Living with Crohn’s Disease can be challenging, but with the right treatment options and coping strategies, managing the condition becomes much easier. This article provides valuable insights into understanding Crohn’s Disease, explores various treatment options available, and offers helpful strategies to cope with the disease. By empowering you with knowledge and practical tips, we aim to help you take control of your health and live a fulfilling life despite the challenges of Crohn’s Disease.
Understanding Crohn’s Disease
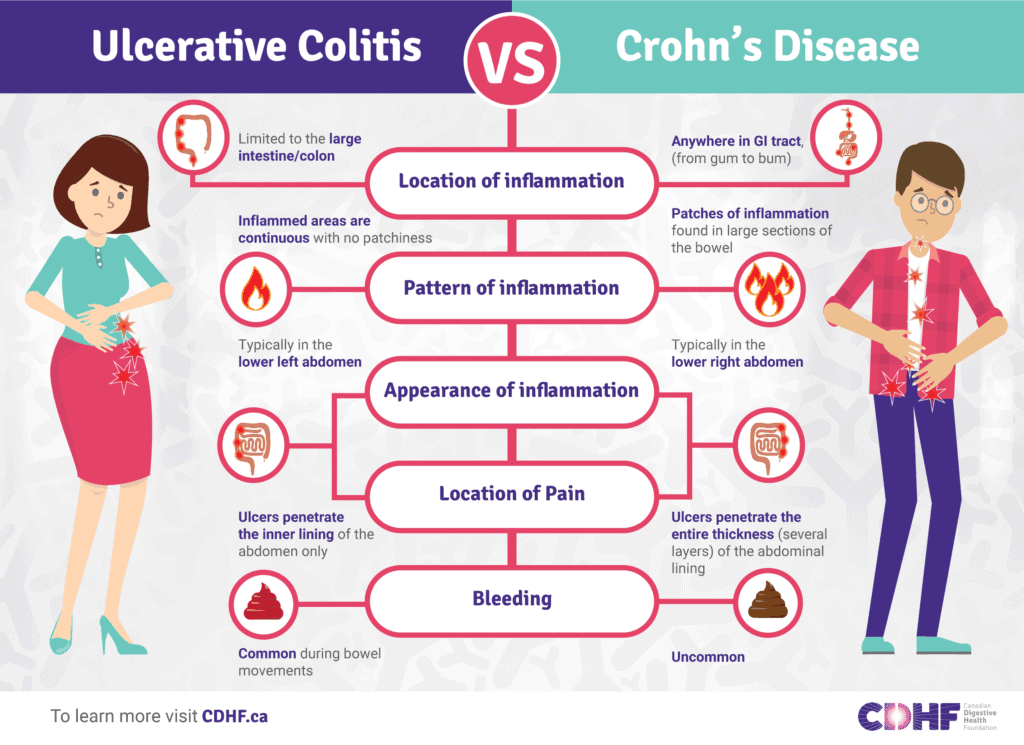
Crohn’s disease is a chronic inflammatory bowel disease that affects the lining of the digestive tract. It can affect any part of the gastrointestinal tract, from the mouth to the anus, but most commonly occurs in the small intestine and the colon. While the exact cause of Crohn’s disease is still unknown, it is believed to be a combination of genetic, environmental, and immune system factors.
What is Crohn’s Disease?
Crohn’s disease is an autoimmune condition in which the body’s immune system mistakenly attacks healthy cells in the digestive tract. This chronic inflammation can lead to various symptoms, such as abdominal pain, diarrhea, fatigue, weight loss, and malnutrition. It can also cause complications like strictures, ulcers, fistulas, and abscesses. Crohn’s disease is a lifelong condition with no known cure, but it can be managed through a combination of treatment options and lifestyle changes.
Causes and Risk Factors
The exact cause of Crohn’s disease is still unknown, but researchers believe that a combination of genetic, environmental, and immune system factors play a role. Certain genes have been associated with an increased risk of developing Crohn’s disease, although not everyone with these genes will develop the condition. Environmental factors such as smoking, diet, and exposure to certain bacteria or viruses may also contribute to the development of Crohn’s disease. Additionally, an overactive immune system may mistakenly attack the healthy cells in the digestive tract, leading to chronic inflammation.
Symptoms and Diagnosis
The symptoms of Crohn’s disease can vary from person to person and depend on the location and severity of the inflammation. Common symptoms include abdominal pain, diarrhea, rectal bleeding, weight loss, fatigue, and fever. Some individuals may also experience complications like joint pain, skin rashes, eye inflammation, and liver problems. To diagnose Crohn’s disease, a healthcare provider will perform a physical examination, review the patient’s medical history, and order diagnostic tests such as blood tests, stool tests, imaging studies (e.g., endoscopy, colonoscopy), and sometimes biopsy.
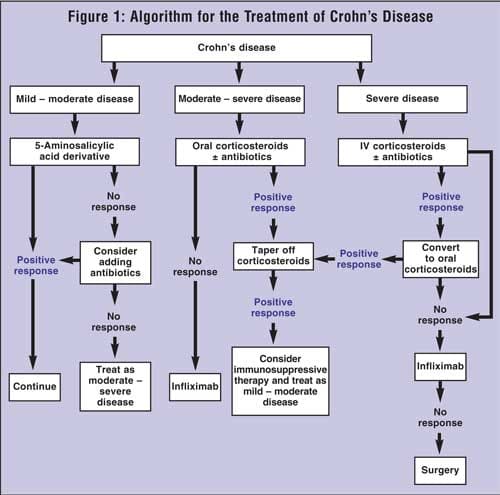
Treatment Options
While there is no cure for Crohn’s disease, various treatment options are available to help manage symptoms, reduce inflammation, and prevent complications. The choice of treatment depends on the severity and location of the disease, as well as the individual’s overall health and preferences.
Medication
Medication is often the first line of treatment for Crohn’s disease. It aims to reduce inflammation, control symptoms, and induce and maintain remission. There are different types of medications used, including:
Anti-inflammatory Drugs:
These drugs help reduce inflammation in the digestive tract. Examples include mesalamine, sulfasalazine, and corticosteroids. They are typically used for mild to moderate cases of Crohn’s disease.
Immunosuppressants:
Immunosuppressant drugs work by suppressing the immune system to reduce inflammation. They are used for moderate to severe cases and to maintain remission. Examples include azathioprine, methotrexate, and cyclosporine.
Biologic Therapies:
Biologics target specific proteins involved in the inflammatory process. They are typically used for moderate to severe cases that do not respond to other medications. Examples include infliximab, adalimumab, and vedolizumab.
Antibiotics:
In some cases, antibiotics may be prescribed to treat bacterial infections or to control inflammation.
Dietary Changes
Dietary changes can play a significant role in managing Crohn’s disease. While there is no specific diet that works for everyone, some common dietary approaches include:
Elimination Diets:
These diets involve eliminating specific foods or food groups that may aggravate symptoms. Common triggers include dairy, gluten, and high-fiber foods. It is essential to work with a healthcare provider or dietitian to ensure proper nutrition while avoiding trigger foods.
Low-Residue Diet:
A low-residue diet aims to reduce the amount of undigested food and fiber in the digestive tract, which can help reduce symptoms like diarrhea and abdominal pain. This diet involves avoiding high-fiber foods like nuts, seeds, and raw fruits and vegetables.
FODMAP Diet:
The FODMAP diet focuses on reducing the intake of specific carbohydrates that are poorly absorbed in the small intestine, leading to increased gas, bloating, and diarrhea. Examples of foods high in FODMAPs include certain fruits, vegetables, grains, and dairy products.
Probiotics and Prebiotics:
Probiotics are beneficial bacteria that can help restore the balance of gut flora and improve digestion. Prebiotics are non-digestible fibers that promote the growth of beneficial bacteria. Both probiotics and prebiotics may have a role in managing Crohn’s disease, but more research is needed.
Nutritional Therapy
In some cases, nutritional therapy may be recommended to manage Crohn’s disease. This approach focuses on providing adequate nutrition while giving the digestive tract a chance to heal. There are two main types of nutritional therapy:
Enteral Nutrition:
Enteral nutrition involves consuming liquid formulas or specially formulated diets that provide all the necessary nutrients. It is administered through a feeding tube or consumed orally. This approach can help reduce inflammation and promote healing in the digestive tract.
Parenteral Nutrition:
Parenteral nutrition is reserved for individuals with severe Crohn’s disease who cannot tolerate oral or enteral nutrition. It involves receiving nutrients intravenously, bypassing the digestive tract altogether.

Surgical Options
In some cases, surgery may be necessary to manage complications or improve the quality of life for individuals with Crohn’s disease. Surgical options for Crohn’s disease include:
Strictureplasty:
A strictureplasty is a surgical procedure that widens narrowed sections of the intestine without removing them. It can be an effective treatment for strictures or narrowings caused by scar tissue.
Bowel Resection:
Bowel resection involves removing the affected portion of the intestine and rejoining the healthy segments. This procedure is commonly used for removing sections with severe inflammation, fistulas, or obstructions.
Colectomy:
A colectomy involves the removal of the entire colon. It may be necessary in cases where the colon is extensively affected by Crohn’s disease or to treat complications such as severe bleeding or perforation.
Colostomy or Ileostomy:
In some cases, a surgical procedure may lead to the creation of a colostomy or ileostomy. These procedures involve diverting the bowel through an opening in the abdomen, allowing waste to exit the body through a stoma into a collection bag.
Complementary and Alternative Medicine
In addition to traditional medical treatments, some individuals with Crohn’s disease may explore complementary and alternative medicine (CAM) approaches to manage their symptoms. While the evidence for these therapies is limited, some options that may be considered include:
Acupuncture:
Acupuncture involves the insertion of thin needles into specific points on the body. It is believed to help relieve pain and reduce inflammation.
Herbal Supplements:
Some herbal supplements, such as aloe vera, turmeric, and Boswellia, may have anti-inflammatory properties. However, it is essential to consult a healthcare provider before starting any herbal supplements, as they may interact with other medications.
Mind-Body Techniques:
Mind-body techniques, such as meditation, guided imagery, and relaxation exercises, may help reduce stress and improve overall well-being.
Probiotics:
Probiotics are beneficial bacteria that can help restore balance to the gut flora. They may help reduce inflammation and improve digestion.
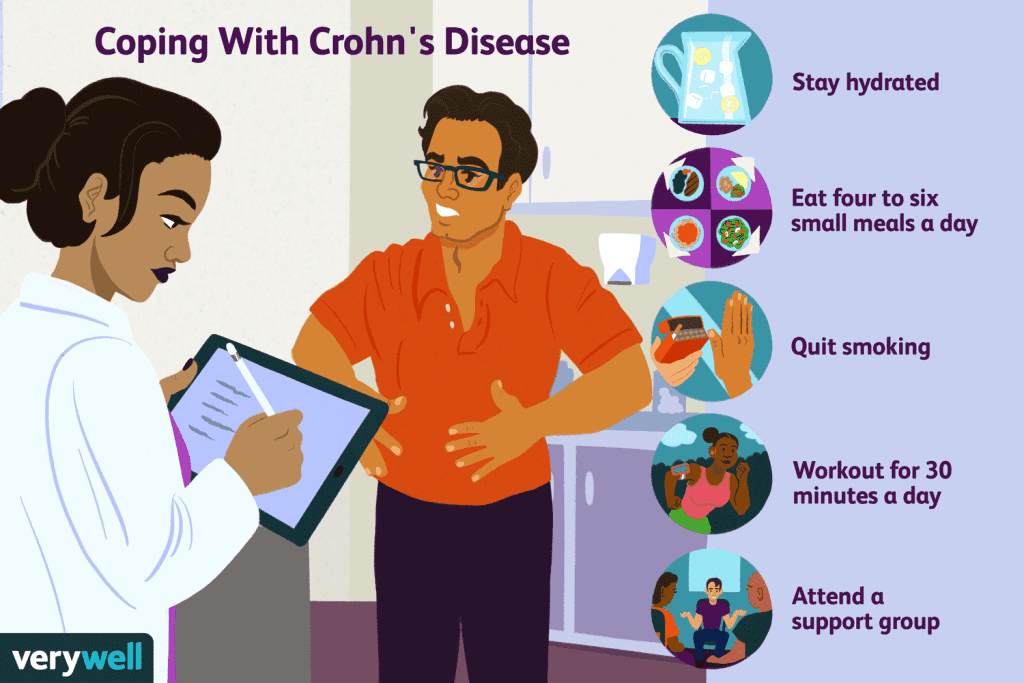
Coping Strategies
Living with Crohn’s disease can be challenging, both physically and emotionally. Here are some coping strategies that can help:
Educating Oneself About the Disease:
Learning about Crohn’s disease can help individuals understand their condition better and make informed decisions about treatment and lifestyle.
Building a Support System:
Having a strong support system, consisting of family, friends, and healthcare providers, can provide the necessary emotional and practical support.
Managing Stress:
Stress can exacerbate symptoms and trigger flare-ups in Crohn’s disease. Managing stress through techniques like yoga, meditation, or engaging in hobbies can be beneficial.
Seeking Therapy or Counseling:
Therapy or counseling can provide a safe space to discuss the emotional challenges of living with Crohn’s disease and develop coping strategies.
Supportive Therapies
In addition to medical and surgical treatments, supportive therapies can help improve the quality of life for individuals with Crohn’s disease. Some of these therapies include:
Psychological Therapy:
Psychological therapy, such as cognitive-behavioral therapy (CBT), may help individuals manage stress and cope with the emotional challenges of living with a chronic illness.
Physical Therapy:
Physical therapy can help improve strength, flexibility, and overall physical well-being. It may also be beneficial for managing pain and recovering from surgery.
Occupational Therapy:
Occupational therapy focuses on improving daily functioning and quality of life. It can help individuals develop strategies to manage fatigue, maintain employment, and engage in meaningful activities.
Speech Therapy:
Speech therapy may be necessary if Crohn’s disease affects the vocal cords or speech-related muscles. It can help individuals with speech or swallowing difficulties.
Pain Management Techniques:
Managing pain is a crucial aspect of living with Crohn’s disease. Pain management techniques such as heat or cold therapy, relaxation techniques, and medication can provide relief.

Lifestyle Changes
Making certain lifestyle changes can be beneficial for managing Crohn’s disease and reducing symptoms. These changes include:
Managing Diet and Nutrition:
Working with a healthcare provider or dietitian to develop a balanced diet that suits individual needs and avoids trigger foods can help manage symptoms.
Regular Exercise:
Regular exercise can help improve overall physical and mental well-being. However, it is essential to choose low-impact activities and listen to your body’s limits.
Quitting Smoking:
Smoking can worsen symptoms and increase the risk of complications in Crohn’s disease. Quitting smoking is crucial for managing the condition effectively.
Getting Adequate Rest and Sleep:
Fatigue is a common symptom of Crohn’s disease. Getting enough rest and ensuring quality sleep can help manage fatigue and promote overall well-being.
In conclusion, understanding and managing Crohn’s disease requires a comprehensive approach that includes medical treatment, lifestyle modifications, and coping strategies. By working closely with healthcare providers, individuals with Crohn’s disease can find the most appropriate treatment options and develop strategies to enhance their quality of life. Remember that each person’s journey with Crohn’s disease is unique, and it may take time to find the right combination of treatments and coping techniques. Stay positive, stay informed, and reach out for support when needed.

