Living with chronic conditions in a rural setting can present unique challenges when it comes to accessing adequate healthcare and community resources. In this article, we explore the various obstacles faced by individuals living with chronic illnesses in rural areas and discuss the importance of available care and community support. By understanding the specific needs of those living in remote areas, we can work towards bridging the gap and ensuring that individuals with chronic conditions have the resources they require to live fulfilling lives. Living with chronic conditions in a rural setting can present unique challenges when it comes to accessing healthcare and community resources. In this article, we will explore the importance of access to care in rural areas, the barriers that individuals with chronic conditions may face, and the impact of limited access on their health and well-being.
Barriers to Accessing Care in Rural Areas
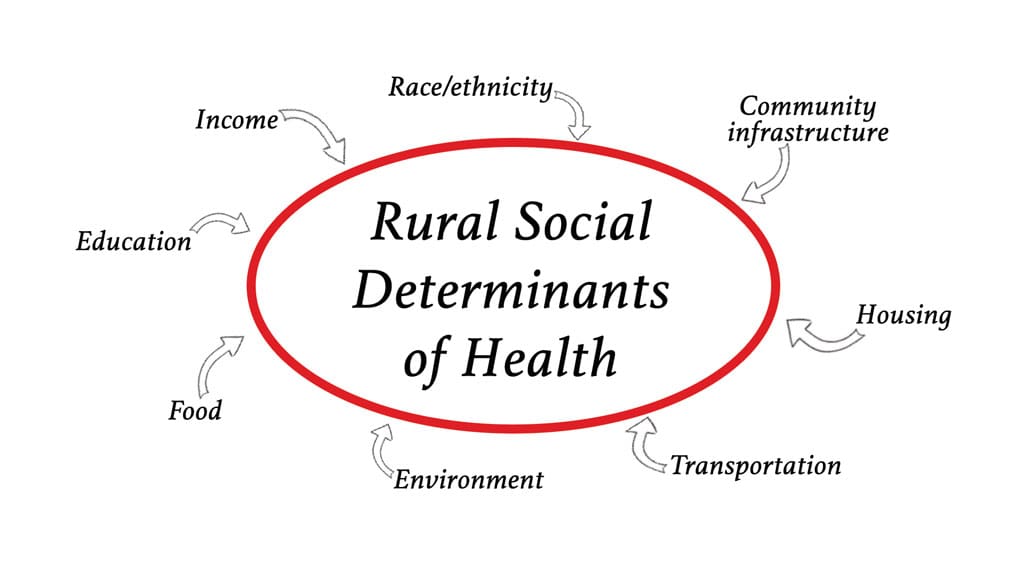
Rural areas often lack the same healthcare infrastructure and resources as urban areas, leading to barriers in accessing care. One of the main challenges is the limited availability of healthcare providers in these areas. Without enough doctors, nurses, and specialists, individuals with chronic conditions may have difficulty finding the necessary care.
Additionally, rural areas often lack transportation options, making it difficult for individuals to travel to medical appointments. Public transportation is often scarce or non-existent, leaving those without personal vehicles at a significant disadvantage. This lack of transportation can result in missed appointments and delayed or inadequate treatment.
Another barrier to accessing care in rural areas is the distance individuals must travel to reach healthcare facilities. Rural residents may have to travel long distances to reach the nearest hospital or specialist, adding extra time, cost, and inconvenience to their healthcare journey. This can be especially challenging for individuals with chronic conditions who require frequent medical visits.
Impact of Limited Access to Care on Individuals with Chronic Conditions
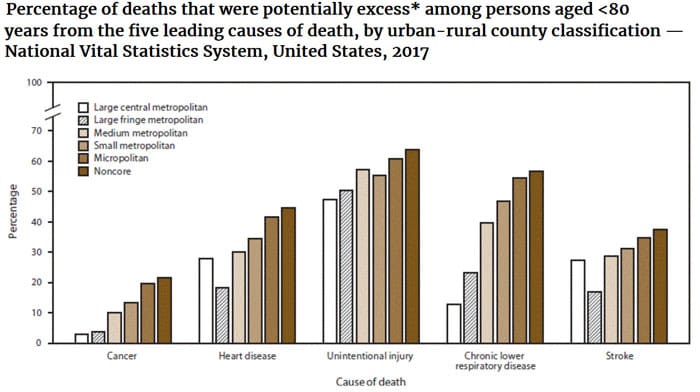
Limited access to care can have a profound impact on individuals with chronic conditions. Without timely access to healthcare providers, individuals may experience worsening symptoms, delays in diagnosis, and inadequate management of their conditions. This can lead to poorer health outcomes, decreased quality of life, and increased healthcare costs in the long run.
Furthermore, individuals with chronic conditions often require ongoing care and management. Without access to regular check-ups, medication refills, and necessary treatments, their conditions may become uncontrolled, leading to flare-ups, complications, and hospitalizations. Limited access to preventive care and health education can also contribute to the development of preventable complications.
The lack of community resources in rural areas can further exacerbate the challenges faced by individuals with chronic conditions. Without local support groups, educational workshops, and organizations dedicated to chronic disease management, individuals may feel isolated and struggle to find the resources and support they need to effectively manage their conditions.
Challenges Faced by Healthcare Providers in Rural Areas
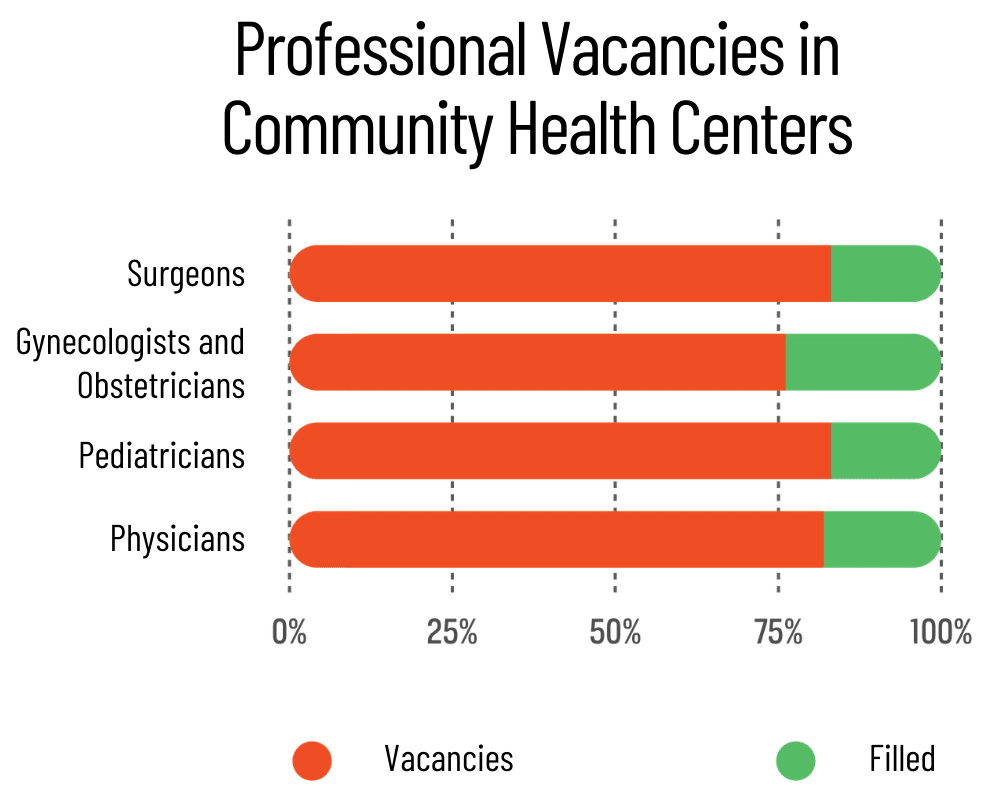
Healthcare providers in rural areas face their own set of challenges when it comes to delivering care. One significant challenge is the shortage of healthcare professionals in these areas. Rural communities often struggle to attract and retain doctors, nurses, and specialists, leading to a higher workload and limited access to specialized care for individuals with chronic conditions.
In addition to the shortage of healthcare providers, rural areas may also experience a lack of funding and resources for healthcare facilities. Limited funding means fewer medical equipment, outdated technology, and inadequate infrastructure, which can hinder the delivery of quality care. Faced with these challenges, healthcare providers often have to be resourceful and find innovative ways to overcome these obstacles.
Strategies to Overcome Challenges Faced by Healthcare Providers in Rural Areas
Despite the challenges, healthcare providers in rural areas have developed strategies to improve access to care for individuals with chronic conditions. One effective strategy is the utilization of telemedicine. Telemedicine allows healthcare providers to connect with patients remotely, providing consultations, monitoring, and even diagnosis from a distance. This has proven to be beneficial in rural areas where travel distances can be burdensome.
Healthcare providers in rural areas also collaborate with other professionals and organizations to ensure comprehensive care for individuals with chronic conditions. They establish partnerships with local hospitals and clinics to provide specialized care through outreach services or scheduled visits. By leveraging these collaborations, healthcare providers can bring necessary services closer to rural communities, reducing travel and improving access to care.
Role of Telemedicine in Providing Care in Rural Areas
Telemedicine plays a crucial role in providing care to individuals in rural areas. Through telemedicine, individuals can access healthcare providers and specialists without leaving their communities, saving time and money. This is particularly important for those with chronic conditions who may require frequent check-ups or consultations.
Telemedicine also allows for remote monitoring of chronic conditions, such as diabetes, hypertension, or heart disease. With the use of wearable devices and digital health apps, individuals can track their health measurements, such as blood pressure, blood glucose levels, or heart rate, and share the data with healthcare providers. This enables timely interventions and adjustments to treatment plans, improving the management of chronic conditions.
While telemedicine has significant benefits, challenges in implementing this technology in rural areas remain. Limited access to reliable internet connections and technological literacy among the population can hinder the widespread adoption of telemedicine. However, efforts are being made to address these challenges through infrastructure improvements and education initiatives.
Importance of Community Support for Individuals with Chronic Conditions
Community support plays a vital role in the well-being of individuals with chronic conditions in rural areas. Having a supportive network of peers, healthcare providers, and community resources can make a significant difference in their ability to manage their conditions and improve their quality of life.
Local support groups and organizations dedicated to specific chronic conditions provide a safe space for individuals to connect with others who share similar experiences. These groups offer emotional support, share information and resources, and provide a sense of belonging. Being part of a community that understands and empathizes with their struggles can be incredibly empowering for individuals with chronic conditions.
Churches and community centers also play an important role in supporting individuals with chronic conditions. Many churches offer support groups, educational programs, and even transportation assistance for their congregants. Community centers often host workshops, exercise classes, and social events tailored to the needs of individuals with chronic conditions. These resources foster a sense of community and provide additional avenues for support and connection.

Educational Workshops and Programs
Educational workshops and programs are crucial for promoting self-management and empowerment among individuals with chronic conditions. These workshops offer practical information, tools, and strategies to help individuals better understand their conditions, manage their symptoms, and make informed decisions about their healthcare.
Rural areas may face challenges in accessing such workshops due to limited resources and funding. However, healthcare providers, community organizations, and local leaders can collaborate to organize educational programs in their communities. By leveraging existing community spaces, such as churches or community centers, and partnering with healthcare providers, these workshops can provide valuable knowledge and empower individuals to take control of their health.
Lack of Public Transportation in Rural Areas
Transportation can be a significant barrier to accessing healthcare services in rural areas. Many rural communities lack reliable and affordable public transportation, leaving individuals with chronic conditions without a means to travel to medical appointments. This can result in missed appointments, delayed care, and inadequate treatment.
The lack of public transportation options poses a particular challenge for individuals who do not own a personal vehicle. They may depend on family members, friends, or neighbors for transportation, which can be unreliable and burdensome for both parties involved. Seeking alternative transportation options becomes crucial in ensuring that individuals with chronic conditions can access the care they need.
Transportation Assistance Programs
To overcome the transportation barrier, many rural areas have implemented transportation assistance programs. These programs aim to provide affordable and reliable transportation to medical appointments for individuals who are unable to drive themselves. They often utilize volunteer drivers or partner with local transportation services to offer reduced rates.
Collaboration with local clinics and hospitals is also important in addressing transportation challenges. By organizing shared transportation services or shuttle programs, healthcare providers can ensure that individuals can get to and from medical appointments conveniently and safely. When various healthcare facilities work together, they can optimize transportation resources and minimize the burden on patients.
Advancements in Remote Monitoring Technologies
Advancements in remote monitoring technologies have revolutionized the management of chronic conditions. These technologies allow individuals to measure and track their health data from the comfort of their own homes, reducing the need for frequent in-person visits and providing timely interventions.
Remote monitoring devices, such as blood pressure cuffs, glucometers, or wearable fitness trackers, can automatically transmit data to healthcare providers. This enables them to monitor an individual’s health trends, identify potential issues, and make necessary adjustments to treatment plans. Remote monitoring takes advantage of modern technology to bridge the gap between patients and healthcare providers, especially in rural areas.
Benefits of Remote Monitoring for Individuals with Chronic Conditions
Remote monitoring offers numerous benefits for individuals with chronic conditions living in rural areas. Firstly, it allows for the early detection of health issues or changes in symptoms. By collecting and analyzing real-time health data, healthcare providers can intervene promptly before a condition worsens, potentially preventing hospitalizations or emergency visits.
Secondly, remote monitoring reduces the need for frequent travel to healthcare facilities. This is especially advantageous for individuals with limited transportation options or those living in remote areas. With remote monitoring, individuals can manage their conditions from the comfort of their homes, reducing the time, cost, and effort associated with in-person appointments.
Thirdly, remote monitoring promotes self-management and patient empowerment. By having access to their health data, individuals can become more actively involved in their care. They can make lifestyle adjustments, follow treatment plans more effectively, and gain a deeper understanding of how their behaviors impact their health outcomes.
Challenges in Implementing Remote Monitoring in Rural Areas
While remote monitoring has immense potential, several challenges exist in implementing this technology in rural areas. One of the main challenges is the lack of access to reliable internet connections. Rural areas often have limited or slow internet service, hindering the real-time transmission of health data. Addressing this challenge requires infrastructure improvements and broadband expansion in rural communities.
In addition to the internet connectivity issue, some individuals in rural areas may lack the necessary technological literacy to use remote monitoring devices effectively. Education and training programs can play a vital role in overcoming this challenge. Healthcare providers and community organizations can offer workshops and resources to help individuals learn how to use remote monitoring technologies and interpret their health data accurately.
Financial Challenges Faced by Individuals with Chronic Conditions
Living with a chronic condition often comes with significant financial burden. Individuals may face increased healthcare costs, including medication expenses, co-pays for doctor visits, and insurance deductibles. These financial challenges can impact an individual’s ability to access necessary care and manage their conditions effectively.
Furthermore, individuals with chronic conditions may experience a decrease in productivity and income due to the limitations imposed by their health. They may have to reduce working hours, take time off for medical appointments, or even leave their jobs altogether. This loss of income further compounds the financial strain they face.
Government Programs and Subsidies
To alleviate the financial burden faced by individuals with chronic conditions, various government programs and subsidies are available. Programs such as Medicaid and Medicare provide healthcare coverage for eligible individuals, including those with chronic conditions. These programs can significantly reduce out-of-pocket expenses and ensure access to necessary medications and treatments.
Additionally, individuals with chronic conditions may qualify for Social Security Disability Insurance (SSDI) or Supplemental Security Income (SSI) if their conditions prevent them from working. These programs provide financial assistance to individuals with disabilities, offering a safety net during times of financial hardship.
Non-Profit Organizations Providing Financial Aid
Non-profit organizations also play a crucial role in providing financial assistance to individuals with chronic conditions. These organizations offer grants, scholarships, and financial aid programs to help individuals cover medical expenses, purchasing necessary equipment, or accessing specialized care.
Non-profit organizations often work in collaboration with healthcare providers and community organizations to identify individuals in need and provide support. Many of these organizations are dedicated to specific chronic conditions, ensuring that individuals receive targeted assistance and resources tailored to their unique needs.

Limited Mental Health Resources in Rural Areas
Access to mental health resources is often limited in rural areas, presenting significant challenges for individuals with chronic conditions who require additional mental health support. Mental health services, such as therapists, psychiatrists, and support groups, may be scarce, leaving individuals without the necessary resources to address their mental health needs.
The shortage of mental health providers in rural areas can result in long wait times for appointments, inadequate access to specialized care, and a lack of understanding and awareness about mental health issues. This lack of resources may lead to underdiagnosis and undertreatment of mental health conditions among individuals with chronic conditions.
Integration of Mental Health Services into Primary Care
To address the shortage of mental health resources in rural areas, the integration of mental health services into primary care settings is crucial. By integrating mental health into primary care, individuals with chronic conditions can receive comprehensive and coordinated care, addressing both their physical and mental health needs simultaneously.
Primary care providers can receive training in mental health screening, assessment, and basic counseling techniques to provide initial support to individuals. They can also collaborate with specialists through telepsychology or telepsychiatry services to ensure timely access to mental health expertise. This integrated approach eliminates the need for individuals to travel long distances to access mental health services, improving their overall well-being.
Telepsychology and Online Therapy Options
Telepsychology and online therapy options have emerged as valuable resources for individuals with chronic conditions in rural areas. These services allow individuals to access mental health support from the comfort of their homes, eliminating travel barriers and reducing the stigma associated with seeking mental health care.
Telepsychology enables individuals to have therapy sessions with licensed mental health professionals through secure video conferencing or telecommunication platforms. Online therapy options, such as text-based counseling or self-guided programs, provide additional flexibility and convenience for individuals who prefer asynchronous communication or have limited access to video conferencing technology.
These virtual mental health services not only expand access to care but also cater to the unique needs of individuals with chronic conditions in rural areas. They offer a safe and confidential space for individuals to receive support, manage their mental health, and work towards a better quality of life.
Creating a Network of Individuals with Chronic Conditions
Building a supportive community is crucial for individuals with chronic conditions in rural areas. Creating a network of individuals facing similar challenges can provide emotional support, a sense of belonging, and opportunities for shared knowledge and experiences. This peer support plays a significant role in empowering individuals to take control of their health and well-being.
Healthcare providers, community organizations, and online platforms can facilitate the creation of these networks. They can organize support groups, online forums, or social media communities where individuals can connect, share their stories, seek advice, and inspire one another. Through these networks, individuals can realize that they are not alone in their struggles and find strength in their shared experiences.
Importance of Peer Support
Peer support offers unique benefits for individuals with chronic conditions. Peers who have experienced similar challenges can provide practical advice, tips for self-management, and strategies for coping with the emotional and physical aspects of their conditions. Peer support also helps individuals feel understood and validated, reducing feelings of isolation and stigma.
By actively engaging in peer support, individuals can gain valuable knowledge about their conditions, learn from others’ experiences, and discover new resources and coping strategies. Peer support has been shown to improve self-confidence, self-care behaviors, and overall psychological well-being among individuals with chronic conditions.
Organizing Community Events and Activities
Organizing community events and activities centered around chronic conditions can further enhance the supportive network and resources available in rural areas. These events create opportunities for education, engagement, and socialization, fostering a sense of community and empowerment for individuals with chronic conditions.
Community organizations, healthcare providers, and local leaders can collaborate to organize educational workshops, wellness fairs, or awareness campaigns. These events can offer information, screenings, and free resources related to chronic disease management. They can also provide social activities, such as walks, exercise classes, or support group meetings, that encourage physical activity, social interaction, and peer support.
Promoting Inclusivity and Understanding
Promoting inclusivity and understanding within rural communities can significantly impact the well-being of individuals with chronic conditions. It is essential to reduce the stigma associated with chronic conditions and mental health issues, fostering an environment where individuals feel comfortable seeking care and accessing community resources.
Education and awareness campaigns can play a crucial role in promoting inclusivity and understanding. By disseminating accurate information about chronic conditions, their impact, and management strategies, individuals can develop a better understanding and empathy towards those living with these conditions. This understanding can help reduce judgment, misconceptions, and isolation, creating a more supportive and accepting community.
Importance of Advocating for Rural Healthcare
Advocacy for rural healthcare is essential to ensure that individuals with chronic conditions have equal access to care and resources regardless of their geographical location. By raising awareness and advocating for the unique challenges faced by rural communities, individuals, healthcare providers, and community organizations can bring about positive changes and improvements in healthcare infrastructure.
Advocacy efforts can involve engaging with policymakers, attending public meetings or hearings, and sharing personal stories and experiences. By highlighting the gaps in care and the importance of rural healthcare, advocates can influence policy decisions, funding allocations, and resource distribution. Through collective advocacy, individuals with chronic conditions in rural areas can have their voices heard and their needs addressed.
Policy Changes to Improve Access to Care and Resources
Policy changes are necessary to improve access to care and resources for individuals with chronic conditions in rural areas. Policymakers can implement initiatives that encourage healthcare professionals to practice in rural areas, such as loan forgiveness programs or financial incentives. They can also allocate funding for infrastructure improvements, telehealth initiatives, and the recruitment and training of healthcare providers in rural communities.
In addition to workforce and infrastructure improvements, policymakers can also develop policies that prioritize rural healthcare needs in decision-making processes. This includes considering the unique challenges faced by rural communities in allocating resources, designing interventions, and implementing programs aimed at improving health outcomes.
Collaboration with Healthcare Providers and Policymakers
Collaboration between healthcare providers and policymakers is crucial in driving positive change for individuals with chronic conditions in rural areas. Healthcare providers can provide valuable insights and expertise about the challenges faced by their patients, the gaps in care, and the necessary resources for effective management.
By working together, healthcare providers and policymakers can develop policies and programs that address the specific needs of rural communities. They can identify opportunities for telehealth implementation, advocate for increased funding for healthcare infrastructure, and develop training programs to attract and retain healthcare professionals in rural areas. This collaboration ensures that policy changes are evidence-based, feasible, and aligned with the needs of the community.
Investment in Healthcare Facilities and Resources
Investing in healthcare facilities and resources is crucial for improving access to care for individuals with chronic conditions in rural areas. The development and expansion of healthcare facilities, such as clinics, hospitals, and specialized centers, ensure the availability of comprehensive care services closer to rural communities, reducing travel burdens.
Investments should also focus on improving the quality and capacity of healthcare infrastructure in rural areas. This includes ensuring access to state-of-the-art medical equipment, digital health technologies, and reliable internet connections for telehealth services. By investing in healthcare facilities and resources, rural areas can attract healthcare professionals, alleviate financial barriers, and enhance the overall health infrastructure.
Attracting Healthcare Professionals to Rural Areas
Attracting and retaining healthcare professionals in rural areas is crucial for addressing the shortage of providers and improving access to care. Various strategies can be employed to encourage healthcare professionals to practice in rural areas, such as offering loan forgiveness programs or providing scholarships for individuals committed to working in underserved communities.
Rural healthcare organizations can also develop mentorship and support programs for healthcare professionals, particularly those new to practicing in rural areas. These programs can help them navigate the unique challenges and build a sense of community within the healthcare workforce. By fostering a supportive environment, rural areas can increase the likelihood of healthcare professionals staying and contributing to the long-term health of the community.
Telehealth Initiatives and Their Impact
Telehealth initiatives have a tremendous impact on improving access to care for individuals with chronic conditions in rural areas. Telehealth encompasses various technologies, including telemedicine and remote monitoring, that allow individuals to connect with healthcare providers remotely, reducing travel burdens and increasing access to specialized care.
Telehealth initiatives offer numerous benefits for individuals with chronic conditions, including access to virtual consultations, the ability to remotely monitor health data, and increased convenience. Through telehealth, individuals can receive timely care, manage their conditions effectively, and improve their overall health outcomes.
Furthermore, telehealth initiatives can contribute to cost savings for both individuals and healthcare systems. By reducing the need for in-person appointments, hospitalizations, and emergency visits, telehealth can lead to significant cost reductions. This is particularly important for individuals with chronic conditions who may require ongoing care and monitoring.
In conclusion, access to care and community resources is of utmost importance for individuals with chronic conditions living in rural areas. The barriers faced by rural communities in accessing healthcare can have a profound impact on individuals’ health outcomes and quality of life. However, strategies such as telemedicine, transportation assistance programs, and the integration of mental health services into primary care can address these challenges and improve access to care. Building a supportive community, advocating for policy changes, and investing in healthcare infrastructure are key to ensuring that individuals with chronic conditions in rural areas receive the care and resources they need. With concerted efforts from healthcare providers, policymakers, and community organizations, individuals can live fulfilling lives despite their chronic conditions in a rural setting.
