Living with Rheumatoid Arthritis can be challenging, but understanding the disease and how to manage it is essential to maintaining a good quality of life. From the symptoms you may experience to the various treatment options available, this article aims to provide you with the necessary knowledge to navigate life with Rheumatoid Arthritis. Whether you have recently been diagnosed or have been living with the condition for some time, this article will help you gain a better understanding of what to expect and how to effectively manage the challenges that may arise.
What is Rheumatoid Arthritis?
Rheumatoid arthritis (RA) is a chronic autoimmune disease that primarily affects the joints. Unlike osteoarthritis, which is caused by wear and tear on the joints, RA occurs when the immune system mistakenly attacks the body’s own healthy tissues, leading to inflammation in the joints. This inflammation can cause pain, stiffness, and swelling, and if left untreated, can lead to joint deformity and disability. RA can also affect other parts of the body, such as the lungs, heart, and blood vessels.
Definition of Rheumatoid Arthritis
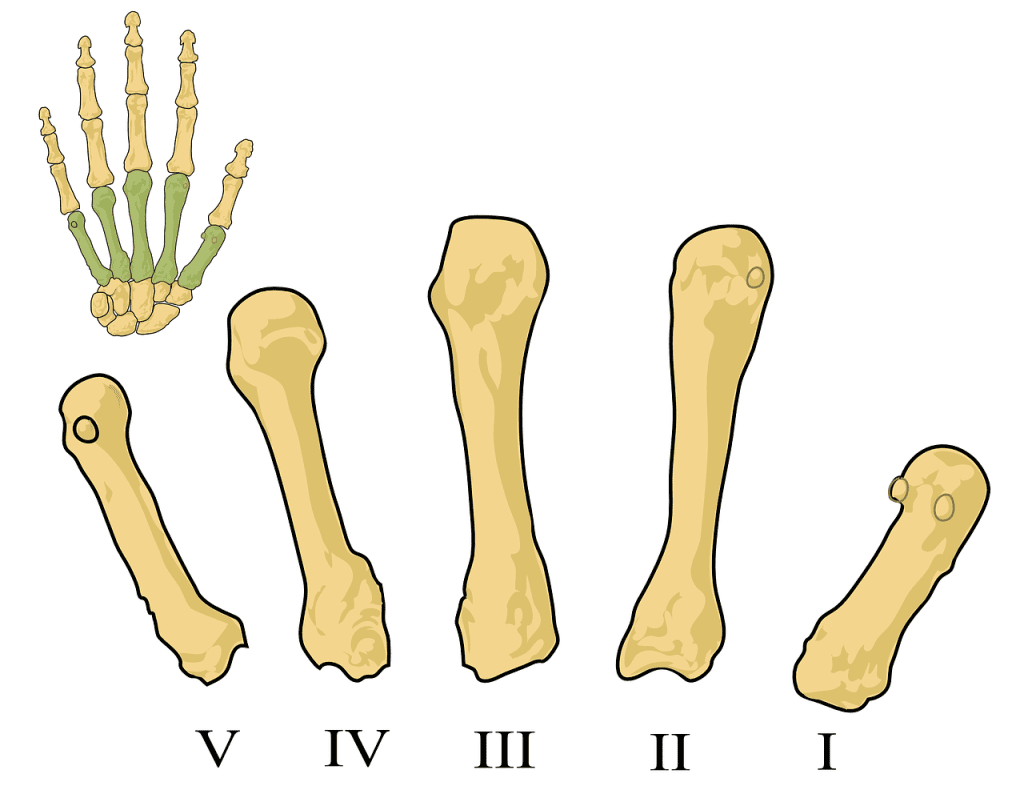
Rheumatoid arthritis is a systemic autoimmune disease that primarily targets the joints, leading to chronic inflammation and damage. It is characterized by the presence of autoantibodies, such as rheumatoid factor (RF) and anti-cyclic citrullinated peptide (anti-CCP) antibodies, which are markers of the disease. RA typically affects the small joints in the hands and feet symmetrically, although it can also involve larger joints in the body. It often presents with morning stiffness, joint pain, and swelling that lasts for at least six weeks.
Causes of Rheumatoid Arthritis
The exact cause of RA is unknown, but it is believed to be a combination of genetic and environmental factors. Certain genes, such as the HLA-DRB1 gene, have been associated with an increased risk of developing RA. Environmental triggers, such as smoking, infections, and hormonal changes, can also play a role in the development of the disease. It is thought that these triggers can activate the immune system, leading to the formation of autoantibodies and the subsequent inflammatory response in the joints.
Symptoms of Rheumatoid Arthritis
The symptoms of RA can vary from person to person, but common symptoms include joint pain, swelling, and stiffness, especially in the morning or after periods of inactivity. Other symptoms may include fatigue, low-grade fever, loss of appetite, and weight loss. RA can also cause joint deformity and reduced mobility if left untreated. Additionally, some individuals with RA may experience extra-articular manifestations, such as lung inflammation, heart complications, or eye problems.
Diagnosis and Medical Tests
Visiting a Rheumatologist
If you suspect you may have RA, it is essential to consult with a rheumatologist, a specialist who focuses on the diagnosis and treatment of arthritis and other rheumatic diseases. During your visit, the rheumatologist will perform a thorough physical exam to assess your joint inflammation, range of motion, and overall disease activity. They may also ask about your medical history, family history of autoimmune diseases, and any symptoms you’re experiencing.
Blood Tests for Rheumatoid Arthritis
Blood tests are crucial for confirming the diagnosis of RA and assessing disease activity. The rheumatologist may order tests to detect the presence of autoantibodies, such as rheumatoid factor (RF) and anti-CCP antibodies. These antibodies are often elevated in individuals with RA. Additionally, blood tests can help identify markers of inflammation, such as erythrocyte sedimentation rate (ESR) and C-reactive protein (CRP) levels.
Imaging Tests for Rheumatoid Arthritis
Imaging tests, such as X-rays, ultrasound, or magnetic resonance imaging (MRI), may be used to evaluate the extent of joint damage and monitor disease progression over time. These tests can help visualize changes in the joints, such as erosion, swelling, and narrowing of the joint space, which are indicative of RA. Imaging can also assist in ruling out other conditions that may mimic RA symptoms.
Other Diagnostic Methods
In some cases, the rheumatologist may recommend additional tests, such as joint aspirations or biopsies, to help confirm the diagnosis or exclude other possible causes of joint inflammation. Joint aspirations involve removing fluid from the affected joint for analysis, while biopsies involve taking a small sample of tissue for examination under a microscope.
Treatment Options
Medications for Rheumatoid Arthritis
Medications play a crucial role in managing RA symptoms, slowing down disease progression, and reducing joint damage. Nonsteroidal anti-inflammatory drugs (NSAIDs) can help alleviate pain and inflammation, while disease-modifying antirheumatic drugs (DMARDs) are used to suppress the immune system and prevent further joint damage. Biologic response modifiers, a type of DMARD, specifically target the underlying mechanisms of RA and can be highly effective in controlling symptoms. Corticosteroids may also be prescribed to manage flare-ups and provide short-term relief.
Physical Therapy and Exercise
Physical therapy and regular exercise are essential components of RA treatment. A physical therapist can teach you specific exercises and techniques to improve joint strength, flexibility, and mobility. These exercises can help reduce pain, maintain joint function, and enhance overall quality of life. It is important to work with a professional who understands the unique needs and limitations of individuals with RA.
Lifestyle Changes
Making lifestyle changes can significantly impact the management of RA symptoms. This includes adopting a balanced and nutritious diet, getting regular exercise, managing stress levels, and getting adequate rest and sleep. It may be helpful to maintain a healthy weight to alleviate pressure on the joints and reduce inflammation. Additionally, incorporating stress-reducing activities, such as yoga or meditation, can provide relief from both physical and emotional symptoms.
Surgical Options
In severe cases of RA where joint damage is extensive and conservative treatments have not been effective, surgery may be considered. Joint replacement surgery, such as hip or knee replacement, can provide relief and restore mobility in affected joints. Synovectomy, a procedure to remove inflamed joint lining, and tendon repair surgeries are also possible options. Surgery should be discussed thoroughly with a rheumatologist and orthopedic surgeon to weigh the benefits and risks involved.

Managing Flare-ups and Pain
Identifying Triggers
Flare-ups in RA can be unpredictable, but certain triggers may contribute to increased disease activity. It is crucial to identify and avoid these triggers whenever possible. Common triggers include stress, illness, certain foods, overexertion, and exposure to cold weather. Keeping a journal to track your symptoms and potential triggers can help identify patterns and make necessary lifestyle adjustments.
Tips for Managing Flare-ups
During a flare-up, it is important to listen to your body and prioritize self-care. Resting the affected joints and providing them with support, such as with splints or braces, can help reduce inflammation and alleviate pain. Applying hot or cold packs, taking over-the-counter pain relievers, or using prescribed medications as directed can also provide relief. Communicating with your healthcare team about your flare-ups is essential to ensure timely and appropriate management.
Pain Management Strategies
Managing pain is a crucial aspect of living with RA. In addition to medications, there are various strategies for pain management that can be beneficial. Heat therapy, such as warm baths or heating pads, can help relax muscles and relieve joint stiffness. Cold therapy, such as ice packs or cold compresses, can reduce inflammation and numb pain. Transcutaneous electrical nerve stimulation (TENS) devices and acupuncture are alternative options that can provide pain relief for some individuals.
Coping with Emotional and Mental Health
Impact of Rheumatoid Arthritis on Mental Health
Living with a chronic condition like RA can take an emotional toll. The pain and physical limitations associated with the disease can lead to feelings of frustration, helplessness, and even depression or anxiety. It is important to recognize and address the emotional and mental health aspect of RA to maintain overall well-being. Seeking support from loved ones, joining support groups, and seeking professional counseling or therapy can be beneficial for managing these challenges.
Seeking Support from Loved Ones
Building a strong support system is crucial for individuals living with RA. Educate your loved ones about the disease and how it affects you, so they can better understand your needs and provide support. Their emotional support, assistance with daily activities, and understanding during flare-ups can greatly contribute to your overall well-being. Open communication and sharing your feelings and concerns can help alleviate the burden and foster healthy relationships.
Counseling and Therapy
Professional counseling or therapy can be invaluable in managing the emotional and mental health aspects of RA. A mental health professional can help you develop coping strategies, provide tools for managing stress and anxiety, and offer a safe space to discuss and explore your feelings about the disease. Cognitive-behavioral therapy (CBT) has been shown to be particularly effective in helping individuals with chronic illnesses develop adaptive strategies and improve their overall quality of life.
Maintaining a Healthy Diet
Foods to Include in a Rheumatoid Arthritis Diet
Although there is no specific diet that can cure RA, certain foods may have anti-inflammatory properties and promote overall health. Including foods rich in omega-3 fatty acids, such as fatty fish, walnuts, and flaxseeds, can help reduce inflammation. Antioxidant-rich foods, including berries, spinach, and turmeric, may also provide protection against inflammation. Additionally, incorporating lean proteins, whole grains, and plenty of fruits and vegetables can ensure a well-balanced and nutritious diet.
Foods to Avoid
While there is no one-size-fits-all approach when it comes to dietary restrictions for RA, some individuals may find that certain foods can trigger inflammation or worsen symptoms. Common culprits include processed foods, saturated fats, refined sugars, and excessive alcohol consumption. It may be helpful to keep a food diary and note any adverse reactions to specific foods. Consulting with a registered dietitian who specializes in autoimmune conditions can provide personalized guidance.
Weight Management
Maintaining a healthy weight is essential for managing RA symptoms, as excess weight can put additional strain on the joints and worsen inflammation. Incorporating regular exercise and following a balanced diet can contribute to weight management. It is important to consult with a healthcare professional or a registered dietitian to create a plan that suits your specific needs and takes into account any dietary restrictions or medications.
Assistive Devices and Home Modifications
Types of Assistive Devices
Assistive devices can help individuals with RA overcome physical limitations and maintain independence. For example, using ergonomic tools and utensils can make daily tasks such as cooking and writing more manageable. Splints or braces can provide support and alleviate pain in affected joints. Canes, walkers, or mobility aids can assist with balance and mobility. It is important to work with an occupational therapist who can assess your unique needs and recommend appropriate assistive devices.
Home Modifications for Easier Living
Modifying your home environment can make daily activities more accessible and manageable. Simple adjustments, such as installing grab bars in the bathroom, using nonslip mats in the shower, and raising toilet seat height, can greatly improve safety and ease of use. Lever-style door handles, easy-to-reach shelving, and adaptive kitchen utensils can also enhance functionality. Consult with an occupational therapist or home remodeling professional to assess your specific needs and make appropriate modifications.
Alternative Therapies and Complementary Treatments
Acupuncture
Acupuncture, a traditional Chinese medicine practice, involves inserting thin needles into specific points on the body. It is believed to promote the flow of qi (energy) and balance the body’s systems. Some individuals with RA find acupuncture helpful in reducing pain, stiffness, and inflammation. However, it is essential to consult with a qualified and experienced acupuncturist to ensure safety and effectiveness.
Chiropractic Care
Chiropractic care focuses on the musculoskeletal system and the spine’s alignment. Chiropractors use manual adjustments and other techniques to improve joint function and alleviate pain. While some individuals with RA may benefit from chiropractic care, it is crucial to communicate and work closely with both your rheumatologist and chiropractor to ensure a coordinated and safe approach to treatment.
Massage Therapy
Massage therapy can provide relief from muscle tension, joint stiffness, and pain associated with RA. The manipulation of soft tissues and gentle stretching can enhance circulation, relax muscles, and improve range of motion. It is important to choose a qualified massage therapist who has experience working with individuals with RA and understands the specific needs and limitations associated with the disease.
Herbal Supplements
Herbal supplements, such as turmeric, ginger, and fish oil, are often touted for their anti-inflammatory properties. While some individuals may find symptom relief from these supplements, it is crucial to approach their use with caution. Herbal supplements can interact with medications and have potential side effects. It is important to consult with a healthcare professional, such as a rheumatologist or an integrative medicine specialist, before incorporating any supplements into your treatment plan.
The Importance of Regular Check-ups
Monitoring Disease Progression
Regular check-ups with your rheumatologist are essential in managing RA. These visits allow your healthcare provider to assess disease activity, monitor the effectiveness of medications, and make any necessary adjustments to your treatment plan. Blood tests and imaging may be ordered periodically to evaluate disease progression and detect any signs of joint damage. Staying proactive and keeping regular appointments can help prevent complications and optimize your long-term outlook.
Adjusting Treatment Plans
RA is a complex and dynamic disease, and treatment plans may need to be adjusted over time. As the disease progresses or your symptoms change, your rheumatologist may recommend modifications to your medication regimen or suggest trying new therapies. Regular check-ups provide an opportunity for open communication with your healthcare team, allowing them to better understand your needs and tailor your treatment accordingly.
Preventing Complications
Regular check-ups also help identify potential complications or comorbidities associated with RA. By closely monitoring your disease activity and overall health, your rheumatologist can identify and address any emerging issues. For example, individuals with RA are at an increased risk of developing cardiovascular disease, osteoporosis, and infections. By staying vigilant and attending regular appointments, you can work together with your healthcare team to minimize these risks and promote overall well-being.
Living a Fulfilling Life with Rheumatoid Arthritis
Setting Realistic Goals
Living with RA does not mean you have to give up on your dreams and aspirations. However, it is important to set realistic goals that take into account your physical limitations and the unpredictable nature of the disease. Focus on what you can do rather than what you can’t, and adapt your goals accordingly. Celebrate small victories and learn to prioritize self-care and balance to ensure a fulfilling and sustainable life with RA.
Adapting Hobbies and Activities
Having RA may require some modifications to your hobbies and activities, but it doesn’t mean you have to give them up entirely. Explore adaptive techniques or equipment that can help you continue doing what you love. For example, if you enjoy gardening, consider using ergonomic tools or raised garden beds to reduce strain on your joints. If you are a music lover, consider playing a different instrument that puts less stress on your hands or explore singing or music production. Be creative and flexible in finding ways to adapt your interests to accommodate your physical needs.
Maintaining Social Connections
Living with a chronic illness like RA can sometimes feel isolating, but maintaining social connections is crucial for your well-being. Stay engaged with friends, family, and your community. Reach out for support when needed, and don’t hesitate to share your experiences and ask for understanding. Joining support groups or connecting with other individuals living with RA can provide a sense of community and shared understanding. Being surrounded by a supportive network can positively impact your emotional and mental health, making the journey with RA more manageable.

