Living with a chronic illness can be challenging, but when you combine it with the effects of climate change, the risks to your health may become even more daunting. In this article, we will explore the ways in which chronic illness and climate change intersect, and discuss potential adaptation strategies to help you navigate these challenges. From understanding the increased vulnerability to identifying effective coping mechanisms, this article aims to provide valuable insights and support for individuals grappling with the unique combination of chronic illness and climate change.
Health Risks of Climate Change
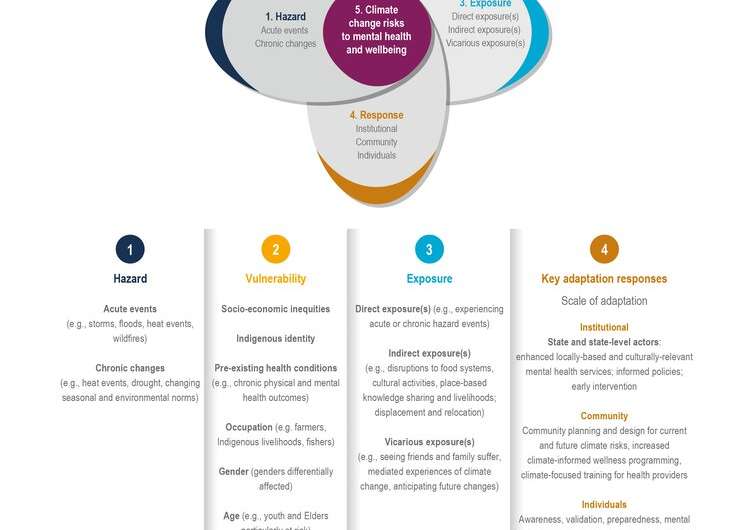
Climate change is not just an environmental issue; it also poses significant threats to human health. As temperatures continue to rise, the risk of heat-related illnesses is becoming increasingly prevalent. Heatwaves, often lasting longer and becoming more intense due to climate change, can lead to dehydration, heat exhaustion, and even heatstroke. It is crucial to recognize the warning signs of these illnesses and take steps to stay cool and hydrated during hot weather.
Another health risk associated with climate change is the worsening air quality, which can have severe consequences for respiratory health. As temperatures rise, there is an increased prevalence of air pollutants such as ozone and particulate matter, exacerbating respiratory problems like asthma and chronic obstructive pulmonary disease (COPD). Individuals with pre-existing respiratory conditions should be particularly cautious and seek medical advice on how to manage their symptoms effectively.
Climate change also plays a role in the spread of vector-borne diseases. As the geographical range of disease-carrying vectors, such as mosquitoes and ticks, expands due to changes in temperature and rainfall patterns, so does the risk of contracting illnesses like malaria, dengue fever, and Lyme disease. Implementing vector control measures, such as eliminating breeding grounds and using insect repellents, becomes crucial in preventing the transmission of these diseases.
Furthermore, climate change affects waterborne diseases and food safety, primarily through extreme weather events. Flooding and heavy rainfall can lead to contaminated water sources, contributing to the spread of diseases like cholera and dysentery. Additionally, the warming of oceans can impact the occurrence and distribution of harmful algal blooms, leading to seafood contamination. Ensuring access to safe drinking water and practicing proper food safety measures becomes essential to prevent these health risks.
Impact of Climate Change on Chronic Illness
Climate change not only poses acute health risks but can also worsen chronic illnesses. For individuals with existing chronic conditions, such as cardiovascular disease, diabetes, and allergies, climate change can exacerbate their symptoms and increase the severity of their conditions. Hotter temperatures and poorer air quality can put additional stress on the body, making it more challenging to manage these chronic illnesses effectively.
In addition to aggravating existing conditions, climate change also increases the risk of new onset chronic illnesses. For example, exposure to extreme heat can lead to heat-related conditions like heat cramps, heat exhaustion, and heatstroke. Prolonged exposure to pollutants can also contribute to the development of respiratory diseases in individuals previously unaffected. The rising prevalence of chronic illnesses due to climate change necessitates a proactive approach to healthcare and prevention.
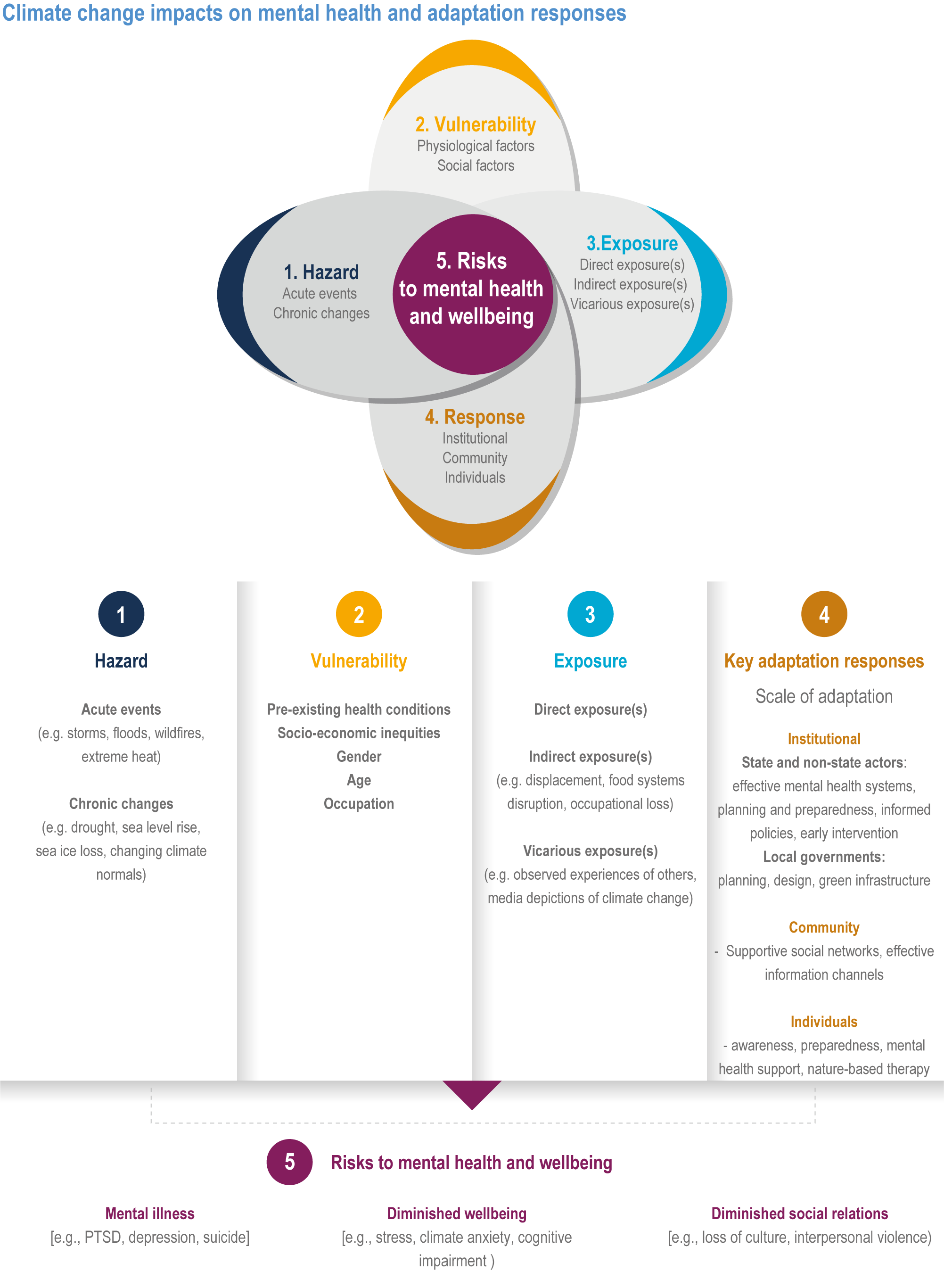
Climate change can also have significant impacts on mental health. As individuals face the adverse effects of extreme weather events, displacement, or loss of homes and loved ones, their mental well-being may be severely affected. Anxiety, depression, and post-traumatic stress disorder are all potential mental health consequences of climate change. Recognizing and addressing these psychological effects is essential to ensuring comprehensive healthcare in the face of climate change.
Adapting to the Effects of Climate Change
To mitigate the health risks associated with climate change, it is crucial to implement adaptation strategies at both individual and systemic levels.
Medical management and treatment adjustments are vital for individuals with chronic illnesses to cope with the changing climate. Healthcare providers need to stay informed about the latest research on climate-related health issues to provide the most effective care. They can assist patients in understanding the specific impacts of climate change on their conditions and make appropriate adjustments to their treatment plans.
Heat stress prevention and management are essential for individuals vulnerable to heat-related illnesses. This involves taking measures such as seeking cool environments, staying hydrated, and using cooling techniques like fans or air conditioning. Educating individuals on recognizing the signs of heat-related illnesses and proper hydration can encourage proactive heat stress prevention.
Improving indoor air quality is crucial in combatting the worsening air quality associated with climate change. Measures such as proper ventilation, air filtration, and reducing exposure to indoor pollutants can help individuals manage their respiratory conditions effectively.
Vector control and prevention measures are essential in limiting the spread of vector-borne diseases. This includes eliminating breeding grounds for mosquitoes, using protective clothing and insect repellents, and promoting community awareness about the importance of vector control.
Ensuring safe drinking water access and practicing food safety measures are vital in preventing waterborne diseases. Proper sanitation infrastructure, regular testing of water sources, and educating individuals about safe food handling practices are key components of this adaptation strategy.
Building Resilience and Support Systems
Building community resilience and support systems is crucial for mitigating the health risks associated with climate change.
Engaging communities through education and awareness programs is essential in promoting proactive healthcare practices. By informing individuals about the health risks of climate change and providing guidance on adaptation strategies, communities can better prepare and protect themselves.
Enhanced healthcare infrastructure is necessary to meet the growing healthcare demands resulting from climate change. This includes increasing the capacity of healthcare facilities, ensuring adequate resources for emergency response, and strengthening healthcare networks to facilitate effective communication and coordination during extreme weather events.
Psychological and emotional support should also be integrated into healthcare systems to address the mental health consequences of climate change. Mental health professionals can play a significant role in providing counseling and therapy to individuals experiencing anxiety, depression, or trauma related to climate change.
Social support networks are essential for individuals coping with chronic illnesses and the impacts of climate change. Connecting patients with support groups or online communities can provide a sense of belonging and understanding, reducing feelings of isolation and anxiety.
Healthcare System Preparedness
To effectively address the health risks of climate change, healthcare systems must be prepared to incorporate climate change considerations into their planning and operations.
Integrating climate change considerations into healthcare planning involves assessing vulnerability and implementing measures to adapt to changing climate conditions. This includes developing protocols for extreme weather events, such as heatwaves or hurricanes, and ensuring adequate resources and personnel are available to respond to these emergencies.
Developing early warning systems can help healthcare systems and individuals prepare for impending climate-related health risks. These systems can provide timely alerts and guidance, enabling individuals to take necessary precautions and healthcare facilities to mobilize resources for effective response.
Enhancing surveillance and monitoring systems is crucial for tracking and understanding the health impacts of climate change. By collecting and analyzing data on climate-related illnesses, healthcare systems can identify trends, allocate resources strategically, and implement targeted interventions to prevent and manage these health risks.
Training healthcare professionals on climate-related health issues is vital to ensure that medical professionals are equipped with the knowledge and skills to effectively address the health risks of climate change. This includes educating healthcare providers on the connections between climate change and health, as well as providing training on best practices for prevention, diagnosis, and treatment.
Promoting Environmental Sustainability
To mitigate the health risks of climate change, promoting environmental sustainability is essential.
Advocacy for clean energy and reduced greenhouse gas emissions plays a critical role in minimizing the impacts of climate change on human health. By supporting renewable energy sources and advocating for policies that prioritize the reduction of greenhouse gas emissions, individuals and communities can contribute to a healthier and more sustainable future.
Promotion of sustainable transportation is another key strategy to reduce the environmental impacts of transportation and improve air quality. By encouraging walking, biking, and public transportation, individuals can reduce their carbon footprint while improving their own health.
Mitigating climate change through lifestyle changes, such as reducing energy consumption and waste, can have significant environmental and health benefits. By making conscious choices to minimize resource consumption and reduce waste, individuals can contribute to a more sustainable and resilient future.
Policy and Governance Recommendations
To effectively address the health risks of climate change, policy and governance measures are essential.
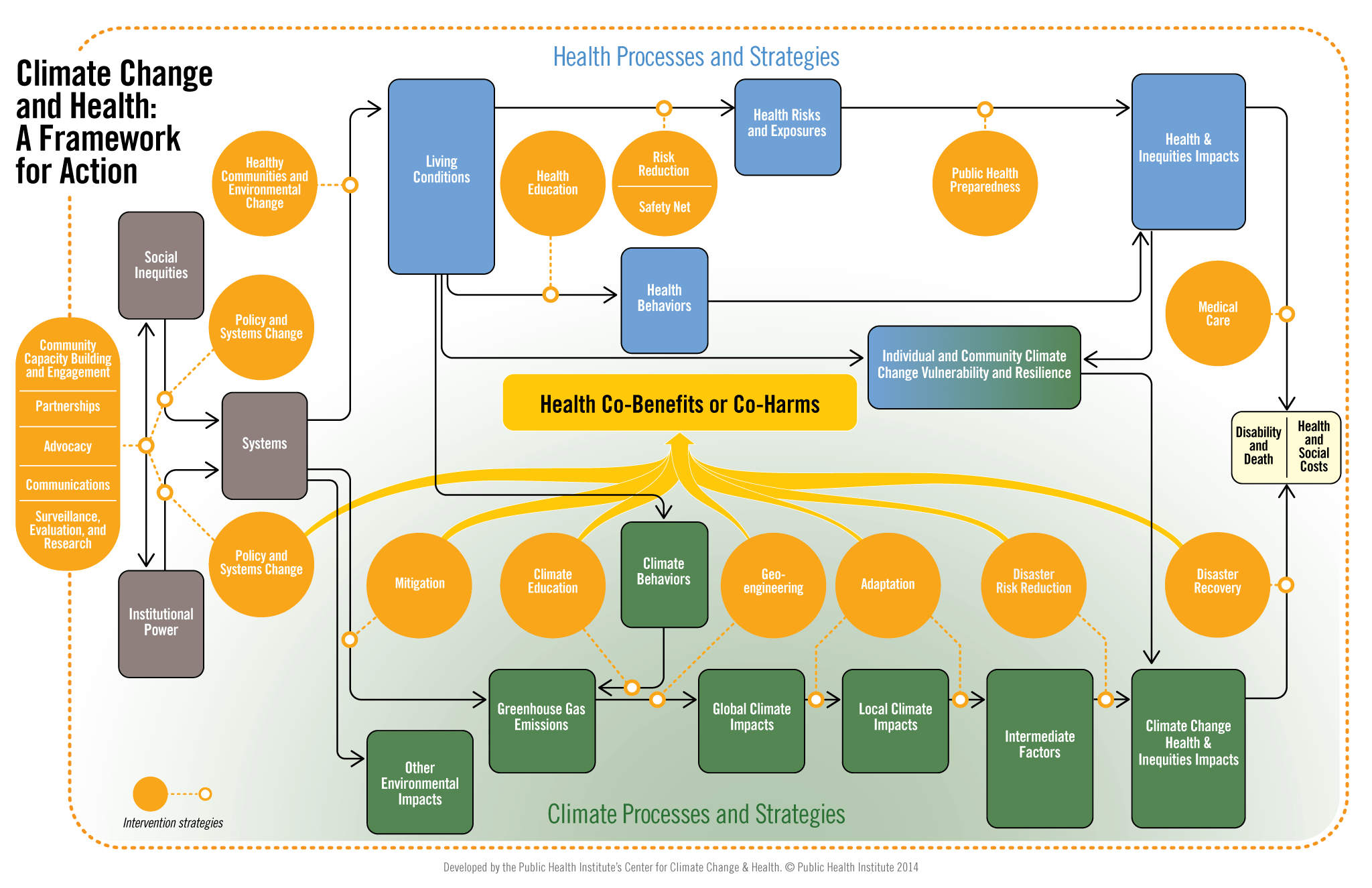
Integration of health and climate policies is crucial for ensuring a coordinated and comprehensive approach to climate change adaptation. By aligning health policies with climate goals, governments can prioritize the health and well-being of their citizens in the face of environmental challenges.
Establishing climate-resilient communities involves implementing policies and regulations that promote sustainable infrastructure, disaster preparedness, and community engagement. By investing in resilient infrastructure and encouraging community participation, governments can foster adaptive communities that are better prepared to withstand the impacts of climate change.
Funding research and innovation for climate change adaptation is vital for developing effective strategies and interventions. Governments, international organizations, and private entities should invest in research and innovation to better understand the health impacts of climate change and develop innovative solutions for adaptation.
International cooperation and collaboration are critical in addressing the global challenges of climate change. By sharing knowledge, resources, and best practices, countries can work together to develop and implement effective policies and strategies to protect public health in the face of climate change.
Empowering Individuals with Chronic Illnesses
Individuals with chronic illnesses also play a crucial role in adapting to the health risks of climate change.
Implementing self-care strategies is essential for individuals to effectively manage their chronic illnesses in a changing climate. This includes adherence to medication regimens, proper monitoring of symptoms, and making necessary lifestyle adjustments to promote overall well-being.
Building support networks can provide individuals with the necessary emotional, social, and practical support to navigate the challenges of climate change and chronic illness. Connecting with others who share similar experiences can offer valuable insights, coping strategies, and a sense of empowerment.
Education and awareness about climate change impacts are important for individuals to understand the specific risks and vulnerabilities they may face. By being informed about the potential health risks and adaptation strategies, individuals can take appropriate actions to protect their health.
Advocacy for improved healthcare and climate policies empowers individuals to contribute to positive change. By voicing their concerns, sharing their experiences, and participating in advocacy efforts, individuals can influence policy decisions and promote a healthcare system that is responsive to the impacts of climate change.

Research and Data Collection
Research and data collection are fundamental in understanding the complex interactions between climate change and chronic illnesses.
Investigating the links between climate change and chronic illnesses is crucial to determine the specific mechanisms through which climate change impacts human health. Research can help identify the pathways by which climate change exacerbates chronic conditions and inform targeted interventions.
Monitoring health indicators and climate change impacts is essential for tracking trends and assessing the effectiveness of adaptation strategies. By collecting data on climate-related illnesses, hospital admissions, and emergency department visits, researchers can identify patterns and trends that guide public health interventions.
Long-term studies on adaptation strategies and outcomes are necessary to evaluate the effectiveness and sustainability of interventions. By conducting rigorous research with long-term follow-up, researchers can provide evidence-based recommendations for adapting to the health risks of climate change.
Conclusion
Climate change poses significant risks to human health, particularly for individuals with chronic illnesses. The increasing prevalence of heat-related illnesses, worsening air quality, spread of vector-borne diseases, and waterborne diseases necessitate proactive measures to adapt to the impacts of climate change. Adapting to climate change requires a comprehensive approach that involves medical management, prevention strategies, building resilience, and promoting environmental sustainability. It is crucial for healthcare systems, policymakers, and individuals to work together to address the health risks of climate change and ensure a healthy and sustainable future for all.

