Living with a chronic blood disorder can be challenging, but with the right knowledge and coping strategies, it is possible to manage the condition and lead a fulfilling life. This article provides valuable insights and practical tips to help you understand the intricacies of chronic blood disorders and navigate the physical and emotional difficulties associated with them. From explaining the different types of blood disorders to offering coping mechanisms and support resources, this article aims to empower you with the tools you need to effectively manage your condition and enhance your overall well-being.

Types of Chronic Blood Disorders
Anemia
Anemia is a common chronic blood disorder that occurs when your body doesn’t have enough healthy red blood cells to deliver oxygen to your tissues. There are various types of anemia, including iron deficiency anemia, which is caused by a lack of iron in the body, and vitamin deficiency anemia, which occurs due to a deficiency in certain vitamins, such as vitamin B12 or folate. Other types of anemia may be caused by underlying medical conditions, such as kidney disease or certain types of cancer.
Hemophilia
Hemophilia is an inherited blood disorder that affects the body’s ability to clot blood. People with hemophilia have lower levels of clotting factors, which are proteins in the blood that help stop bleeding. This can lead to prolonged bleeding even from minor injuries or no apparent cause. Hemophilia is usually inherited and primarily affects males, although females can also carry the genetic mutation and pass it on to their children.
Thrombophilia
Thrombophilia is a chronic blood disorder characterized by an increased tendency to develop blood clots in veins and arteries. It can be caused by inherited genetic mutations or acquired factors. People with thrombophilia may experience blood clots in their legs (deep vein thrombosis) or lungs (pulmonary embolism), which can be life-threatening if not properly managed. Certain medical conditions, such as cancer or pregnancy, can increase the risk of developing thrombophilia.
Causes of Chronic Blood Disorders
Inherited genetic mutations
Many chronic blood disorders, such as hemophilia and certain types of anemia, are caused by inherited genetic mutations. These mutations can affect the production or function of certain blood components, leading to abnormal blood clotting or low red blood cell count. Genetic counseling can be beneficial in identifying and understanding these inherited conditions, as it helps individuals and families make informed decisions about their health and future generations.
Autoimmune conditions
Some chronic blood disorders, such as autoimmune hemolytic anemia and immune thrombocytopenia, are caused by autoimmune conditions. In these disorders, the body’s immune system mistakenly attacks its own red blood cells or platelets, leading to their destruction and subsequent health problems. The underlying causes of autoimmune conditions are not fully understood, but it is believed that a combination of genetic and environmental factors play a role in their development.
Medication side effects
Certain medications, such as those used in chemotherapy or to treat autoimmune disorders, can have side effects that impact the blood and its components. For example, some medications may suppress the production of red blood cells, leading to anemia. It is important to discuss potential side effects with your healthcare provider when starting a new medication, as they can provide guidance on managing or mitigating any adverse effects on your blood health.
Symptoms and Diagnosis
Fatigue and weakness
One common symptom of chronic blood disorders is fatigue and weakness. This is due to the inadequate delivery of oxygen to the body’s tissues caused by anemia or abnormal blood clotting. If you find yourself frequently feeling tired or lacking energy, it is important to consult with your healthcare provider to determine the underlying cause and receive appropriate treatment.
Abnormal bleeding or bruising
Another symptom of chronic blood disorders is abnormal bleeding or bruising. This can manifest as prolonged bleeding from small cuts or bruises that appear without any significant impact. Additionally, you may notice frequent nosebleeds or heavy menstrual bleeding. If you experience these symptoms, it is crucial to discuss them with your healthcare provider to investigate the potential presence of a chronic blood disorder.
Tests for diagnosis
To diagnose a chronic blood disorder, your healthcare provider may order a series of tests. These tests can include blood tests to measure the levels of various blood components, such as red blood cells, platelets, and clotting factors. Additionally, genetic testing may be conducted to identify any inherited mutations associated with certain chronic blood disorders. These diagnostic tests are essential in determining the specific condition and guiding appropriate treatment plans.
Treatment Options
Medication
Medication is a common treatment option for many chronic blood disorders. Depending on the specific condition, medications may be prescribed to address anemia, manage clotting factors, suppress autoimmune responses, or prevent blood clots. It is crucial to follow the prescribed medication regimen and regularly communicate with your healthcare provider to ensure optimal treatment outcomes.
Blood transfusions
In some cases, blood transfusions may be necessary to treat chronic blood disorders. Blood transfusions involve receiving healthy blood components, such as red blood cells or platelets, from a donor. This can help replenish deficient blood components and improve overall blood health. Transfusions may be needed on an ongoing basis for some individuals with chronic blood disorders.
Surgery
In certain situations, surgery may be recommended as a treatment option for chronic blood disorders. For example, individuals with severe cases of hemophilia may require joint surgery to repair damage caused by repeated bleeding into joints. Surgical interventions can help improve quality of life and reduce complications associated with chronic blood disorders. It is essential to discuss the potential benefits and risks of surgery with your healthcare provider before making any decisions.

Lifestyle Changes
Healthy diet and exercise
Maintaining a healthy lifestyle is crucial for managing chronic blood disorders. A balanced diet that includes iron-rich foods, such as leafy greens, lean meats, and fortified cereals, can help address anemia or other nutrient deficiencies. Regular exercise, such as walking or swimming, can also benefit blood circulation and overall health. Consult with your healthcare provider or a registered dietitian for personalized dietary and exercise recommendations.
Avoiding certain activities
Depending on the type and severity of your chronic blood disorder, it may be necessary to avoid certain activities that can increase the risk of bleeding or injury. These activities may include contact sports, heavy lifting, or participating in situations where there is a higher risk of accidents. It is important to discuss any concerns or limitations with your healthcare provider to ensure your safety and wellbeing.
Regular check-ups
Regular check-ups are vital for monitoring the progress of your chronic blood disorder and making any necessary adjustments to your treatment plan. These appointments allow your healthcare provider to assess your blood levels, address any concerns or complications, and provide ongoing guidance and support. Keeping up with regular check-ups can help prevent or manage potential complications associated with chronic blood disorders.
Managing Pain and Discomfort
Pain management techniques
Chronic blood disorders can sometimes cause pain and discomfort, especially if there are associated complications such as joint damage or blood clots. Your healthcare provider can recommend various pain management techniques, including over-the-counter or prescription pain medications, heat or cold therapy, and alternative therapies such as massage or relaxation techniques. It is important to communicate openly about your pain levels and work collaboratively with your healthcare team to develop an effective pain management plan.
Therapies such as acupuncture
Some individuals find complementary therapies, such as acupuncture, helpful in managing pain and discomfort associated with chronic blood disorders. Acupuncture involves the insertion of thin needles into specific points on the body to stimulate healing and provide pain relief. While not all chronic blood disorders may benefit from acupuncture, it can be a viable option for certain individuals. Consult with a licensed acupuncturist and inform them about your specific condition to determine if it may be beneficial for you.
Support from healthcare professionals
Living with a chronic blood disorder can be challenging, both physically and emotionally. It is important to seek support from your healthcare team, including doctors, nurses, and specialist healthcare professionals. They can provide guidance, answer your questions, and offer reassurance throughout your journey. Don’t hesitate to reach out to them when you need assistance or have concerns about managing pain and discomfort associated with your chronic blood disorder.
Emotional Support
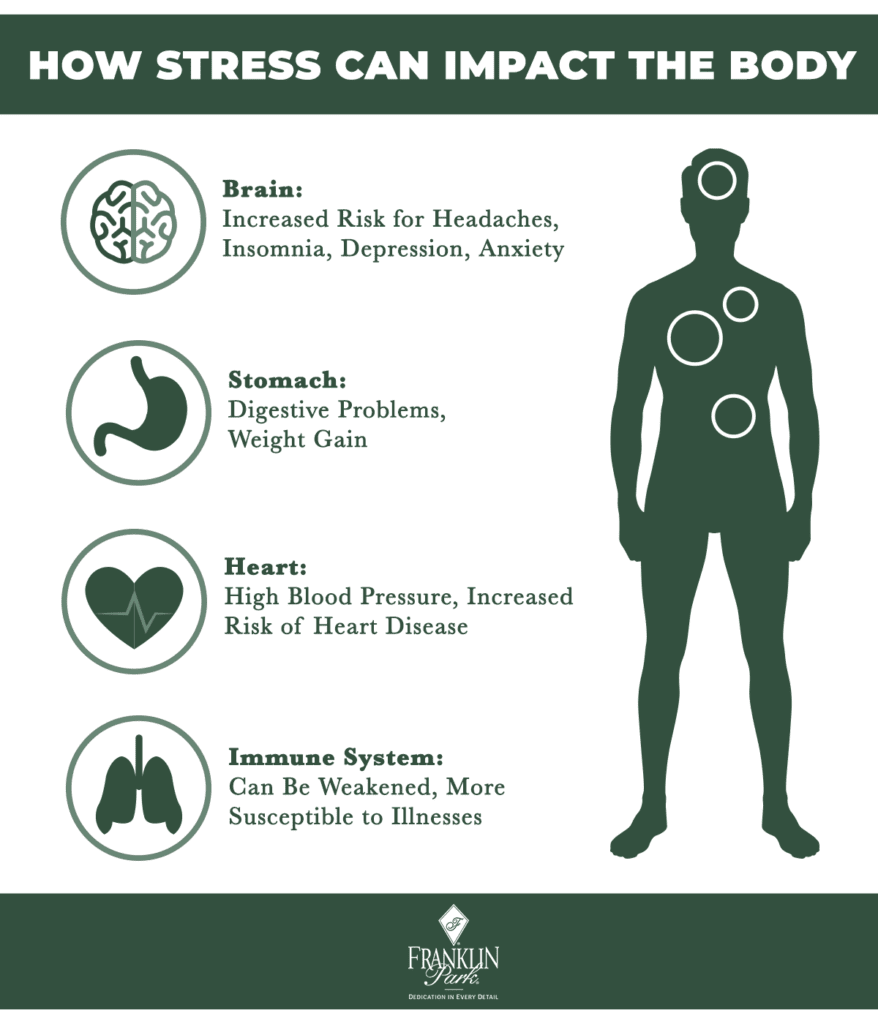
Dealing with stress and anxiety
Managing a chronic blood disorder can sometimes lead to increased stress and anxiety. It is essential to find healthy coping mechanisms to deal with these emotions. Techniques such as deep breathing exercises, mindfulness meditation, or engaging in hobbies and activities you enjoy can help reduce stress and promote a positive mindset. If you find that stress and anxiety are becoming overwhelming, consider seeking support from a mental health professional who can provide guidance and strategies for managing these emotions.
Support from friends and family
Building a support network with friends and family members who understand and empathize with your experiences can be invaluable. They can provide emotional support, help with practical tasks, and accompany you to medical appointments. Having loved ones by your side can make a significant difference in coping with the challenges that come with a chronic blood disorder.
Joining support groups
Connecting with others who share similar experiences can provide a unique sense of understanding and camaraderie. Consider joining support groups or online communities specifically for individuals with chronic blood disorders. These groups can offer a safe space to share concerns, ask questions, and learn from others who have firsthand knowledge of living with these conditions. Support groups can provide emotional support, helpful resources, and a sense of belonging.
Preventing Complications
Taking prescribed medication
Adhering to your prescribed medication regimen is essential for preventing complications associated with chronic blood disorders. Medications help manage symptoms, regulate blood components, or prevent blood clots. It is crucial to take medications as instructed by your healthcare provider, including the correct dosage and timing. If you have any concerns or experience side effects, promptly communicate with your healthcare team for guidance.
Regular monitoring of blood levels
Regular monitoring of blood levels is essential for assessing the effectiveness of treatment and identifying any changes or complications. Your healthcare provider will order blood tests to check various parameters, such as hemoglobin levels, platelet counts, or clotting factors. By monitoring these levels, your healthcare team can make necessary adjustments to your treatment plan and intervene early to prevent or manage complications associated with chronic blood disorders.
Taking necessary precautions
Certain precautions can help reduce the risk of complications associated with chronic blood disorders. This may include wearing protective gear, such as helmets or knee pads, when participating in activities that carry a higher risk of injury. It is also important to inform healthcare providers about your condition before undergoing any medical or dental procedures to ensure appropriate measures are taken to minimize the risk of bleeding or other complications.
Financial Considerations
Insurance coverage
Dealing with chronic blood disorders can involve significant healthcare expenses. Understanding your health insurance coverage is crucial to ensure you can access the necessary medications, treatments, and ongoing care. Review your insurance policy and speak with an insurance representative to clarify coverage details related to chronic blood disorders. It is essential to be aware of any deductibles, copayments, or limitations that may impact your financial responsibilities.
Cost of medications and treatments
Prescription medications, blood transfusions, and surgical procedures can incur substantial costs. It is important to have a clear understanding of the potential financial implications of managing your chronic blood disorder. Research drug assistance programs or initiatives that may provide financial support for specific medications. Additionally, inquire about potential financial aid or grant opportunities offered by non-profit organizations that focus on supporting individuals with chronic blood disorders.
Seeking financial assistance
If the financial burden associated with managing your chronic blood disorder becomes overwhelming, consider seeking financial assistance. Many charitable foundations and organizations offer financial aid to individuals with chronic illnesses who are struggling to cover medical expenses. Research and reach out to these resources to determine if they can provide support and alleviate some of the financial strain.
Importance of Communication
Openly discussing symptoms with healthcare providers
Open and honest communication with your healthcare provider is vital for effectively managing chronic blood disorders. It is essential to share any changes or worsening of symptoms, new concerns, or potential side effects from medications. Your healthcare provider relies on this information to make informed decisions about your treatment and ensure the best possible care. Regularly check in with your healthcare provider and actively engage in discussions about your symptoms.
Informing family and friends
Educating your family and friends about your chronic blood disorder can help them understand your condition better and provide appropriate support. By providing essential information about your diagnosis, treatment plan, and potential complications, you enable your loved ones to be more empathetic and knowledgeable allies. Encourage open dialogue and let them know how they can assist you during challenging times.
Educating others about the condition
Raising awareness about chronic blood disorders is crucial not only for individuals living with these conditions but also for the broader community. Educate others about the signs, symptoms, and challenges associated with chronic blood disorders. By increasing awareness, you contribute to a more understanding and supportive society. Consider participating in advocacy events, sharing information on social media, or joining organizations dedicated to spreading awareness about chronic blood disorders.

