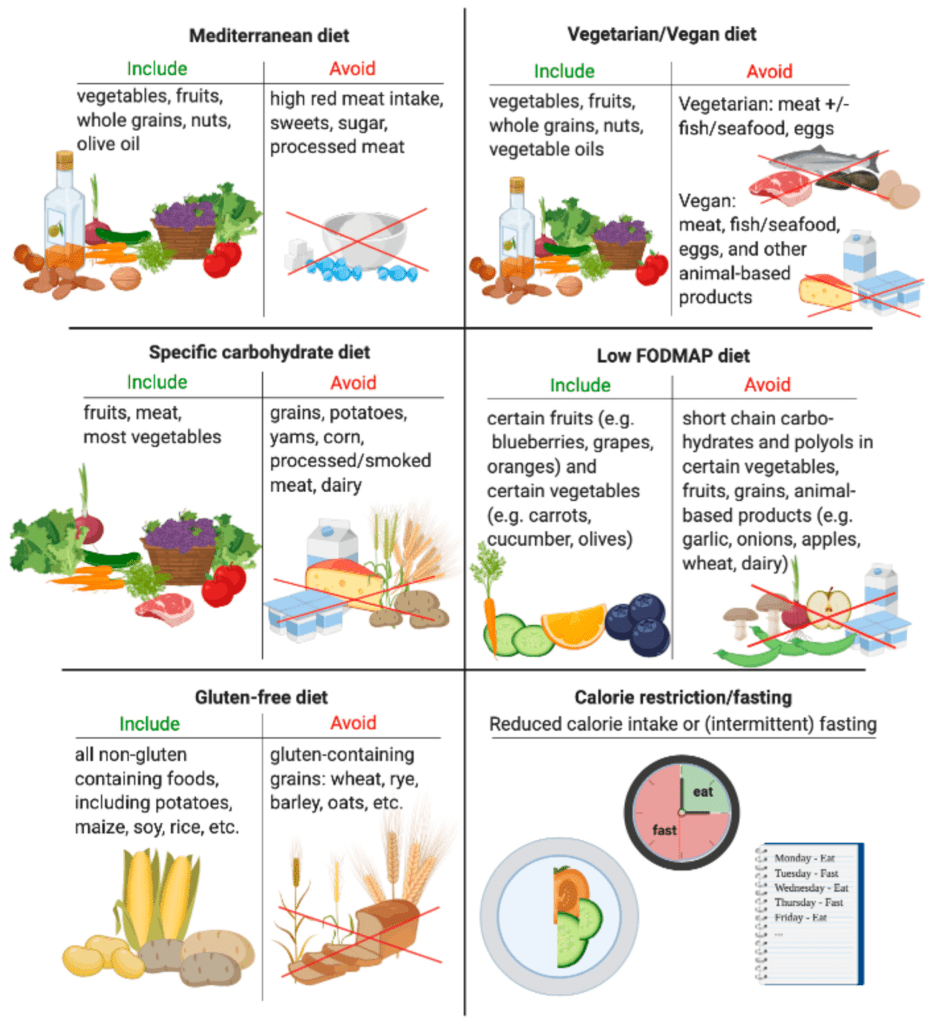
General dietary recommendations
Some general dietary recommendations for individuals with IBD include:
- Eating small, frequent meals to ease digestion and reduce symptoms.
- Avoiding trigger foods that worsen symptoms, such as high-fat foods, spicy foods, caffeine, and alcohol.
- Incorporating a variety of fruits, vegetables, lean proteins, whole grains, and healthy fats into the diet.
- Staying hydrated by drinking an adequate amount of fluids throughout the day.
Specific dietary considerations for Crohn’s disease
For individuals with Crohn’s disease, certain dietary considerations can be helpful, such as:
- Consuming foods that are easily digestible, such as cooked vegetables, tender meats, and well-cooked grains.
- Limiting fiber intake during active flare-ups, as it can worsen symptoms.
- Maintaining a food diary to identify trigger foods and monitor symptom improvement.
Specific dietary considerations for ulcerative colitis
For individuals with ulcerative colitis, specific dietary considerations may include:
- Eating smaller, more frequent meals to reduce the strain on the digestive system.
- Avoiding foods that are known to aggravate symptoms, such as spicy foods, dairy products, and high-fiber foods.
- Ensuring an adequate intake of calcium and vitamin D, as individuals with ulcerative colitis may be at risk of deficiencies.
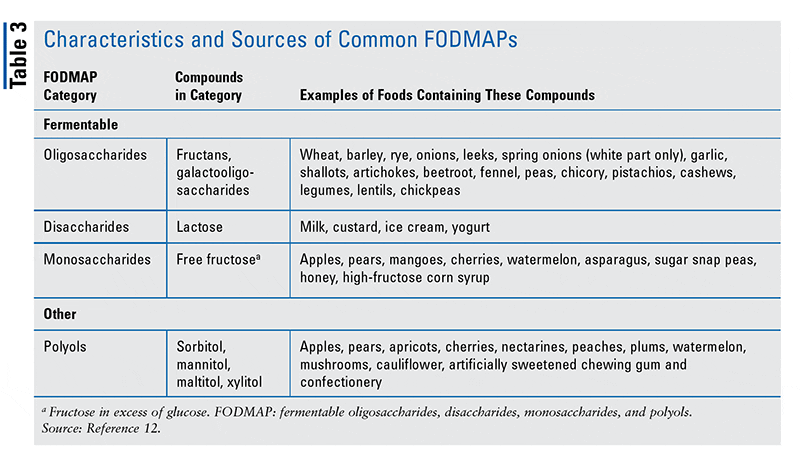
The role of fiber in IBD
Fiber plays a crucial role in maintaining a healthy digestive system, but it can be problematic for individuals with IBD, especially during flare-ups. While fiber can promote bowel regularity and provide various health benefits, it may aggravate symptoms like diarrhea and abdominal pain in some people with IBD. It is important to work closely with a healthcare provider or registered dietitian to determine the appropriate amount and type of fiber for individual needs.
The role of fat in IBD
Fat is an essential nutrient that provides energy and supports the absorption of certain vitamins. However, high-fat foods can exacerbate symptoms in individuals with IBD, particularly those with Crohn’s disease. Lowering the intake of greasy, fried foods and opting for healthier fats found in sources like avocados, nuts, and olive oil can be beneficial for managing symptoms.
Hydration and IBD
Staying hydrated is crucial for individuals with IBD, as diarrhea and increased fluid loss can lead to dehydration. Drinking an adequate amount of fluids throughout the day, such as water, herbal teas, and broths, can help maintain hydration levels. It is important to talk to a healthcare provider about specific hydration needs, especially during flare-ups or when experiencing increased bowel movements.
Medication Management for IBD
Goal of medication management
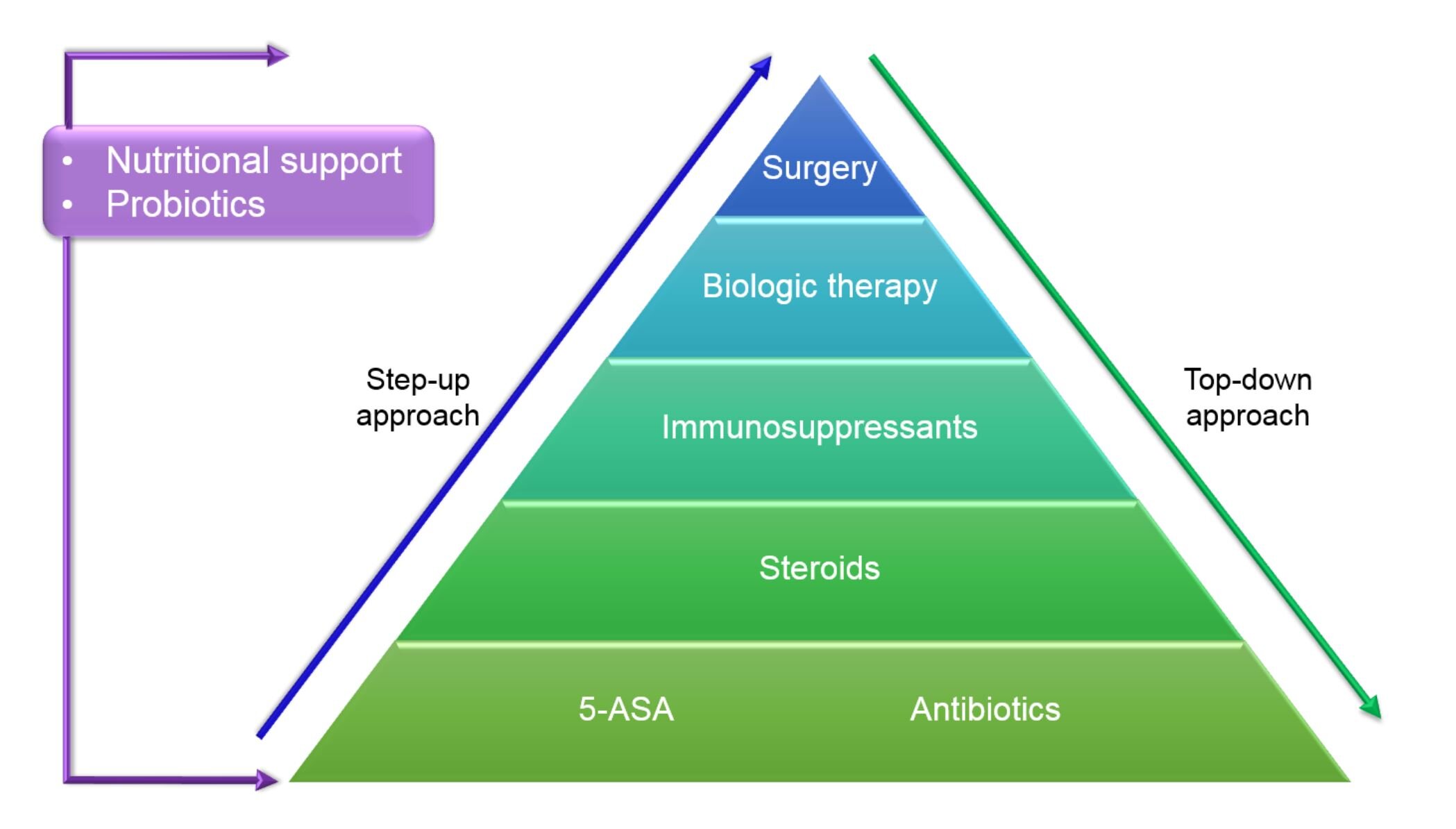
The goal of medication management for IBD is to reduce inflammation, alleviate symptoms, achieve and maintain remission, and prevent disease complications. Different types of medications may be prescribed depending on the type and severity of the IBD.
Types of medications for IBD
-
Anti-inflammatory drugs: These medications, such as aminosalicylates and corticosteroids, help reduce inflammation in the digestive tract and can be effective in managing mild to moderate IBD.
-
Immunosuppressants: These medications, such as azathioprine and methotrexate, work by suppressing the immune system’s response, thereby reducing inflammation. They are generally used for individuals with moderate to severe IBD.
-
Biologics: Biologic medications, such as infliximab and adalimumab, target specific molecules involved in the inflammatory process. They are often prescribed for individuals with moderate to severe IBD who have not responded well to other treatments.
-
Antibiotics: Antibiotics may be used in certain cases of IBD, such as when there is an infection or abscess. They can help reduce inflammation and prevent complications.
-
Pain relievers: Over-the-counter pain relievers, such as acetaminophen, may provide temporary relief from abdominal pain, but they should be used cautiously and under the guidance of a healthcare provider, as some pain relievers can worsen symptoms.
Managing medication side effects
Some medications used to manage IBD can have side effects. It is important to discuss any potential side effects with a healthcare provider and to regularly monitor for them. If side effects occur, healthcare providers can adjust the medication dosage or explore alternative treatment options. Open communication with healthcare providers is key in managing medication side effects and ensuring that the benefits of the medication outweigh any potential risks.
Lifestyle Modifications for IBD
Stress management
Stress can exacerbate symptoms and contribute to disease flares in individuals with IBD. Therefore, implementing effective stress management techniques is crucial. This may include practices such as deep breathing exercises, meditation, yoga, and engaging in hobbies or activities that promote relaxation.
Exercise and physical activity
Regular exercise and physical activity can have numerous benefits for individuals with IBD. Exercise can help reduce inflammation, improve mood, boost energy levels, and promote overall well-being. It is important to consult with a healthcare provider before starting an exercise regimen, as they can provide guidance based on individual needs and limitations.
Smoking cessation
Smoking is a known risk factor for developing and exacerbating IBD. Quitting smoking is essential for individuals with IBD, as it can help improve symptoms, reduce the risk of complications, and increase the effectiveness of medication treatments. Healthcare providers can provide resources and support for smoking cessation.
Sleep and rest
Adequate sleep and rest are important for individuals with IBD to support healing and overall well-being. Establishing a regular sleep schedule, creating a relaxing bedtime routine, and ensuring a comfortable sleep environment can contribute to improved sleep quality. If symptoms like pain or frequent bowel movements disrupt sleep, healthcare providers can offer strategies to manage these symptoms.
Alternative therapies
Some individuals with IBD explore alternative therapies alongside conventional medical treatments to manage symptoms and improve overall well-being. Alternative therapies such as acupuncture, herbal remedies, probiotics, and mind-body techniques may have potential benefits. It is crucial to consult with healthcare providers before incorporating any alternative therapies to ensure they are safe and do not interfere with the prescribed treatment plan.

Collaboration with Healthcare Providers
Importance of healthcare team
Collaboration with a multidisciplinary healthcare team is key in managing IBD effectively. This team may include gastroenterologists, dietitians, pharmacists, nurses, and mental health professionals. Each member of the healthcare team plays a specific role in supporting individuals with IBD, and their expertise and guidance are crucial in developing personalized treatment plans.
The role of gastroenterologists
Gastroenterologists are specialized physicians who diagnose and manage diseases of the gastrointestinal tract, including IBD. They play a central role in the diagnosis, treatment, and ongoing management of IBD. Gastroenterologists may conduct diagnostic tests, prescribe medications, monitor disease progression, and make treatment recommendations based on individual needs.
The role of dietitians
Registered dietitians with expertise in IBD can provide valuable guidance on dietary management. They can help individuals identify trigger foods, develop personalized meal plans, ensure adequate nutrient intake, and address any nutritional deficiencies. Dietitians work closely with individuals to help them make practical and sustainable dietary changes that support overall health and manage IBD symptoms.
The role of pharmacists
Pharmacists are highly knowledgeable about medications used in the management of IBD. They can provide information about potential drug interactions, help individuals understand medication instructions and potential side effects, and offer guidance on the safe use and storage of medications. Pharmacists play a vital role in ensuring medication management is safe and effective.
Open communication with healthcare providers
Open and honest communication with healthcare providers is essential in managing IBD effectively. It is important to share any concerns, symptoms, or changes in condition with the healthcare team. They rely on this information to make informed decisions about treatment adjustments, medication management, and overall care.
Monitoring and Adjusting Management Strategies
Regular follow-up appointments
Regular follow-up appointments with healthcare providers are crucial in monitoring the progress of IBD and making any necessary adjustments to the management plan. These appointments allow healthcare providers to assess disease activity, address any concerns or questions, and evaluate the effectiveness of medications and lifestyle modifications.
Laboratory tests and imaging
Laboratory tests, such as blood work and stool samples, provide valuable information about disease activity, nutritional status, and potential complications. Imaging studies, such as colonoscopies or imaging scans, may also be used to evaluate the bowel and assess disease progression. These tests help healthcare providers make informed decisions about treatment options and adjustments.
Keeping a symptom and food diary
Keeping a symptom and food diary can be a helpful tool in managing IBD. Recording symptoms, food intake, medication usage, and other relevant information can provide valuable insights into triggers and patterns. This information can guide healthcare providers in making adjustments to the treatment plan and identifying potential problem areas.
Making adjustments to diet and medication
The management of IBD is often a continuous process that requires adjustments to diet and medication as needed. Certain foods or medications that were well-tolerated in the past may suddenly become problematic. Healthcare providers, in collaboration with individuals with IBD, can help identify these changes and make appropriate adjustments to optimize symptom management and overall well-being.
When to seek immediate medical attention
It is important to be aware of the signs and symptoms that may require immediate medical attention. Severe abdominal pain, persistent vomiting, high fever, rectal bleeding, and rapid weight loss are all red flags that should prompt seeking prompt medical advice. Timely intervention can help prevent complications and ensure appropriate treatment.
Potential Complications and Prevention
Complications of untreated or poorly managed IBD
If left untreated or poorly managed, IBD can lead to various complications. Some potential complications of IBD include bowel obstructions, fistulas (abnormal connections between organs or tissues), abscesses, malnutrition, anemia, osteoporosis, and an increased risk of colorectal cancer. With proper management and regular monitoring, the risk of complications can be reduced.
Strategies for prevention and early intervention
Several strategies can help prevent and intervene early in the course of IBD. These include:
- Early diagnosis and treatment of IBD to help manage symptoms and prevent disease progression.
- Adherence to prescribed medications and regular follow-up appointments with healthcare providers.
- Implementing dietary modifications to reduce inflammation and support gut health.
- Avoiding known triggers, such as smoking and stress, that can worsen symptoms.
- Engaging in regular physical activity to maintain overall health and reduce disease activity.
Surgical options for IBD
In some cases, surgery may be necessary to manage complications or severe cases of IBD. Surgical interventions can involve removing damaged or diseased portions of the intestine, creating a temporary or permanent ileostomy or colostomy, or repairing fistulas or abscesses. Surgical options are typically considered when medications and other conservative treatments are ineffective in controlling symptoms or preventing complications.
Support and Resources for IBD Patients
Patient support groups
Joining patient support groups can provide individuals with IBD a sense of community, shared experiences, and emotional support. These groups often offer a safe space for individuals to connect, exchange information and insights, and gain valuable support from others who understand the challenges of living with IBD.
Counseling and therapy
Counseling and therapy can be beneficial for individuals with IBD, especially when dealing with the emotional and psychological impact of the condition. Therapy can help individuals develop coping strategies, manage stress, and address any concerns or fears related to IBD. Mental health professionals can provide guidance and support tailored to individual needs.
Online resources and forums
Online resources and forums can be a valuable source of information and support for individuals with IBD. Various reputable websites and forums provide reliable information, personal stories, and access to experts in the field of IBD. However, it is important to verify the credibility of any online information and consult with healthcare providers for personalized advice.
Educational materials
Educational materials, such as brochures, pamphlets, and books, can provide individuals with IBD and their families with a better understanding of the condition. These resources can cover a wide range of topics, including disease management, dietary recommendations, medication information, and strategies for maintaining overall health and well-being.
Importance of Self-Care for IBD
Understanding personal triggers
Understanding personal triggers is essential for individuals with IBD to manage their condition effectively. By identifying specific foods, stressors, or lifestyle factors that worsen symptoms, individuals can make informed choices and take proactive steps to minimize flare-ups and optimize symptom management.
Managing stress and emotional well-being
Stress can significantly impact the course of IBD and exacerbate symptoms. Therefore, managing stress and prioritizing emotional well-being is crucial. Practicing stress management techniques, engaging in activities that promote relaxation, and seeking support from mental health professionals can help individuals better cope with the emotional challenges of living with IBD.
Maintaining a balanced lifestyle
Adopting a balanced lifestyle is vital for individuals with IBD to optimize their overall health and well-being. This encompasses not only dietary and medication management but also engaging in regular physical activity, getting adequate sleep, managing stress, and practicing self-care. Maintaining a balanced lifestyle supports disease management and can lead to a better quality of life.
Seeking support from loved ones
Building a network of support from loved ones can make a significant difference in managing IBD. Friends and family can provide emotional support, help with practical matters, and offer understanding during challenging times. Open communication and educating loved ones about the condition can foster a supportive environment that contributes to increased well-being.
Conclusion
Inflammatory Bowel Disease (IBD), including Crohn’s disease and ulcerative colitis, is a chronic condition that requires comprehensive management. Diet modification, medication management, lifestyle adjustments, collaboration with healthcare providers, and self-care all play critical roles in effectively managing IBD. Each individual’s approach to IBD management should be individualized and based on personal needs and preferences. By implementing these strategies and staying proactive in managing the condition, individuals with IBD can promote overall health and well-being, minimize symptoms, and live fulfilling lives.